Background and Objectives: Point-of-care ultrasound (POCUS) is increasingly being incorporated into family medicine residency training. Attitudes towards POCUS among family medicine residents (FMRs) are largely unknown, and confidence levels with performing and interpreting POCUS exams are also unknown among this group of learners. Our aim was to evaluate FMRs’ attitudes and confidence levels before and after the implementation of a new POCUS curriculum.
Methods: Study participants included FMRs in all postgraduate years (ie, PGY1-PGY3) at the University of New Mexico (UNM) Family Medicine Residency Program. Our intervention was a yearlong implementation of a new POCUS curriculum based on the American Academy of Family Physicians POCUS curriculum guidelines. Our interventions included hands-on training sessions for both FMRs and faculty along with a resource website. We assessed attitudes and confidence levels with various POCUS exams using a pre- and postintervention survey.
Results: Overall, FMRs felt significantly more confident in their ability to perform and interpret a point-of-care ultrasound after the implementation of POCUS curriculum. There was no significant difference in participants’ expectations of their use of POCUS during or after residency.
Conclusions: Overall, this study provides evidence that the implementation of a POCUS curriculum that includes hands-on and didactic training is associated with increased confidence in utilizing POCUS among FMRs.
For years, point-of-care ultrasound (POCUS) has been utilized by various medical specialties, and the value of POCUS in clinical decision-making has been extensively demonstrated.1-4 However, POCUS has only recently been introduced in family medicine residencies, and many residencies lack a family medicine-focused POCUS training curriculum.5,6 The American Academy of Family Physicians published its first guideline on POCUS curriculum in 2018.7 This guideline is unique compared to other disciplines’ ultrasound curricula in that it incorporates a large variety of POCUS skills, acknowledging the broad training of a family medicine resident (FMR). There have been studies to investigate program directors’ perceptions of resident attitudes, use, and barriers to use of POCUS, but attitudes and confidence levels regarding POCUS among FMRs are largely unknown.8,9 Because POCUS operator dependency is high compared with other diagnostic testing, skill development along with confidence in obtaining and interpreting images is vital.10 Our aim was to evaluate FMRs’ attitudes and confidence levels before and after implementation of a novel POCUS curriculum. Our hypothesis was that the confidence level in both performing and interpreting POCUS applications would increase.
Research of attitudes and confidence surrounding POCUS is limited, particularly regarding FMRs. However, there are some studies of residents in internal medicine, general surgery, and emergency medicine that have measured attitudes and confidence.11-14 These studies found that brief POCUS sessions or simulation-based ultrasound learning modules did improve the overall learner confidence levels.
Study participants included FMRs in the University of New Mexico (UNM) Family Medicine Residency program in all postgraduate years (ie, PGY1-PGY3). Our 1-year intervention included:
- 3-hour, hands-on POCUS workshop for FMRs focused on fundamentals of ultrasound and POCUS exams;
- 18-hour, hands-on POCUS workshop focused on fundamentals (over 2 consecutive days) for faculty members (four FMRs were present for this workshop as volunteer models);
- Web-based POCUS resource available to FMRs; and
- 30-minute, exam-based POCUS sessions every other week for FMRs on the family medicine inpatient service.
We assessed attitudes and confidence levels using the same SurveyMonkey survey in September 2017 prior to our 1-year intervention and again in September 2018 after the intervention. No identifiers were requested on the surveys besides postgraduate year. Survey questions used Likert scaling and were focused on the core applications of POCUS included in the American Academy of Family Physicians POCUS curriculum guideline.7
We summarized survey responses as frequencies and percentages or as means and standard deviations. Variables had ordinal scaling and sample sizes were less than 30 per group, so we used nonparametric Wilcoxon rank sum tests to assess equality of pre- and postresponses (Stata v.15 software). We set significance at <.05 for P values from testing.
UNM Health Sciences Center Human Research Protections Office Institutional Review Board granted this study an exemption from formal review.
