Background and Objectives: Experiences of psychological trauma are common among primary care patient populations, and adversely affect patients’ health and health care utilization. Trauma-informed care (TIC) is a framework for identifying and responding to patients’ experiences of psychological trauma to avoid retraumatization. The purpose of this study was to evaluate the current state of TIC training in family medicine residency programs in the United States in order to identify opportunities for and barriers to TIC training.
Methods: Items addressing the four core domains of TIC were incorporated into the 2017 Council of Academy Family Medicine Educational Research Alliance (CERA) survey of program directors. The items assessed the presence, content, and sufficiency of TIC curriculum, as well as barriers to further integration of TIC training.
Results: Approximately 50% of programs responded to the survey. Of 263 respondents, 71 (27%) reported TIC training in their curriculum, but the majority devoted less than 5 hours annually to core content. The content most commonly addressed recognizing signs of trauma, most frequently using didactic formats. Overall, just over one-half of the programs reported that their curriculum met patients’ TIC needs “somewhat” (48.5%) or “a great deal” (4.6%). Lack of a champion followed by lack of time were the most commonly cited barriers to integrating TIC training.
Conclusions: Despite the acknowledged importance of effects of trauma in health care, this study identified insufficient exposure to training in the core TIC domains in family medicine residency programs, underscoring a need for greater integration of TIC training during residency.
Experiences of trauma that are physically or emotionally harmful or life-threatening can have long-term effects on physical, emotional, and social well-being.1 Traumatic experiences, including interpersonal violence, community violence, combat exposure, tragic deaths, and adverse childhood experiences, can impact mental and physical health across the lifespan and interfere with self-care and access to or use of health care services.1-3 In addition, unaddressed trauma can lead to a cascade of negative coping strategies and distress, potentially resulting in a cross-generational cycle of trauma vulnerability. In health care settings, the adverse consequences of traumatic experiences can be mitigated through recognition and responding sensitively to the particular needs of patients who have experienced trauma.4-6
Trauma-informed care (TIC) is an approach that takes patients’ experiences of trauma into account in clinical care delivery, along with an understanding of scope and impacts of trauma exposures among the patient population. It requires skills in assessing for and responding to patients’ disclosures of trauma exposures and related symptoms, and utilizing practices designed to address—and not exacerbate—trauma symptoms. The Substance Abuse and Mental Health Services Administration (SAMHSA) characterizes four key elements of TIC approaches: “realizing the widespread impact of trauma and understands potential paths for recovery; recognizing the signs and symptoms of trauma in clients, families, staff, and others involved with the system; responding by fully integrating knowledge about trauma into policies, procedures, and practices; and seeking to actively resists retraumatization.”1 Knowledge of a patient’s trauma experiences can improve provider sensitivity to the patient, avoid retraumatizing, and inform understanding of symptom development and management.5-6 An example is found in the recent outbreak of Ebola virus disease, where subsequent screening conducted without adequate sensitivity to patients’ trauma-related experiences could unintentionally exacerbate posttraumatic responses and inhibit sufficient disclosure and help-seeking.7 National professional organizations and recommendations from experts have called for primary care providers to be more trauma-informed and address patient experiences of trauma across the lifespan.6-9
Widespread recognition of individual- and community-level trauma experiences as a social determinant of health that affects health behaviors, including access to care and health outcomes, is relatively new. Recommendations for assessment of patient trauma experiences have expanded over the last decade with limited implementation to date.8-9 New initiatives typically pose challenges to existing programs, and already-saturated training needs may be barriers to implementing TIC approaches in clinical care and residency training programs.10-11 Further, medical education teaching models have not fully adapted to the current complexity of our health care environment.12 The purpose of this study was to assess the current state of TIC-related training in family medicine residency programs in order to identify gaps in training, areas for further development, and barriers to further implementation of TIC-related training.
To assess the current state of TIC-related training in US family medicine residency programs, we developed measurement items that were included in the 2017 survey of family medicine residency program directors conducted by the Council of Academic Family Medicine Educational Research Alliance (CERA).13 The TIC-specific items were based on approaches as defined by SAMHSA. The CERA Steering Committee piloted the survey items in a sample of family medicine educators who were not included in the final survey sample. Data were collected from September 2017 to October, 2017. The Institutional Review Board of the American Academy of Family Physicians approved the project, and the Institutional Review Board of the University of Pennsylvania granted exemption to the analysis of survey data.
