Background and Objectives: Primary care physician shortage represents a challenge for many countries and territories, including Puerto Rico (PR), where a significant proportion of the graduating medical students preferred the continental United States (C-US) to complete their training and even as the definitive setting for their practice. We surveyed medical students who graduated from medical schools in PR and have been accepted in a residency program to evaluate the influence of a set of demographics, academic, and personal factors in their decision to pursue a primary care residency program in the C-US.
Methods: A 19-item questionnaire was distributed by institutional email to those medical students who graduated from one of the four Liaison Committee on Medical Education fully accredited medical schools in PR in 2019. We summarized our data by frequency and percentages. We performed data analysis with statistical significance considered for P values <.05.
Results: The questionnaire had a response rate of 51% (138/273), where 49% (67/138) were accepted in a primary care residency. Sixty percent (40/67) matched in a primary care program in the C-US. Among the evaluated factors, a prior degree in C-US (65%) and first-degree relatives living in the C-US (70%) were associated with students who matched in the mainland. First-degree relatives living in PR (96%) were associated with students who remained on the island for training.
Conclusions: The results provide insight into the influence that personal factors have on the decision of medical students in PR to pursue primary care training in the C-US.
Primary care physicians (PCP) serve as the foundation of effective health care practice around the world.1 They are essential for the integrative care of the population through the prevention, diagnosis, management, and treatment of a wide array of conditions.2-4 The Association of American Medical Colleges (AAMC) classified as PCP those doctors involved in general practice, family medicine, internal medicine, pediatrics, and geriatric medicine.5 Several studies have demonstrated that the availability of these physicians in the community improves health costs and outcomes.3,4,6 Unfortunately, there has been a persistent shortage of PCPs in the United States and Puerto Rico (PR) over the years.7-9 In a report from June 2021, the AAMC projected a shortage of between 17,800 and 48,000 PCPs in the United States by 2034.5 These estimates could be associated with the fact that the number of medical students choosing to enter primary care (PC) residency programs have been declining since 1985.10
The consequences of the projected PCP shortage may represent a more significant challenge for the US territories such as Puerto Rico (PR) compared to the mainland. The estimated average of PCPs per 100,000 people in the continent is 156.7, while in PR, this number is reduced to 120.7.11 This discrepancy may be compounded by the fact that the island has been suffering from a massive exodus of physicians due to the economic crisis. From 2006 to 2016, it has been estimated that 5,000 physicians have moved their practices from PR.12 This condition has been aggravated by the low retention rate of PCP in the island, as has been exemplified by the 40.5% of retention of the family medicine graduates reported in 2018.9
Currently, about 300 medical students graduate annually from the four Liaison Committee on Medical Education (LCME) accredited medical schools in PR. A large proportion of these students seek training in the continental US (C-US). However, to date, no studies have analyzed what promotes those medical students from medical schools in PR (MS-PR) to consider PC training in the C-US. We compared a set of demographics, academic, and personal factors of MS-PR to determine their role in the decision to pursue a PC residency in the C-US.
The population for our cross-sectional study were the medical students who graduated from one of the four medical schools in Puerto Rico: University of Puerto Rico (UPR), Escuela San Juan Bautista (ESJB), Universidad Central del Caribe (UCC), and Ponce Health Sciences University (PHSU) and matched in a residency program in 2019. We collected data using a questionnaire sent via the institutional email to those MS-PR who matched a training program within the study period.
Informed consent was requested prior to initiating the questionnaire. The form contained an opening statement that explained the purpose of the study, along with a description of its anonymity and voluntary nature.
The questionnaire included 19 items about basic demographic information (Questions 1-6), professional profile (Questions 7-10; advance degrees, United States Medical License Exam [USMLE] Step 1 and 2 scores, class rank), and personal life aspects (Questions 11-14; prior degree in the C-US, relatives living in PR or C-US, relatives practicing medicine in PR or C-US). Additionally, we assessed the perception of the US-matched MS-PR about the potential benefits of PC training in C-US and about possible improvements to encourage their return to PR to practice (Questions 15-19).
