Background and Objectives: Research into rates of burnout and job satisfaction among family medicine residency coordinators is nonexistent. Coordinators play a pivotal role in medical education, sometimes have multiple roles and titles, and often work in stressful environments. The goals of this study were to explore the prevalence of, and relationship between, burnout and job satisfaction among family medicine residency coordinators.
Methods: This national wellness study involved 307 family medicine residency coordinators. Modified questions of the Professional Quality of Life Scale, Version 5 were used to measure participants’ burnout and job satisfaction rates. The authors used chi-square tests, Pearson’s r correlations, and multiple linear regression to analyze the data.
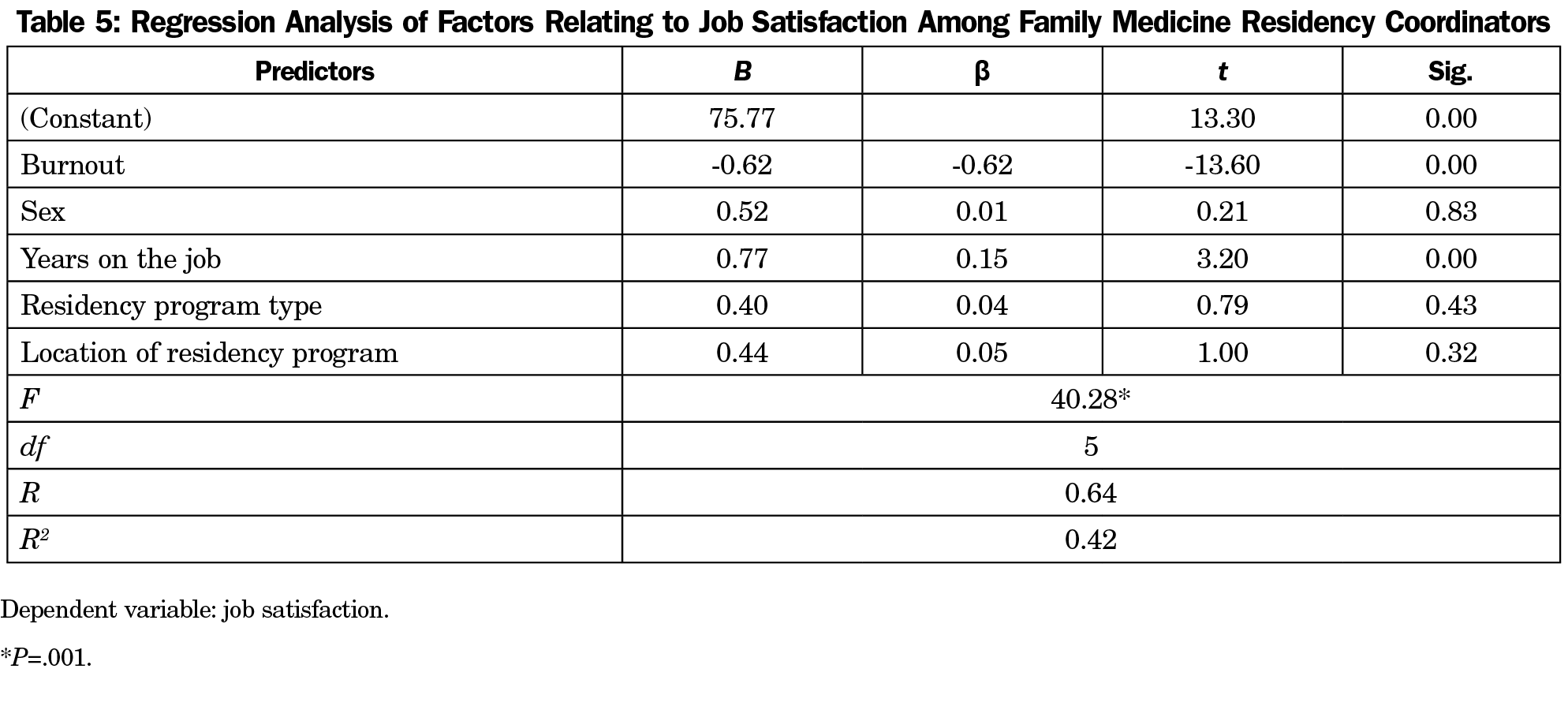
Results: The response rate was 72% (307/429), with 24% of family medicine residency coordinators reporting high, 51% reporting moderate, and 26% reporting low rates of work-related burnout. Twenty-eight percent of the family medicine residency coordinators reported high, 46% moderate, and 26% low job satisfaction. There was a significantly negative relationship between job satisfaction and work-related burnout, r (306)=-.638, P<0.001. Regression explained 42% of variance in job satisfaction, and showed that burnout (β=-.62) and years on the job (β=.15) were significant predictors of job satisfaction (R=0.64; F [5, 277]=40.28, P<.001).