The sampling frame for the survey was directors of all US family medicine residency programs that are accredited by the Accreditation Council for Graduate Medical Education (ACGME). Programs were identified by the Association of Family Medicine Residency Directors (AFMRD). Invitations to participate in the survey along with a link to the online survey platform were sent to program directors by email, with up to five follow-up emails to encourage participation.
Programs were asked to report whether their curriculum included any TIC elements, perceived sufficiency in meeting trauma-related patient needs, and barriers to integrating or expanding TIC into their residency curriculum. Programs that reported any TIC curriculum were further asked to estimate the number of hours dedicated to TIC curriculum and to characterize the TIC-related topics and teaching modalities included in their curricula. The analyses included descriptions of: (1) the proportion of programs reporting any TIC elements in their curricula and number of hours among those with any TIC, (2) the proportion of programs indicating each level of TIC program sufficiency and implementation barriers (scale of 1-4), (3) comparison of mean sufficiency and barriers scores between programs with and without any TIC curricula, and (4) the proportion of programs with any TIC elements that included each of the teaching topics and modalities. Analyses were performed using IBM SPSS Statistics software, version 24.
Respondent Program Characteristics
The survey was sent to 503 out of 526 US family medicine residency program directors; the remaining 23 programs had previously opted out of CERA surveys or were unable to be reached via email. A total of 267 program directors responded to the survey, but four respondents did not complete TIC-specific items on the survey, resulting in a response rate of 52.3% (263/503) for the TIC items.
Among the 263 programs, the majority (58.2%) were community-based, university-affiliated programs, while 17.5% were university-based, and 17.1% community-based without a university affiliation (Table 1). Ten programs were military-based and nine had other affiliations (including combinations of university-, community-, and military-based and teaching health centers). Nearly half (47.5%) of the programs supported between 19 and 31 residents. Twenty-seven percent of the programs