We summarized the data as frequency and percentages. We performed comparisons between the groups were performed using the Fisher exact test and Pearson χ2 test. A P value of <.05 was considered statistically significant.
The Institutional Review Board at the University of Puerto Rico, Medical Sciences Campus approved this study (Protocol #B0110117).
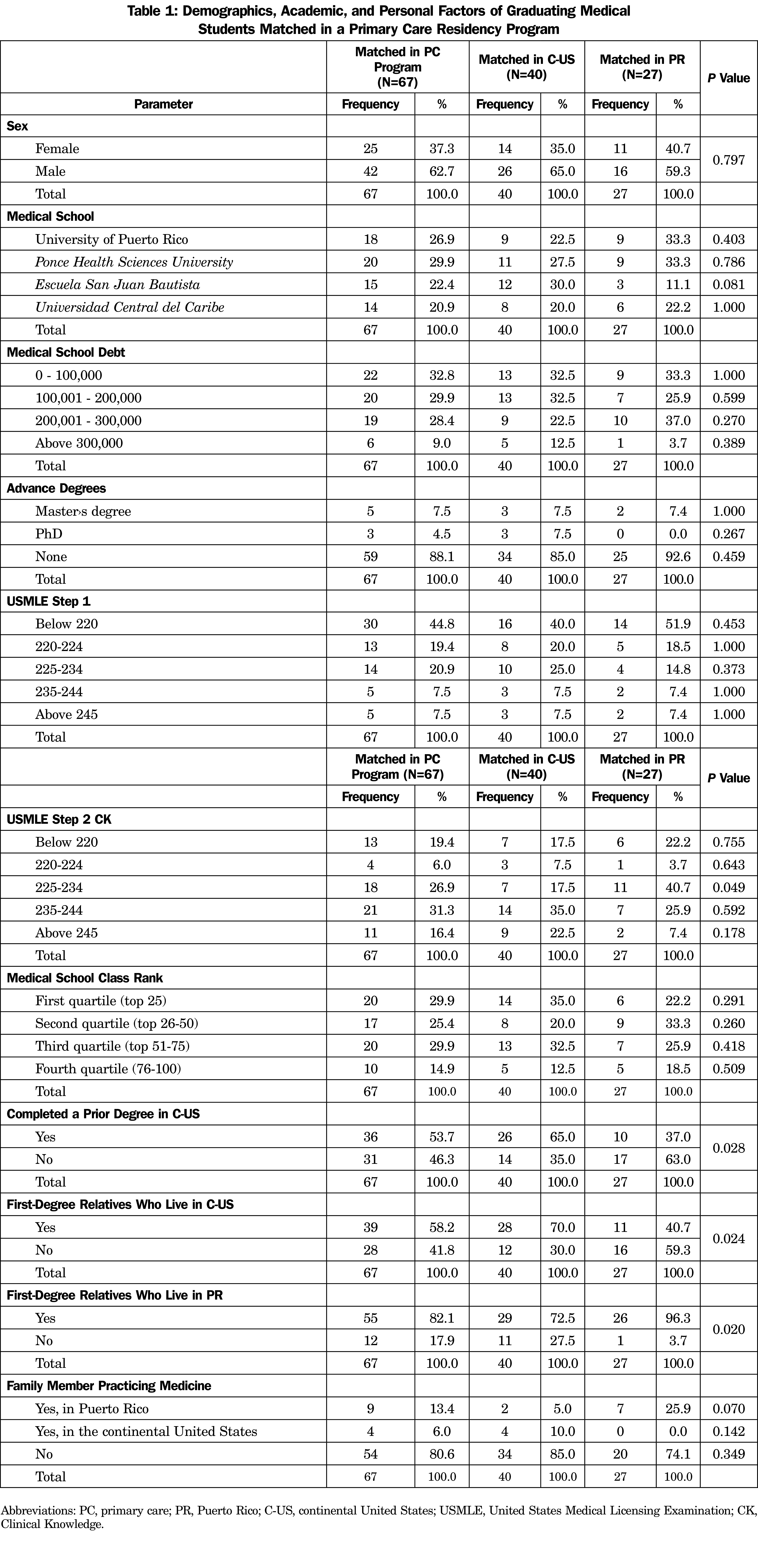
Respondents consist of 138 MS-PR (138/273 MS-PR; response rate: 51%) who graduated in 2019. From this group, 67 students (49%) met the inclusion criteria of being matched to a PC program. The majority (40/67; 60%) corresponded to a training position in the C-US (Table 1).