Conclusions: The results demonstrate that family medicine residency coordinators are generally satisfied with their work and reported moderate to high degree of burnout rates.
Residency coordinators play a pivotal role in graduate medical education. They are often the first people residents contact for information. Residency coordinators’ duties include supporting and meeting regularly with program directors and faculty, maintaining databases that contain resident and faculty data, and providing administrative support to residents and fellows. In addition to their administrative duties and responsibilities, evidence suggests that family medicine residency (FMR) coordinators spend an average of 6 hours each week providing emotional and social support to residents.1 Thus, FMR coordinators have multiple roles and often work in an environment that can be stressful.2,3 There are variations in the job title of FMR coordinators including program manager, residency manager, and academic coordinator. For consistency purposes, “FMR coordinators” is used here to refer to all the coordinators irrespective of their job title.
The residency program coordinators’ administrative responsibilities have changed over the years in response to resident work hour restrictions and the Accreditation Council for Graduate Medical Education’s (ACGME) Next Accreditation System (NAS) that emphasizes more outcomes-based resident evaluation, among other aims. This shift in policy has led to the redefinition of the professional responsibilities and requirements of coordinators as essential members of the management team.4
While residency program directors are responsible for the educational portion of the training programs, the NAS has increased the administrative responsibilities of coordinators.5 Increased job responsibilities and duties are associated with increased job stress when there is an inadequate level of institutional support.6,7 In a 2016 study of directors and coordinators of general surgery residency programs, Fountain and colleagues documented an association between additional
ACGME accreditation requirements and burnout among coordinators.6 A review of the literature indicates little information regarding coordinators’ expanded roles and responsibilities with the new ACGME requirements. Given the expanded roles and responsibilities, we wish to study FMR coordinators’ job satisfaction and work-related burnout. Job satisfaction is the pleasure people derive from their work, including their ability to positively affect the lives of people through work.8 Burnout can reflect the feeling people have that their efforts do not make any difference. It can also be associated with a “very high workload or a non-supportive work environment.”9
A 2013 survey by the University of Utah Graduate Medical Education office found that of 56 coordinators from 21 specialties, including an FMR program, 72% reported they were overwhelmed with job duties and 39% considered resigning from their positions.10 Long-term exposure to work-related stress11,12 and low job satisfaction13,14 have been found to be associated with burnout. Given the negative effects of burnout, the
ACGME has intensified efforts in promoting wellness among physicians in the clinical learning environment.15 These efforts have not been formally extended to residency coordinators despite their contribution to medical education. To our knowledge, there are no job satisfaction and burnout studies involving FMR coordinators. Therefore, this study sought to:
- Explore the prevalence of job satisfaction and burnout among FMR coordinators;
- Assess the relationship between job satisfaction and burnout among the FMR coordinators (we hypothesized that the coordinators who report high job satisfaction will report low burnout symptoms), and
- Determine predictors of FMR coordinators’ job satisfaction using the overall burnout score and demographic variables.
Study Design and Participants
This nonexperimental, cross-sectional, national wellness study included data on 307 FMR coordinators who were members of the Association of Family Medicine Administration (AFMA). Study participants completed an anonymous, 39-item online survey that included some modified questions from the Professional Quality of Life Scale (ProQOL) Version 58 and questions used to construct a demographic profile of the participants. The ProQOL is used to measure the negative and positive affects of people in helping positions. FMR coordinators fall within this category given that they provide a significant amount of emotional support to residents1,2 in addition to their administrative duties. The ProQOL research questions used in this study were formatted to better fit the study population, and were modified to suit the purposes of the study. The University of Kansas School of Medicine-Wichita Institutional Review Board granted exemption for the study. A sample size of 300 was calculated as necessary for adequate power (>.85) to detect significant correlations of 0.5, P<.05 between variables.16
Study Instruments
Job Satisfaction: The modified compassion satisfaction scale of the ProQOL was used to measure the satisfaction participants get from doing their work well (job satisfaction). The modified compassion satisfaction scale is a 10-item scale that is scored on a 5-point Likert scale ranging from “never” to “very often.” The 10 items were summed up into job satisfaction scores, which were standardized using a mean of 50 and standard deviation of 10.9 Higher scores on the scales indicate greater job satisfaction. Consistent with convention,8,9 a score of <44 is defined as low satisfaction, 44-56 is average satisfaction, and >56 is defined as high satisfaction.