reported TIC training as part of their program’s curriculum in some way. Among programs with any TIC curriculum, most (72.9%) had up to 5 hours/year; nine (19.9%) programs had more than 10 hours of TIC training per year. The included programs were similar to the full sampling frame in both geographic region and residency size, although with slightly more representation from more western states and less from the eastern part of the country. We did not find any statistically significant differences in presence of TIC curriculum by program characteristics (analysis not shown in table).
Sufficiency of and Barriers to TIC Integration
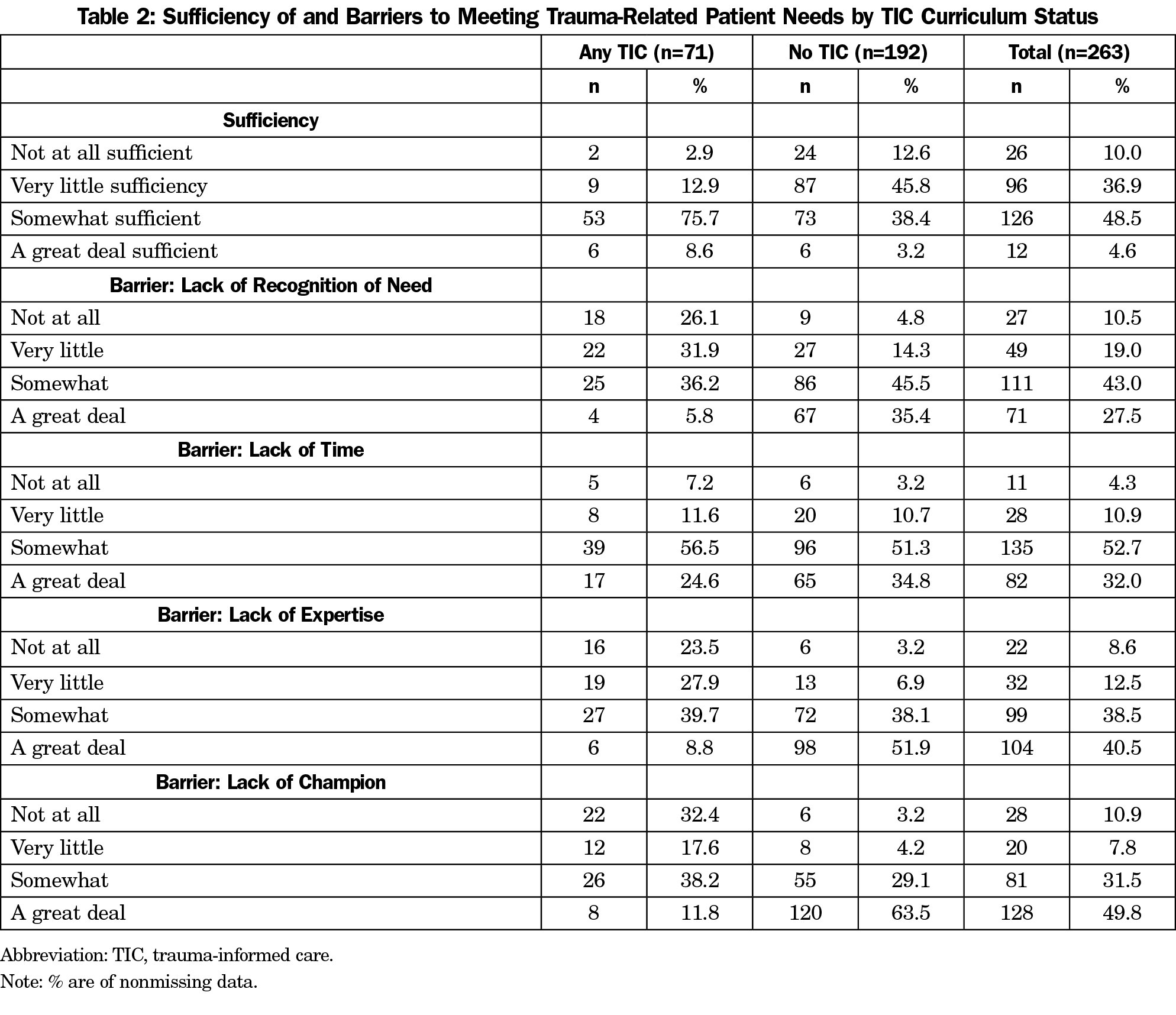
Perceived sufficiency in meeting trauma-related patient needs and barriers to integration of TIC-related curriculum were assessed on a 4-point scale from 1 (“not at all”) to 4 (“a great deal”). Fifty-three percent of all programs (84.3% of those with any TIC curriculum and 41.6% of those without TIC curriculum) rated their program as “somewhat” or “a great deal” sufficient in meeting the trauma-related needs of patients. One in 10 programs (2.9% of those with any TIC, and 12.6% of those with no TIC) reported that their program was “not at all” sufficient in meeting patient trauma-related needs (Table 2). Only 8.6% of programs with any TIC curriculum and 3.2% of those with no TIC curriculum reported “a great deal” sufficient in meeting patients’ trauma-related needs.
Among the barriers to integrating or expanding TIC training in the residency curriculum, “lack of a trauma-informed care practice champion” was rated as the most common (“a great deal”) barrier for the most programs (49.8%), with over 80% of programs reporting that this was at least “somewhat” of a barrier (Table 2). The factor most commonly identified as at least “somewhat” of a barrier to TIC integration was lack of time, with only 4.3% of programs indicating that this was “not at all” a barrier. Lack of recognition of need for TIC-related curriculum was indicated as a barrier “somewhat” or “a great deal” by 42% of programs with any TIC-related curriculum and 81% of those with no TIC-related curriculum. Ninety percent of programs with no TIC-related curriculum (and 49% of those with any TIC-related curriculum) indicated that lack of a local TIC champion was “a great deal” of a barrier to TIC curriculum implementation.