Personal factors such as a prior degree in the mainland (65%) and first-degree relatives living in the C-US (70%) were associated with MS-PR who matched in a PC program in C-US (P<.03). Conversely, there is an association between those who matched in PR (P<.02) with having first-degree relatives living in PR (96%). There was no statistically significant difference in advanced degrees, the medical school debt, or the academic profile (USMLE scores, class rank, advanced degrees).
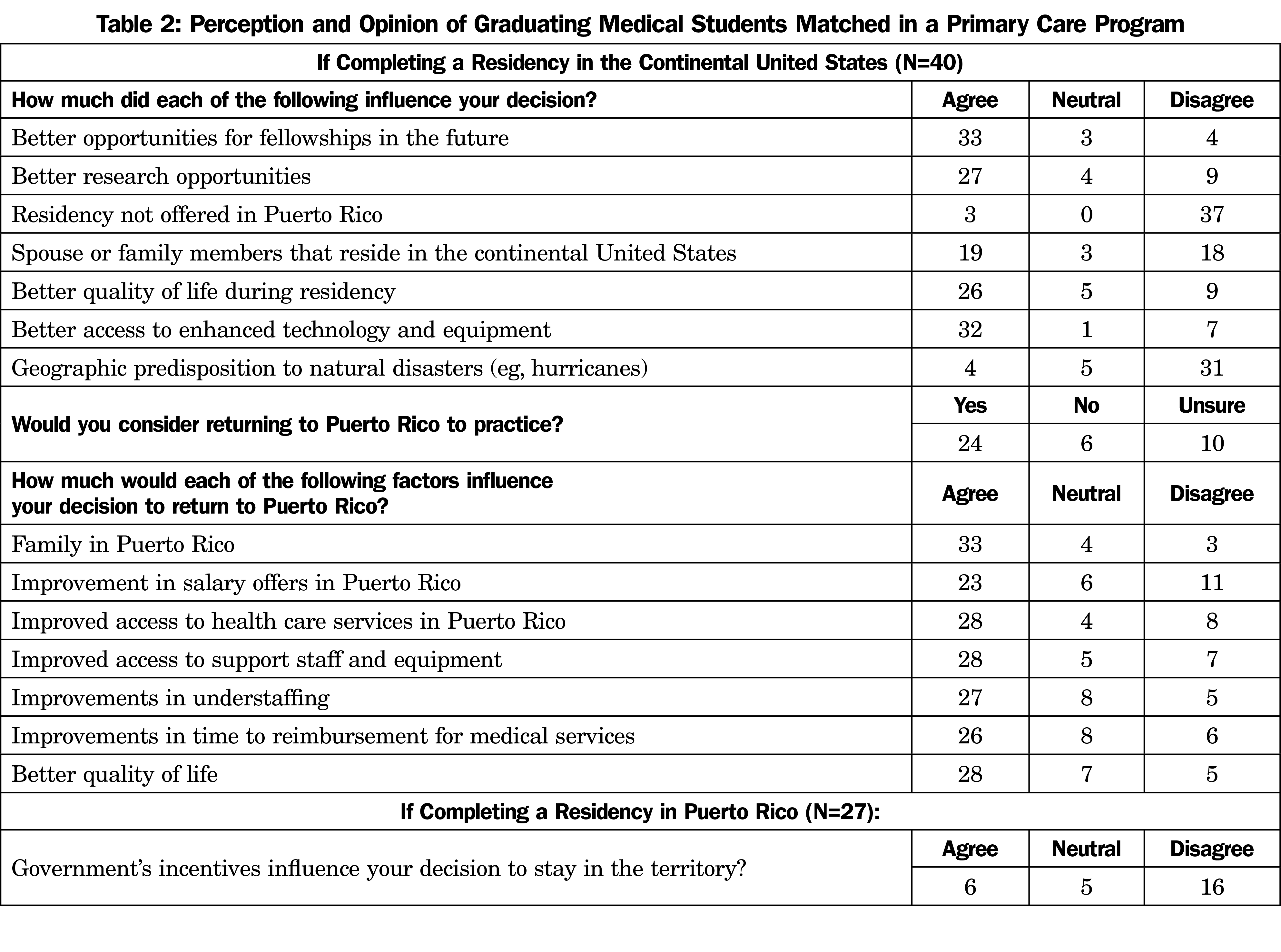
For those who matched in the C-US, fellowship opportunities (83%), training quality (83%), access to enhanced technology and equipment (80%), research opportunities (68%), and quality of life during residency (65%) were among factors they found superior and motivated them to choose a residency in C-US. Geographic predisposition to natural disasters (eg, hurricanes) was not an influential factor within this group (Table 2).
Most MS-PR (60%) leaving to C-US would consider returning to PR for practice. Their decision would be encouraged by improvements in access to health care services (70%), quality of life in terms of work hours (70%), understaffing (68%), time to reimbursement for medical services (65%), and salary offers (58%).
Our findings suggest that personal factors, such as having a prior degree in the mainland and first-degree relatives in the C-US, are most influential in the decision of MS-PR to pursue a PC residency in the C-US. The fact that these significant factors are nonmodifiable represents a challenge for local governments and hospitals when considering strategies to retain future PCPs. These results are consistent with previous studies that show how unchangeable factors, like family, friends, and peers, have a major influence on the decision of students when deciding on residency programs.13-15
A search for better economic opportunities has been reported as the strongest influencing factor leading to the exodus of health professionals from PR to the C-US.10 Interestingly, economic factors like total medical school debt and specific financial incentives provided by the government were not as influential in the decision of our respondents when deciding where to pursue a PC residency. This situation would further limit the governments’ options when working on plans to attract future PC residents. Although attracting a physician workforce involves a complex, multilayered approach, our findings indicate that financial and professional strategies may be less influential than previously thought.16