Burnout: The modified burnout scale of the ProQOL was used to investigate the participants’ work-related burnout rates. The scale consists of 10 questions. Participants recorded how often they experienced specified work-related feelings using a 5-point Likert scale ranging from “never” to “every day.” Five of the items were reverse-scored. The 10 items were summed up into burnout scores, which were standardized using a mean of 50 and standard deviation of 10.8,9 Higher degree of burnout is one in which respondents reported higher scores. Consistent with convention,8,9 a score under 44 was defined as low, 44 to 56 as average, and over 56 as high on the burnout scale.
Demographic Measurement: We also used the following questions to measure participants’ demographic characteristics: sex, years on the job, residency type, and community location of the residency program.
Data Collection
There are 566 accredited FMR programs nationally.17 For logistical reasons (such as our inability to know the total number of the FMR coordinators and their contact information), the current study only included FMR coordinators who were active members of AFMA at the time of the study. AFMA is a professional organization dedicated to the professional growth and development of FMR coordinators. The authors used SurveyMonkey to host the survey, and a generated link was sent via email to all 429 registered members of AFMA in all the 50 states in the United States. Two reminders were subsequently sent to those who had not completed the survey. Data were collected between April 2017 and July 2017.
Statistical Analyses
Descriptive analyses provided detailed demographic information about the respondents and their survey responses. Chi-square tests were conducted to determine the relation between job satisfaction, burnout, and gender (male vs female). Correlation coefficients were calculated to determine factors that related to the respondents’ job satisfaction and burnout, and to assess the relationship between job satisfaction and burnout among the coordinators. We also conducted multiple linear regression analysis using the overall burnout score and demographic measures to determine predictors of job satisfaction of the respondents. A statistical critical value of .05 was specified for all inferential statistics.