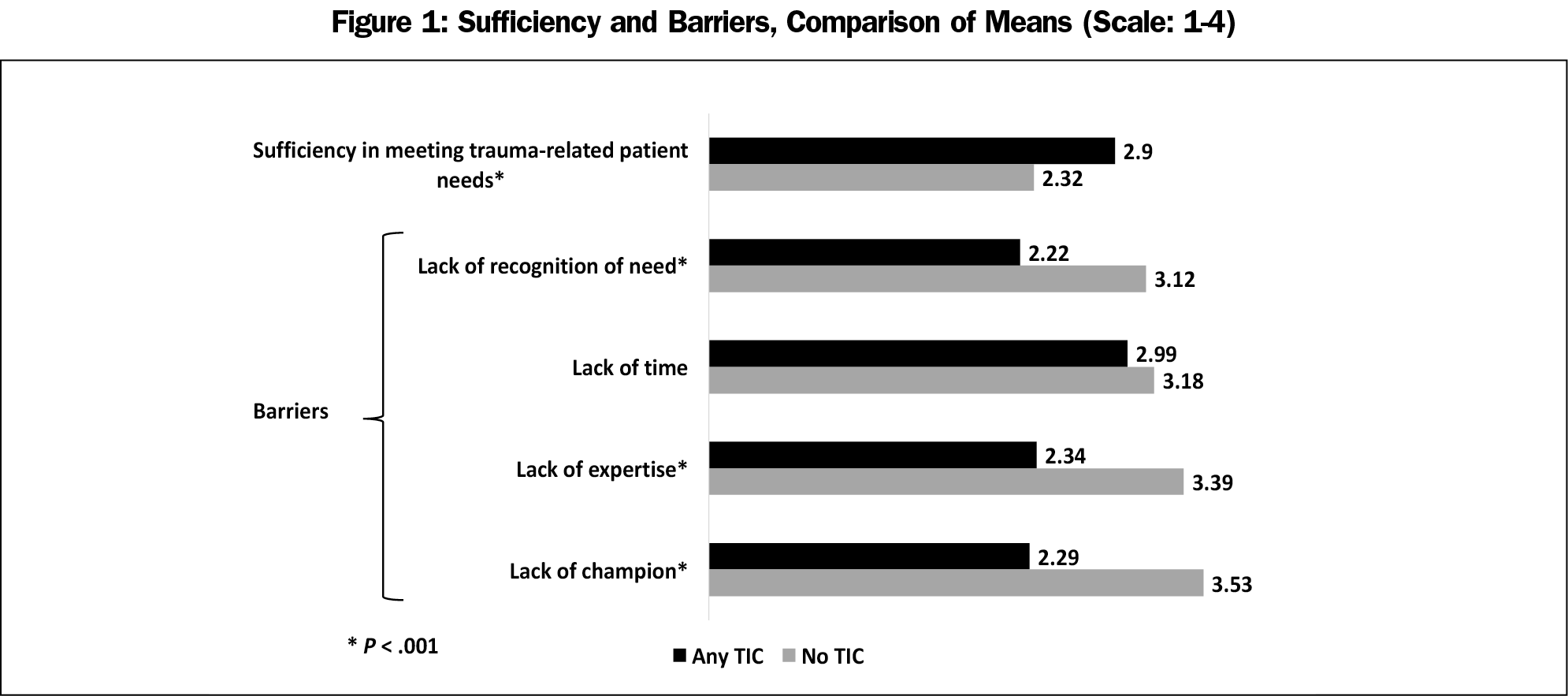
Mean scores for perceived sufficiency in meeting trauma-related patient needs were higher among programs with any TIC curriculum versus those with no TIC curriculum (2.9 vs 2.32; Figure 1). Mean scores for extent of each of the categories of barriers were higher for those with no TIC curriculum than with any TIC curriculum, except for lack of time, for which there was no statistically significant difference between the two groups. Among the “any TIC” group, lack of time was the most highly-rated barrier and lack of recognition of need as the lowest-rated barrier. Among the “no TIC” group, lack of a TIC champion was identified as the highest-rated barrier, with lack of recognition of need as the lowest.
TIC Curriculum Topics and Activities Among Programs Reporting Any TIC Curriculum
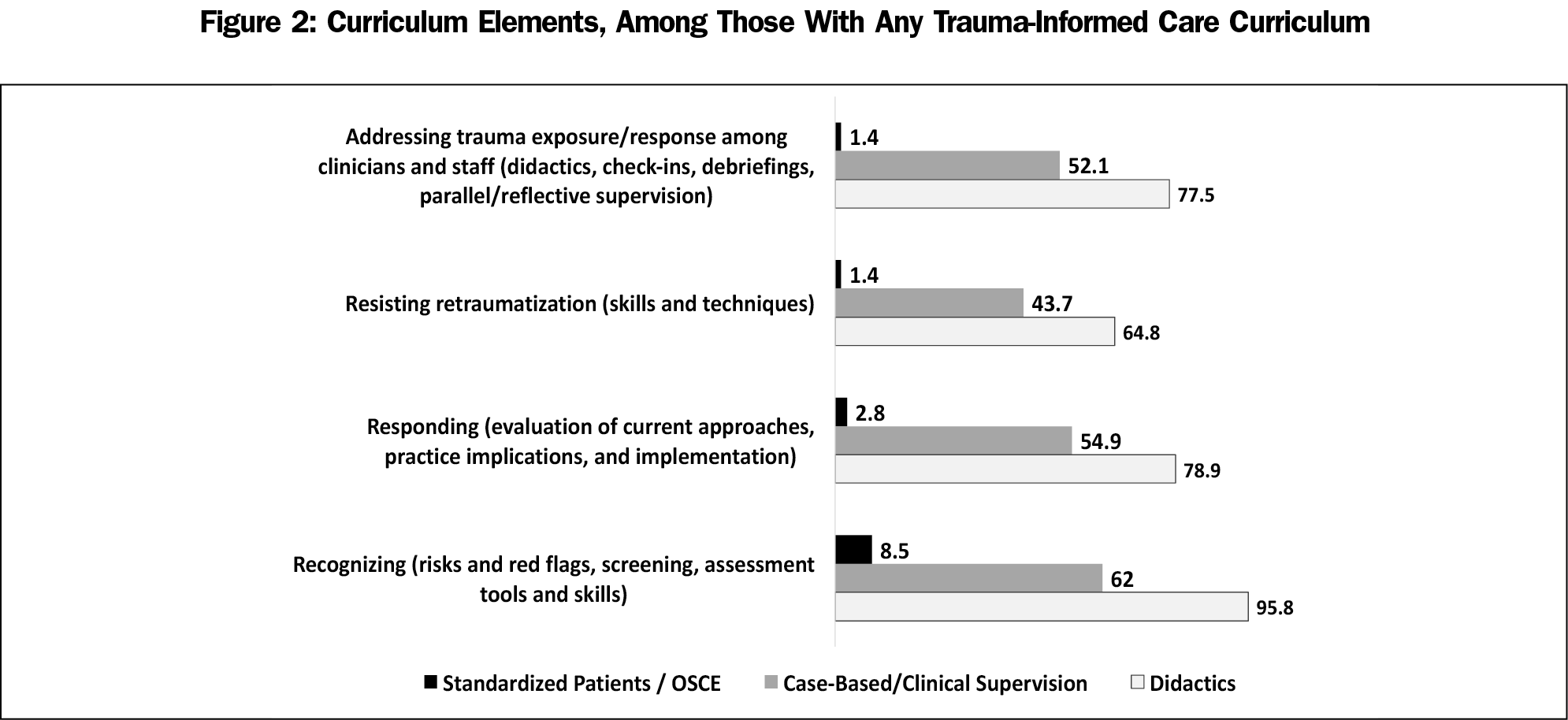
Among the programs with any TIC curriculum (n=71), all but one (98.6%) reported at least one of the curricular activities, with didactics being the most frequently reported (97.2%) TIC-related activity (Figure 2). The majority of the programs (69%) reported case-based or clinical supervision activities, and fewer than one in ten (8.5%) programs reported using standardized patients or objective structured clinical examination (OSCE) for TIC curricular activities. Nearly all of the described TIC content areas were covered among the activities by all programs, with the most (98.6%) covering recognizing, followed by responding (88.7%), addressing among clinicians/staff (88.7%), and resisting (74.6%).
This study evaluated the presence and sufficiency of, as well as barriers to inclusion of TIC training in family medicine residency programs. Most of the programs do not have TIC curricular elements for residents, and nearly all programs (>95%) reported room for improvement in meeting patients’ TIC-related needs. Lack of a local