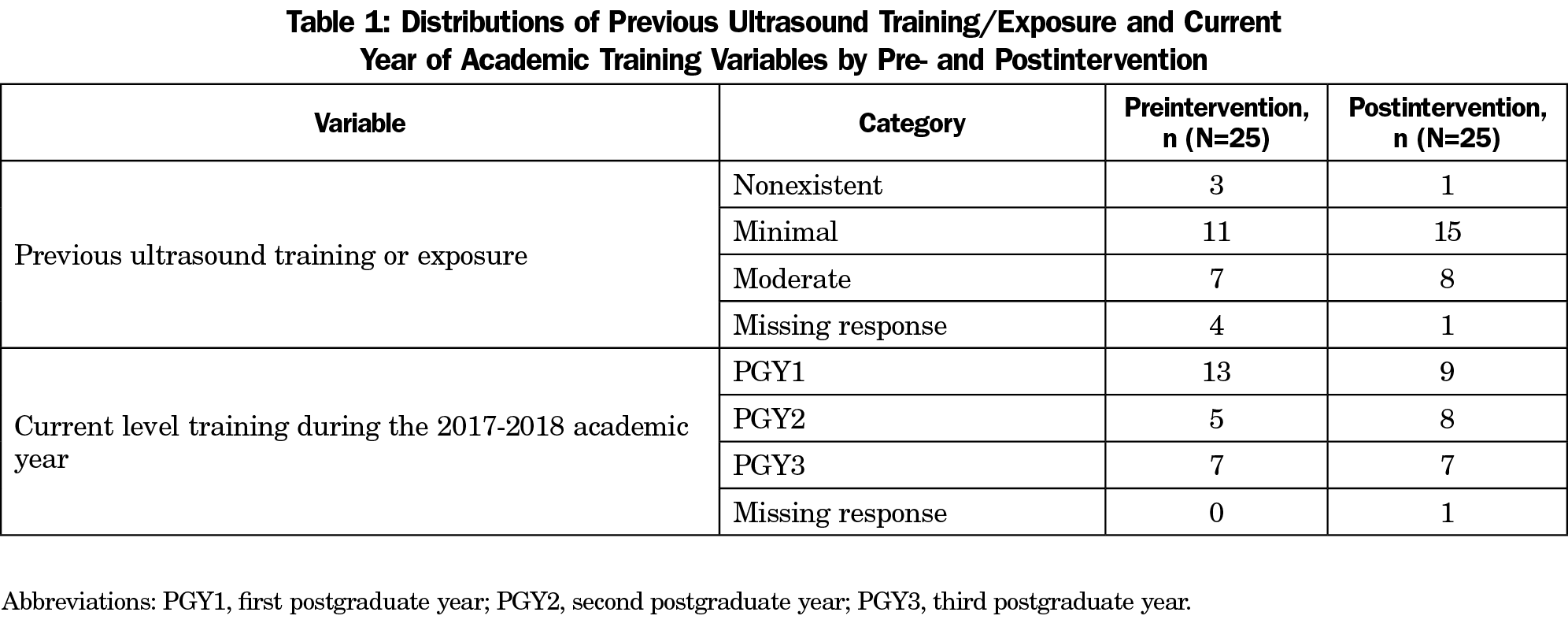
Survey response rates were 25/45 (56%) in the preintervention, and 25/46 (54%) in the postintervention. Table 1 shows no significant differences in level of training (PGY1, PGY2, or PGY3; P=.48) or in previous ultrasound training or exposure between pre- and postintervention (P=.66).