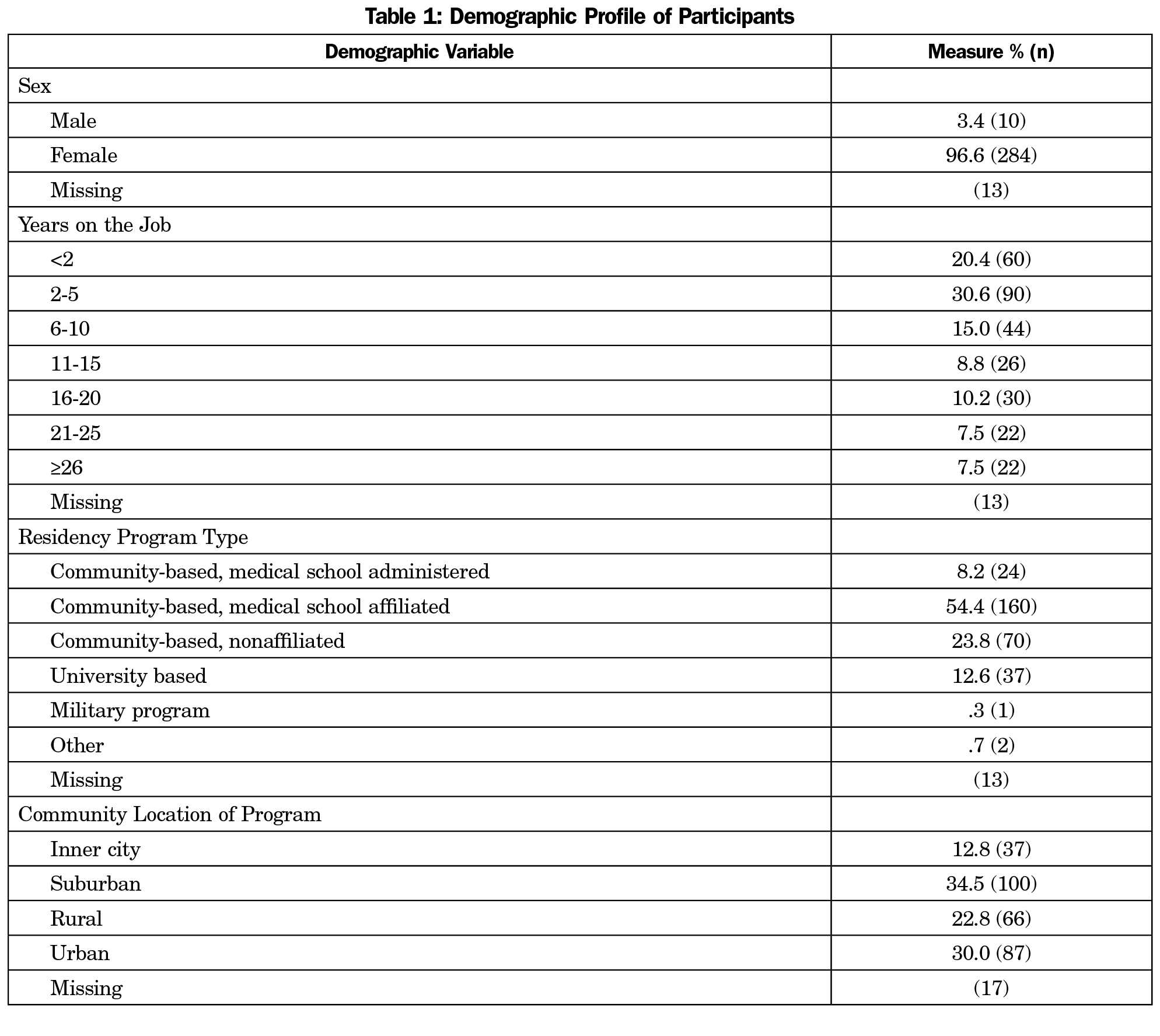
Of the 429 FMR coordinators surveyed, data were collected from 307, for a response rate of 72%. As shown in Table 1, 97% of the participants were female and 51% reported being in their current job for 5 years or less. Fifty-four percent were working in community-based, medical school affiliated programs. The chi-square tests showed no significant relationship between participants’ gender, job satisfaction, and burnout.
Job Satisfaction Results
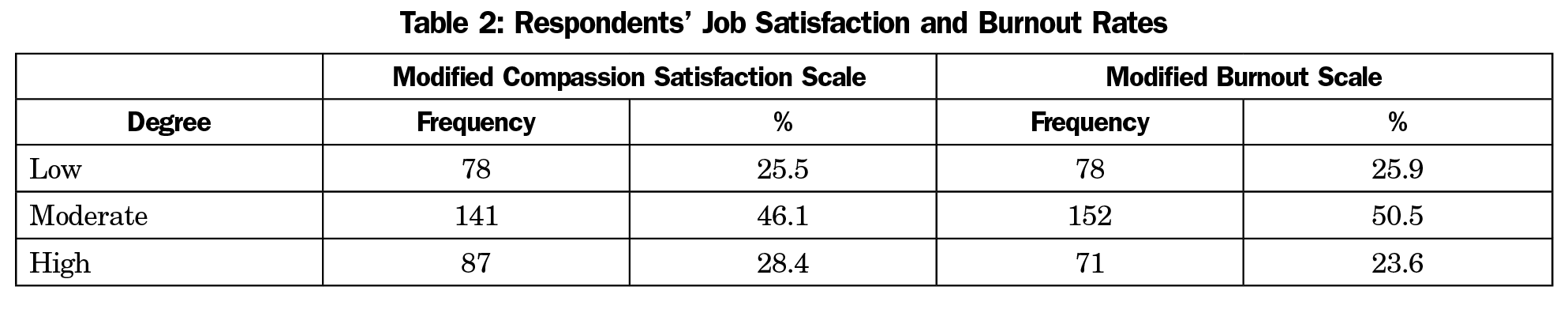
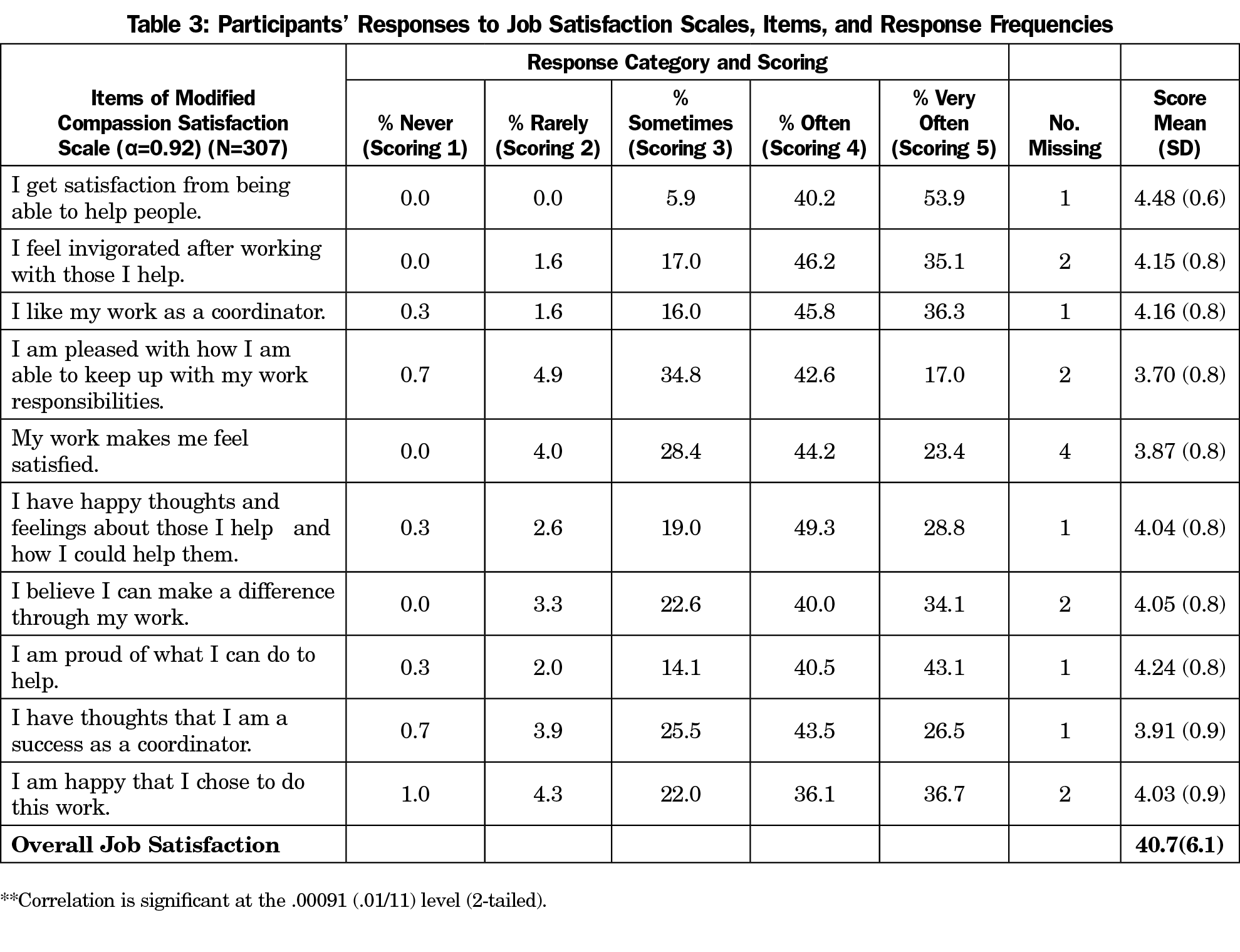
Overall, 28% of the FMR coordinators reported high, 46% average, and 26% low job satisfaction on the modified compassion satisfaction scale (Table 2). Specifically, 94% of the coordinators reported that they often/very often get satisfaction from helping people; 82% often/very often feel invigorated after helping others; and 81% are often/very often like their work as coordinators (Table 3).