champion and lack of time were barriers to TIC integration for more than 80% of programs; more than 70% also reported lack of recognition of need as implementation barriers. Not surprisingly, programs without any current TIC curriculum rated their program as less sufficient in meeting patients’ trauma-related needs and as facing higher levels of barriers to curricular implementation compared with programs with existing content. However, it is noteworthy that over 41% of those without any TIC curriculum indicated their program was at least somewhat sufficient in meeting patients’ trauma-related needs. Among programs with any TIC-related curriculum, most utilized didactic methods most commonly focused on recognizing trauma-related symptoms. This reliance on didactic methods to recognize symptoms alone may be insufficient for learners to acquire needed knowledge and skills.12
Study findings related to the penetration of TIC curriculum in family medicine residency programs should be considered in the context of a 50% response rate. We do not know the extent of TIC curriculum among nonresponders. The lack of association between program characteristics and TIC may be due to limited sample size or limited information about program characteristics, for example, programs serving a population with high rates of trauma exposure (eg, refugees, sexual assault survivors). Additionally, although surveys were completed by program directors who likely have strong knowledge of their curriculum, it is possible that another program representative may have had different responses to the survey items. Self-report data are always subject to social desirability bias which may lead to an overestimation of the true penetration of TIC curricular components in our study. Survey respondents were not asked to include their individual or program identities, which may help mitigate social desirability bias.