More importantly, governments and program leaders should consider allocating their funds to projects that address the factors described in this study. For example, prioritizing implementing a reputable research program or improving access to advanced equipment may ultimately enhance residents’ training and, subsequently, their quality of life. This multifaceted approach may result in more valuable than simply providing financial incentives.4 As these measures may translate into an improvement in PC trainees’ retention, the patients’ quality of care should also improve as PCP availability in the communities has been associated with better health costs and outcomes.3,4,6
This study has some limitations. Only respondents from PR were surveyed, so findings may not generalize to students from other locations. Additionally, some applicants do not match their favored program, thus leaving the potential for bias when completing the questionnaire. Based on our results, future studies could consider a comprehensive assessment of strategies to retain medical students in PC programs in PR. Similarly, our data could be a fundamental ground for investigation by the medical schools in PR as student selection based on the highlighted factors may play a role in retaining our future PC workforce. Finally, measures to increase the number of medical students choosing PC programs should be considered another imperative topic of investigation.
Our study showed the significant influence that personal factors have in the decision of MS-PR to pursue a PC training program in the C-US. These findings represent a challenge for the local government and the medical schools as these factors are essentially nonmodifiable. However, addressing complementary issues such as technology access, training quality, and research funding may have potential benefits to minimize the exodus of the MS-PR.
Acknowledgments
The authors are deeply grateful to Dr. Gerardo Olivella and Dr Lenny Rivera from the Department of Orthopaedic Surgery at the University of Puerto Rico for their assistance in this study’s survey distribution and statistical coordination.