Burnout Results
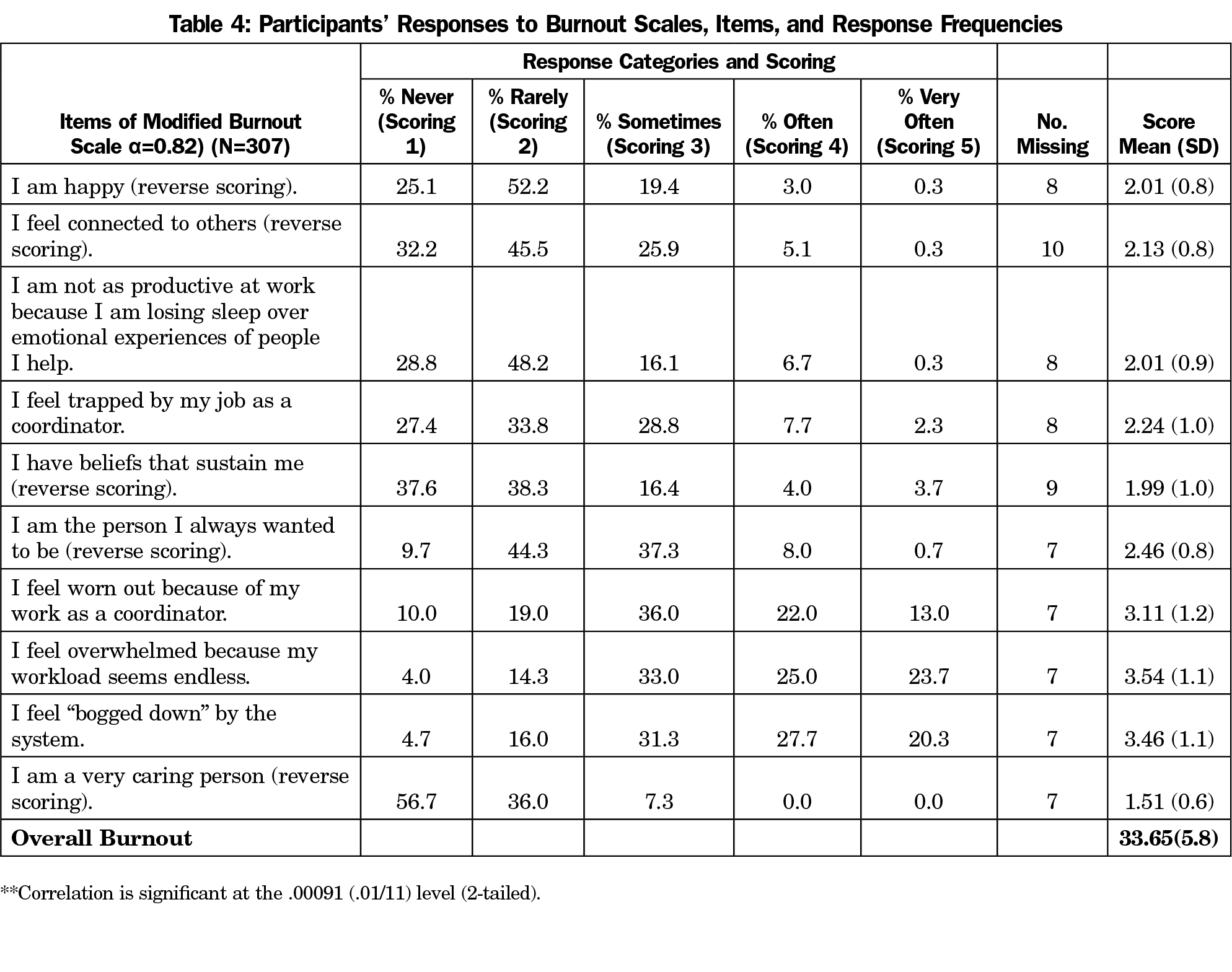
Results of the burnout analyses are presented in Tables 2 and 4. Overall, 24% of FMR coordinators reported high, 51% average, and 26% low rates of work-related burnout on the modified burnout scale (Table 2). As shown in Table 4, 71% of the coordinators reported that their work sometimes/often/very often wore them out, 81% stated that they sometimes/often/very often feel overwhelmed by workload, and 79% indicated that they sometimes/often/very often feel “bogged down” by their work.
Job Satisfaction and Burnout Results
To test the study hypothesis that FMR coordinators who are satisfied with their job will report lower rates of burnout, a correlation coefficient was calculated. The results showed a significantly negative relationship between the variables, r(300)=-.638, P<0.01, suggesting that FMR coordinators who reported satisfaction with their job reported lower rates of burnout on the burnout scale. In predicting the level of FMR coordinators’ job satisfaction, 42% of variance in job satisfaction, and showed that the overall burnout (β=-.62) and years on the job (β=.15) were significant predictors of job satisfaction (R=0.64; F[5, 277] 40.28, P<.001; Table 5).