Despite these methodological limitations, study findings reveal important gaps training in patients’ trauma-related needs, and therefore a need for greater attention and response to trauma experiences and related symptoms among both patients and clinical providers and staff. It is crucial to ensure trainees’ knowledge of the impacts of trauma on patients’ health and the potential health benefits of appropriately addressing trauma experience in the clinical setting. Further, TIC approaches can also help improve overall patient-centered care delivery.10
Our findings also point to areas of knowledge gap. More research is needed on approaches for successful integration of TIC training into existing behavioral health curricula. The study identified lack of a champion or time as primary barriers to implementation of TIC, and it is unknown whether programs had faculty with the expertise or training to provide leadership needed for integration of TIC training into existing longitudinal curricula. Research is needed on existing best practices for TIC training within training programs. The mastery learning model is grounded in opportunities for knowledge and skill acquisition through purposeful practice, measurement of formative achievements, feedback and coaching, and thorough measurement of learner outcomes.14 This model is well suited to TIC training to prepare family medicine physicians to screen for trauma, recognize the signs and symptoms, and respond to patient care needs without retraumatizing. Physician readiness for TIC may be enhanced by the application of specific curricula including setting expectations for knowledge and skills, providing opportunities to practice newly acquired skills, and measuring learner outcomes.
Acknowledgments
Financial support for this study was provided to Dr Doubeni by Health Resources and Services Administration (HRSA) grant UH1HP29964. This article’s contents are solely the responsibility of the authors and do not necessarily represent the official views of the Health Resources and Services Administration or the US Department of Health and Human Services. The authors acknowledge the contributions of Andrea Bilger and Emily Paterson.
References
- Substance Abuse and Mental Health Services Administration. SAMHSA’s concept of trauma and guidance for a trauma-informed approach. Rockville, MD: SAMHSA; 2014.
- Cronholm PF, Forke CM, Wade R, et al. Adverse childhood experiences: expanding the concept of adversity. Am J Prev Med. 2015;49(3):354-361. https://doi.org/10.1016/j.amepre.2015.02.001
- Dube SR, Felitti VJ, Dong M, Giles WH, Anda RF. The impact of adverse childhood experiences on health problems: evidence from four birth cohorts dating back to 1900. Prev Med. 2003;37(3):268-277. https://doi.org/10.1016/S0091-7435(03)00123-3
- Green BL, Kaltman S, Frank L, et al. Primary care providers’ experiences with trauma patients: A qualitative study. Psychol Trauma. 2011;3(1):37-41. https://doi.org/10.1037/a0020097
- Machtinger EL, Cuca YP, Khanna N, Rose CD, Kimberg LS. From treatment to healing: the promise of trauma-informed primary care. Womens Health Issues. 2015;25(3):193-197. https://doi.org/10.1016/j.whi.2015.03.008
- Raja S, Hasnain M, Hoersch M, Gove-Yin S, Rajagopalan C. Trauma informed care in medicine: current knowledge and future research directions. Fam Community Health. 2015;38(3):216-226. https://doi.org/10.1097/FCH.0000000000000071
- Faherty LJ, Doubeni CA. Unintended consequences of screening for Ebola. Am J Public Health. 2015;105(9):1738-1739. https://doi.org/10.2105/AJPH.2015.302768
- Institute of Medicine. Clinical Preventive Services for Women: Closing the Gaps. Washington, DC: The National Academies Press; 2011.
- Green BL, Saunders PA, Power E, et al. Trauma-informed medical care: CME communication training for primary care providers. Fam Med. 2015;47(1):7-14.
- Raymond JR Sr, Kerschner JE, Hueston WJ, Maurana CA. The merits and challenges of three-year medical school curricula: time for an evidence-based discussion. Acad Med. 2015;90(10):1318-1323. https://doi.org/10.1097/ACM.0000000000000862
- Carek PJ, Anim T, Conry C, et al. Residency training in family medicine: A history of innovation and program support. Fam Med. 2017;49(4):275-281.
- McGaghie WC. Mastery learning: it is time for medical education to join the 21st century. Acad Med. 2015;90(11):1438-1441. https://doi.org/10.1097/ACM.0000000000000911
- Mainous AG III, Seehusen D, Shokar N. CAFM Educational Research Alliance (CERA) 2011 Residency Director survey: background, methods, and respondent characteristics. Fam Med. 2012;44(10):691-693.