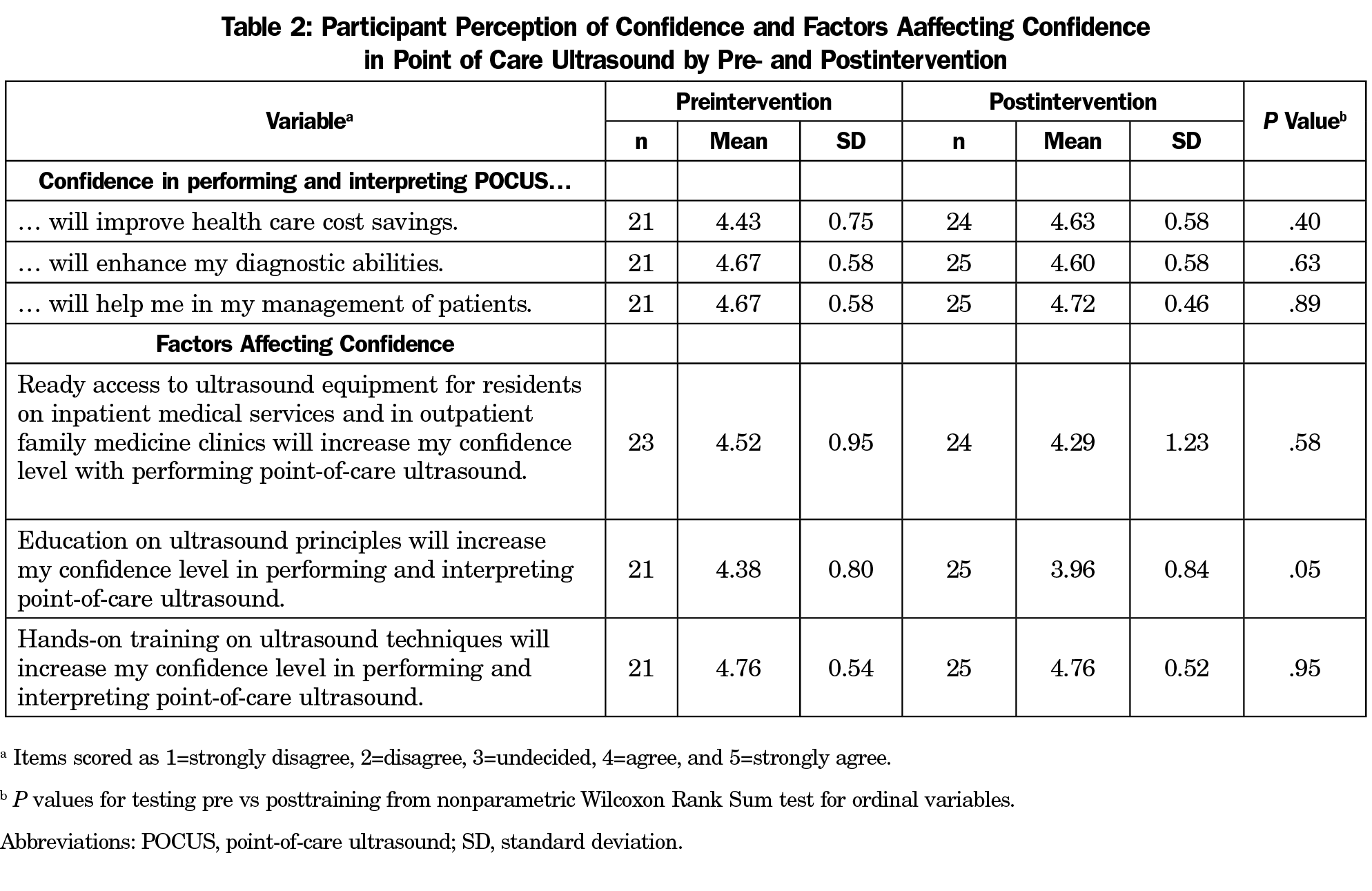
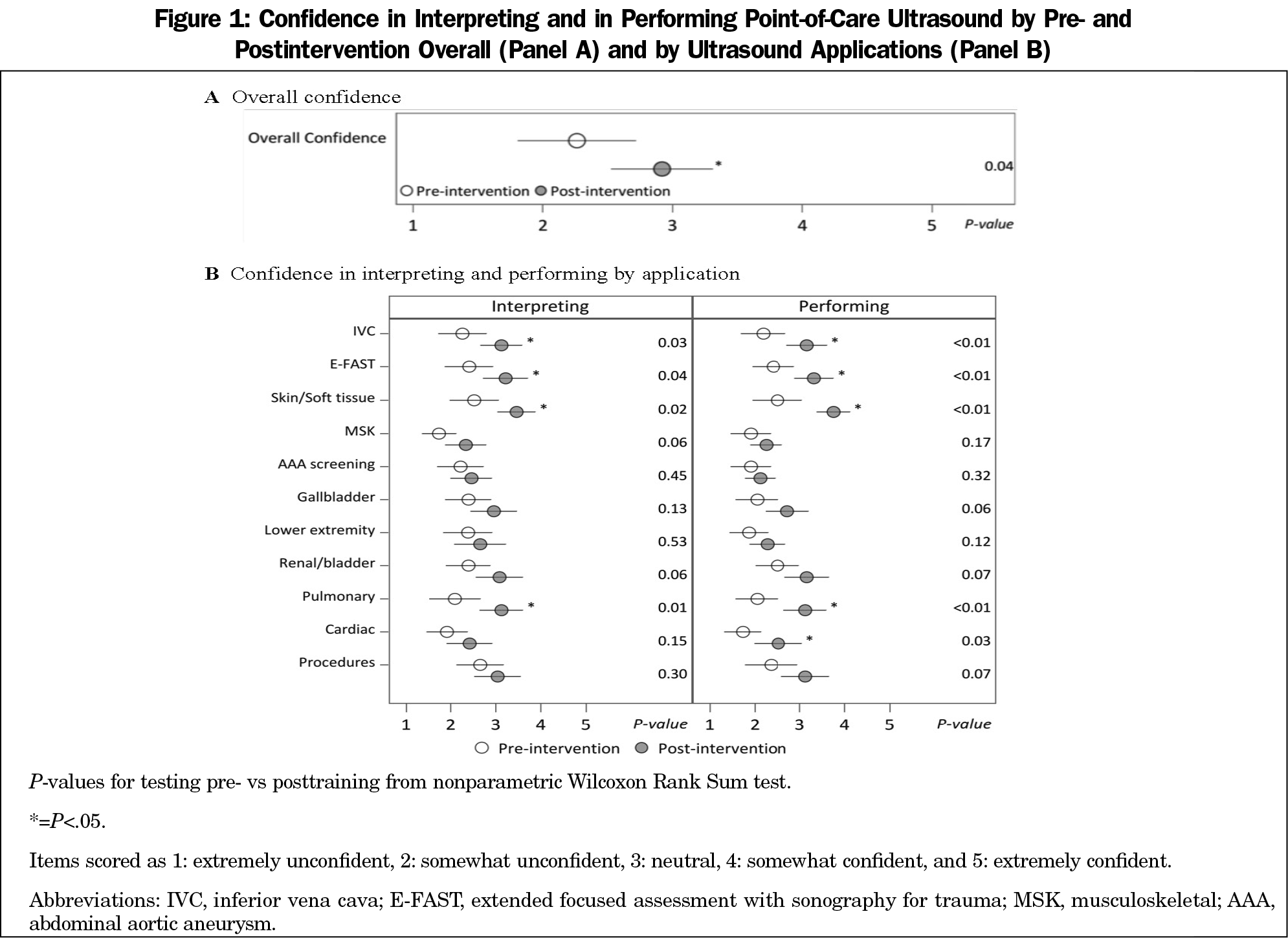
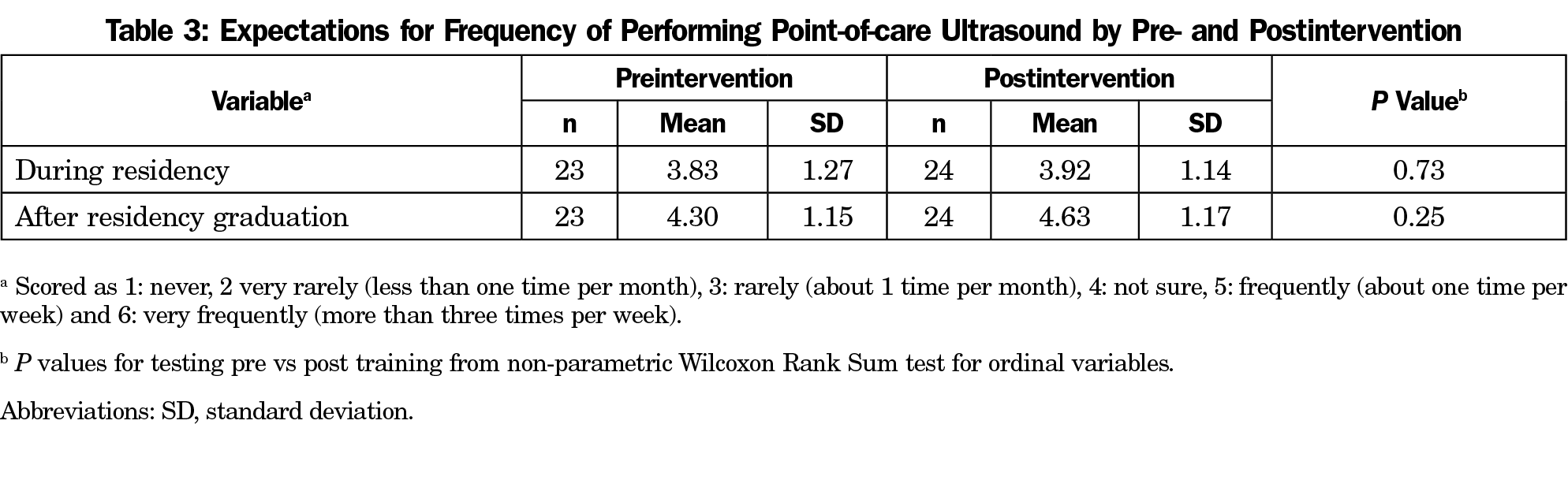
Table 2 shows that the pre- and postintervention attitudes toward POCUS were overall not significantly different. Figure 1 demonstrates pre- and postintervention differences in participants’ confidence levels specific to ultrasound applications. Overall, FMRs felt significantly more confident in performing and interpreting a POCUS exam to answer a clinical question postintervention. Confidence improved significantly in performing and in interpreting four POCUS applications: inferior vena cava (IVC), extended focused assessment with sonography for trauma (E-FAST), skin/soft tissue, and pulmonary exams. Confidence improved significantly in performing cardiac evaluations. All other activities showed minor gains in confidence in both performing and interpreting. There were no significant pre- and postintervention differences in FMRs’ expectations in their use of POCUS during or after residency (Table 3).