This study provides detailed information regarding rates of burnout and job satisfaction among FMR coordinators. FMR coordinators had an adequate response rate of 72%. The high response rate may indicate interest in this important subject. Most of the respondents (97%) were female. This high percentage of female respondents is consistent with results of a previous study where 95% of FMR coordinators who participated were female.1 The majority of respondents reported moderate to high job satisfaction, suggesting that FMR coordinators take pride in their work as being able to help people, and derive a great deal of professional satisfaction from their work as coordinators.6
Most of the FMR coordinators’ work is done behind-the-scenes; they provide significant logistical, social, and emotional support to residents, fellows, faculty, and staff.1,2 Although their work is often underrecognized, our study suggests that most FMR coordinators are proud of the work they do as helpers contributing to graduate medical education. Consistent with previous findings,18,19,20 our data show that FMR coordinators who are satisfied with their job report low rates of burnout.
There was a significant negative correlation between the overall job satisfaction and burnout scores. The overall burnout score was a better predictor of job satisfaction with negative β coefficient. These findings suggest that increased rates of burnout are responsible for job dissatisfaction among the FMR coordinators. The FMR coordinators’ years on the job was also a predictor of job satisfaction with positive β coefficients. This finding suggests that FMR coordinators who enjoy their work tend to stay on the job for long time, which is consistent with other studies that have shown inverse relation between job satisfaction and turnover rates.21,22
Seventy-four percent of FMR coordinators have moderate to high burnout rates and deserve attention directed toward their well-being. FMR coordinators should be included in the ACGME’s ongoing promotion of awareness of resident-physician well-being in order to increase work satisfaction and decrease burnout rates. Potential solutions include providing reinforcement for a job well done and ensuring workload is manageable. This study’s data show that although most of the coordinators enjoy their work as helpers contributing to graduate medical education, their workload overwhelms and wears them out.
This study has limitations. First, only members of the AFMA were included. The social support provided by coworkers and supervisors, and its effect on job satisfaction and burnout may vary by location. Another limitation may be the time of year the survey was conducted. The study was conducted between April 2017 and July 2017, at a time of heavy workload, which included residency graduation and preparing for first-year residents to start. Additionally, the survey only provides a single snapshot of the FMR coordinators’ subjective responses.
The data collected has the potential for many future projects. One possibility is to collect longitudinal data similar to the work done on physician burnout and satisfaction at Mayo Clinic in 2011 and 2014. The relationship of this data to coordinators’ turnover rates could also be assessed given that 51% of the FMR coordinators have been on the job for less than 5 years. Future attention could be directed toward assessing associations between FMR coordinators’ satisfaction and burnout and residency faculty job satisfaction and burnout.
In conclusion, the findings of this national study have drawn attention to the importance of family medicine residency coordinators’ well-being. Job satisfaction and burnout constructs are well studied among clinicians, and are now documented among family medicine residency coordinators.
Acknowledgments
Conflict Disclosure: Cheryl Haynes is the current president of the Association of Medicine Administration. Lisa Marquise is currently the media chair of the Association of Family Medicine Administration. Caren Bachman is the residency education symposium committee chair of the Association of Family Medicine Administration.
References
- McCann WJ, Knudson M, Andrews M, Locke M, Davis SW. Hidden in plain sight: residency coordinators’ social support of residents in family medicine residency programs. Fam Med. 2011;43(8):551-555.
- Scot K, Garvin K. Coordinators’ stress: results of a national survey. www.apds.org/ARCS%202006%20Talks/APDSCoordinators%20Stress.ppt. Accessed August 17, 2017.
- Ike SFM, Rotandi CL, Christofferson M, Johnson E, Carpenter P, Bruse JD, Pike K. Program coordinator wellness: combating burnout and promoting career satisfaction. Presented at: Association of Pediatric Program Directors Annual Meeting; March 30-April 2, 2016; New Orleans, LA. https://www.appd.org/meetings/2016SpringPresentations/WS9CFridaySlides.pdf. Accessed August 17, 2017.