References
- Chan SC, Ganeson JV, Ong JT, Sugathan S. Perceptions of Malaysian medical students from different academic years on primary care: a qualitative research. Fam Med Community Health. 2020;8(1):e000188. doi:10.1136/fmch-2019-000188
- Grandes G, Sanchez A, Montoya I, Ortega Sanchez-Pinilla R, Torcal J, Group P; PEPAF Group. Two-year longitudinal analysis of a cluster randomized trial of physical activity promotion by general practitioners. PLoS One. 2011;6(3):e18363. doi:10.1371/journal.pone.0018363
- Basu S, Berkowitz SA, Phillips RL, Bitton A, Landon BE, Phillips RS. Association of primary care physician supply with population mortality in the United States, 2005-2015. JAMA Intern Med. 2019;179(4):506-514. doi:10.1001/jamainternmed.2018.7624
- Pfarrwaller E, Sommer J, Chung C, et al. Impact of interventions to increase the proportion of medical students choosing a primary care career: a systematic review. J Gen Intern Med. 2015;30(9):1349-1358. doi:10.1007/s11606-015-3372-9
- IHS-Markit-Ltd. The complexities of physician supply and demand: Projections from 2019 to 2034. Washington, DC: Association of American Medical Colleges. 2021. Accessed April 7, 2022. https://www.aamc.org/media/54681/download
- Starfield B, Shi L, Macinko J. Contribution of primary care to health systems and health. Milbank Q. 2005;83(3):457-502. doi:10.1111/j.1468-0009.2005.00409.x
- Kao AC, Jager AJ. Medical students’ views of medicine as a calling and selection of a primary care-related residency. Ann Fam Med. 2018;16(1):59-61. doi:10.1370/afm.2149
- Pfarrwaller E, Audétat MC, Sommer J, et al. An expanded conceptual framework of medical students’ primary care career choice. Acad Med. 2017;92(11):1536-1542. doi:10.1097/ACM.0000000000001676
- Wilkinson E, Killeen D, Pérez-López GJ, Jabbarpour Y. A shrinking primary care workforce in Puerto Rico. Am Fam Physician. 2020;101(1):13-14.
- Messinger CJ, Hafler J, Khan AM, Long T. Recent trends in primary care interest and career choices among medical students at an academic medical institution. Teach Learn Med. 2017;29(1):42-51. doi:10.1080/10401334.2016.1206825
- United-Health-Foundation. America’s Health Rankings Annual Report. 2018. Accessed April 7, 2022. https://assets.americashealthrankings.org/app/uploads/ahrannual-2018.pdf
- Parés-Arroyo M. Peligrosa fuga de miles de médicos. El Nuevo Día. July 28, 2016. Accessed April 7, 2022. https://www.elnuevodia.com/noticias/locales/notas/peligrosa-fuga-de-miles-de-medicos/
- Blissett S, Law C, Morra D, Ginsburg S. The relative influence of available resources during the residency match: a national survey of canadian medical students. J Grad Med Educ. 2011;3(4):497-502. doi:10.4300/JGME-D-11-00043.1
- Cochran A, Melby S, Neumayer LA. An Internet-based survey of factors influencing medical student selection of a general surgery career. Am J Surg. 2005;189(6):742-746. doi:10.1016/j.amjsurg.2005.03.019
- Mihalynuk T, Snadden D, Bates J, Scott I, Frinton V, Wilson G. Size matters: what influences medical students’ choice of study site? Med Teach. 2008;30(4):e108-e114. doi:10.1080/01421590801931170
- Weissman C, Zisk-Rony RY, Avidan A, Elchalal U, Tandeter H. Challenges to the Israeli healthcare system: attracting medical students to primary care and to the periphery. Isr J Health Policy Res. 2018;7(1):28. doi:10.1186/s13584-018-0218-z



There are no comments for this article.