- Cook DA, Brydges R, Zendejas B, Hamstra SJ, Hatala R. Mastery learning for health professionals using technology-enhanced simulation: a systematic review and meta-analysis. Acad Med. 2013;88(8):1178-1186. https://doi.org/10.1097/ACM.0b013e31829a365d

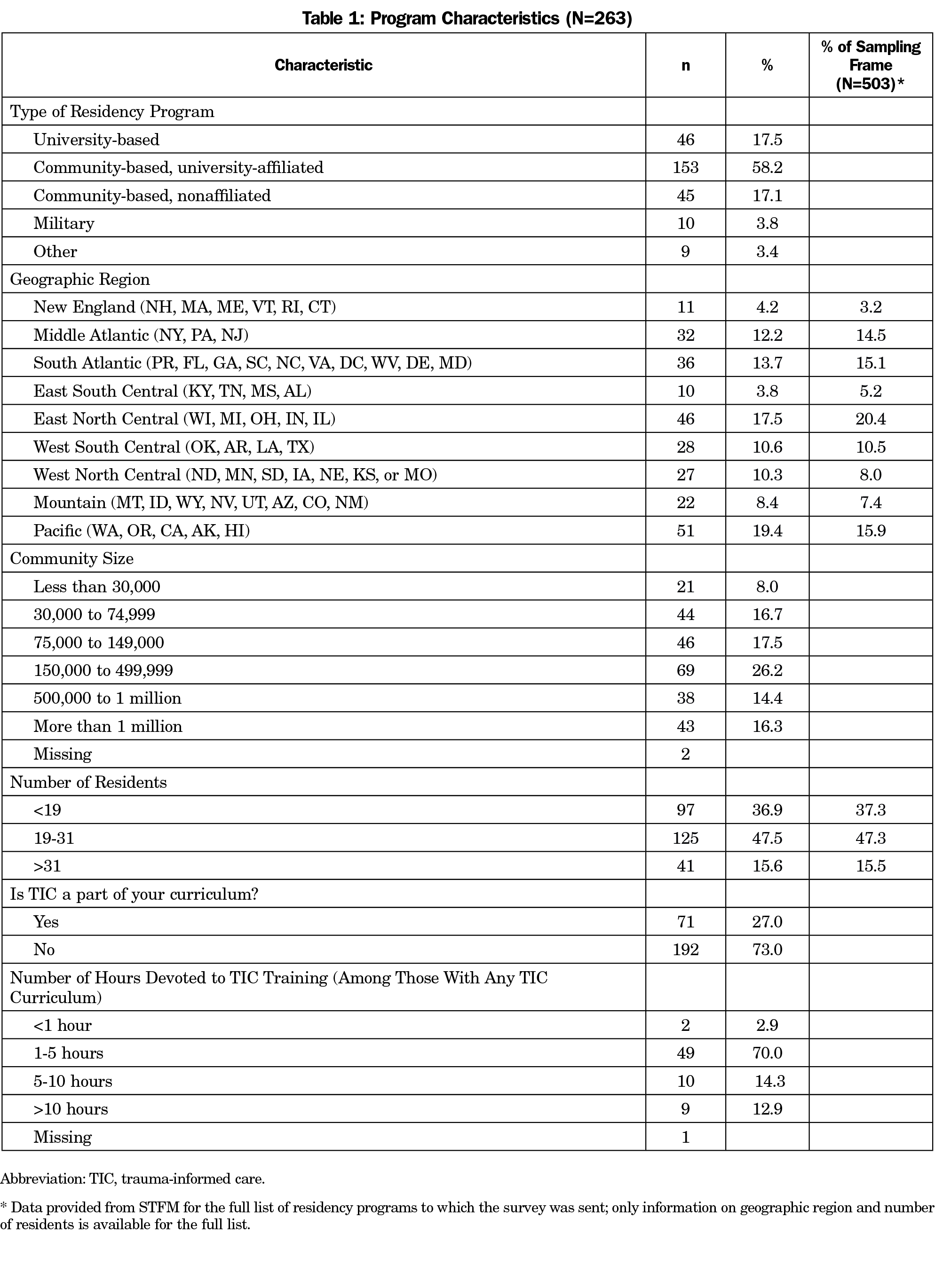


There are no comments for this article.