Confidence levels of FMRs in performing and interpreting POCUS applications improved after the implementation of a POCUS curriculum. These findings are important as they demonstrate that increased training of faculty and FMRs on POCUS applications appears to improve self-reported learner confidence in answering clinical point-of-care questions.
There were several methodologic limitations to our study. Traditional paired analyses were not possible as the data were anonymous and we could not track FMRs after graduation. In addition, there were four FMRs who participated passively as volunteer models in the 18-hour workshop provided to our faculty, which may have also provided inequitable POCUS exposure. Some surveys were not completely filled out, which is another limitation in the statistical analysis. There was a low response rate in our study, which may be due to nature of busy residency training and lack of time to complete the surveys.
Interestingly, the baseline attitudes toward POCUS were very favorable in both the pre- and postintervention surveys. This may reflect a strong interest among FMRs in POCUS applications, but additional POCUS training did not alter these attitudes.
Our study also found that FMRs felt that they would use POCUS at least one time per month both during residency and after residency graduation, which is a promising result. However, FMRs may perceive other barriers to using POCUS in clinical practice besides lack of confidence that were not addressed in this study.
This study provides evidence that simple interventions are associated with increased FMR confidence in utilizing POCUS. We cannot clearly correlate confidence with clinical competency in POCUS or infer that confidence will lead to future use of POCUS applications in practice without further research in the field.15 However, we can expect that continued confidence building and knowledge acquisition will push learners along the Dunning-Kruger curve towards becoming masters.16 Future research opportunities include investigating the effectiveness of different POCUS training modalities among FMRs and associated effects on patient-oriented outcomes. However, medical schools, hospitals, and health systems will have to invest in POCUS resources and training before large effectiveness trials can evaluate clinical outcomes. Further training on POCUS applications at all levels of medical education will help further research on this topic.