- Grant RE, Murphy LA, Murphy JE. Expansion of the coordinator role in orthopaedic residency program management. Clin Orthop Relat Res. 2008;466(3):737-742. https://doi.org/10.1007/s11999-007-0110-6
- Training Administrators of Graduate Medical Education. The History of TAGME. http://tagme.org/history/. Accessed December 20, 2017.
- Fountain D, Quach C, Norton D, White S, Ratliff S, Molteg K, Heyduk D, Roof J, Badurina L. The perfect storm is on the horizon! J Surg Educ. 2017;74(6):e120-e123. https://doi.org/10.1016/j.jsurg.2017.07.020
- Raitano RE, Kleiner BH. Stress management: Stressors, diagnosis, and preventative measures. Manage Res News. 2004;27(4/5):32-38. https://doi.org/10.1108/01409170410784446
- Stamm BH. Professional quality of life: compassion satisfaction and fatigue version 5 (ProQOL, 2009-2012). https://www.templateroller.com/template/2521452/compassion-satisfaction-and-compassion-fatigue-proqol-version-5.html. Accessed August 17, 2017.
- Stamm H. The ProQOL Manual. Brooklandville, MD: Sidran Press; 2005. http://www.compassionfatigue.org/pages/ProQOLManualOct05.pdf. Accessed December 20, 2017.
- Bracken S, Garcia A, Asay K, Bird E, Butterfield R, et al. Program coordinator burnout: building support and job satisfaction through GME [poster]. https://medicine.utah.edu/gme/coordinators/files/acgme-poster.pdf. Accessed August 17, 2017.
- Maslach C, Schaufeli WB. Historical and conceptual development of burnout. In Schaufeli WB, Maslach C, Marek T, eds. Series in Applied Psychology: Social Issues and Questions. Philadelphia, PA: Taylor & Francis; 1993:1-16.
- Collings JA, Murray PJ. Predictors of stress amongst social workers: an empirical study. Br J Soc Work. 1996;26(3):375-387. https://doi.org/10.1093/oxfordjournals.bjsw.a011101
- Burisch M. A longitudinal study of burnout: the relative importance of dispositions and experiences. Work Stress. 2002;16(1):1-17. https://doi.org/10.1080/02678370110112506
- Kalliath T, Morris R. Job satisfaction among nurses: a predictor of burnout levels. J Nurs Adm. 2002;32(12):648-654. https://doi.org/10.1097/00005110-200212000-00010
- Nasca T. Physician Wellbeing: Letter to the Community. http://www.acgme.org/Portals/0/PDFs/Nasca-Community/August2016NascaLettertoCommunity.pdf. Accessed October 17, 2017.
- Australia and New Zealand Melanoma Trials Group Statistical Decision Tree. Power Calculation for Pearson’s & Spearman’s Correlation. https://www.anzmtg.org/stats/PowerCalculator/PowerCorrelation. Accessed August 17, 2017.
- Accreditation Council for Graduate Medical Education. Number of Accredited Programs Academic Year 2017-2018 United States. https://apps.acgme.org/ads/Public/Reports/ReportRun?ReportId=3&CurrentYear=2017&AcademicYearId=2017. Accessed December 24, 2017.
- Ofei-Dodoo S, Scripter C, Kellerman R. Job satisfaction and burnout among nonclinical workers in a medical education center. Fam Med. 2018;50(3):223-227. https://doi.org/10.22454/FamMed.2018.473306
- Ogresta J, Rusac S, Zorec L. Relation between burnout syndrome and job satisfaction among mental health workers. Croat Med J. 2008;49(3):364-374. https://doi.org/10.3325/cmj.2008.3.364
- Khamisa N, Peltzer K, Ilic D, Oldenburg B. Work related stress, burnout, job satisfaction and general health of nurses: A follow-up study. Int J Nurs Pract. 2016;22(6):538-545. https://doi.org/10.1111/ijn.12455
- Medina E. Job satisfaction and employee turnover intention: what does organizational culture have to do with it? [master’s thesis] New York: Columbia University Academic Commons; 2012. https://doi.org/10.7916/D8DV1S08
- Sherman MF, Gershon RR, Samar SM, Pearson JM, Canton AN, Damsky MR. Safety factors predictive of job satisfaction and job retention among home healthcare aides. J Occup Environ Med. 2008;50(12):1430-1441. https://doi.org/10.1097/JOM.0b013e31818a388e



There are no comments for this article.