Acknowledgments
The authors acknowledge the University of New Mexico Department of Family and Community Medicine, Contra Costa Family Medicine Resident Program (who provided Train-the-Trainer Point of Care Ultrasound course on September 9-10, 2017), and the FCM Research Management Team (Jeff Carter, Ashton Lawler, and Maxwell Randall).
References
- Moore CL, Copel JA. Point-of-care ultrasonography. N Engl J Med. 2011;364(8):749-757. doi:10.1056/NEJMra0909487
- Melniker LA, Leibner E, McKenney MG, Lopez P, Briggs WM, Mancuso CA. Randomized controlled clinical trial of point-of-care, limited ultrasonography for trauma in the emergency department: the first sonography outcomes assessment program trial. Ann Emerg Med. 2006;48(3):227-235. doi:10.1016/j.annemergmed.2006.01.008
- Mantuani D, Frazee BW, Fahimi J, Nagdev A. Point-of-care multi-organ ultrasound improves diagnostic accuracy in adults presenting to the emergency department with acute dyspnea. West J Emerg Med. 2016;17(1):46-53. doi:10.5811/westjem.2015.11.28525
- Kendall JL, Hoffenberg SR, Smith RS. History of emergency and critical care ultrasound: the evolution of a new imaging paradigm. Crit Care Med. 2007;35(5)(suppl):S126-S130. doi:10.1097/01.CCM.0000260623.38982.83
- Bornemann P. Assessment of a novel point-of-care ultrasound curriculum’s effect on competency measures in family medicine graduate medical education. J Ultrasound Med. 2017;36(6):1205-1211. doi:10.7863/ultra.16.05002
- Flick D. Bedside ultrasound education in primary care. J Ultrasound Med. 2016;35(7):1369-1371. doi:10.7863/ultra.15.08073
- American Academy of Family Physicians. AAFP Recommended Curriculum Guidelines for Family Medicine Residents Point of Care Ultrasound. Reprint No. 290D. https://www.aafp.org/dam/AAFP/documents/medical_education_residency/program_directors/Reprint290D_POCUS.pdf. Accessed February 18, 2021.
- Hall JW, Holman H, Bornemann P, et al. Point of care ultrasound in family medicine residency programs: a CERA study. Fam Med. 2015;47(9):706-711.
- Hall JWW, Holman H, Barreto TW, et al. Point-of-care ultrasound in family medicine residencies 5-year update: a CERA study. Fam Med. 2020;52(7):505-511. doi:10.22454/FamMed.2020.223648
- Geria RN, Raio CC, Tayal V. Point-of-care ultrasound: not a stethoscope-a separate clinical entity. [letter]. J Ultrasound Med. 2015;34(1):172-173. doi:10.7863/ultra.34.1.172
- Keddis MT, Cullen MW, Reed DA, et al. Effectiveness of an ultrasound training module for internal medicine residents. BMC Med Educ. 2011;11(1):75. doi:10.1186/1472-6920-11-75
- Stolz LA, Amini R, Situ-LaCasse E, et al. Multimodular ultrasound orientation: residents' confidence and skill in performing point-of-care ultrasound. Cureus. 2018;10(11):e3597. doi:10.7759/cureus.3597
- Kotagal M, Quiroga E, Ruffatto BJ, et al. Impact of point-of-care ultrasound training on surgical residents’ confidence. J Surg Educ. 2015;72(4):e82-e87. doi:10.1016/j.jsurg.2015.01.021
- Bhagra A, Tierney DM, Sekiguchi H, Soni NJ. Point-of-care ultrasonography for primary care physicians and general internists. Mayo Clin Proc. 2016 Dec;91(12):1811-1827. doi:10.1016/j.mayocp.2016.08.023.
- Morgan PJ, Cleave-Hogg D. Comparison between medical students’ experience, confidence and competence. Med Educ. 2002;36(6):534-539. doi:10.1046/j.1365-2923.2002.01228.x
- Kruger J, Dunning D. Unskilled and unaware of it: how difficulties in recognizing one’s own incompetence lead to inflated self-assessments. J Pers Soc Psychol. 1999;77(6):1121-1134. doi:10.1037/0022-3514.77.6.1121



There are no comments for this article.