Objectives: Safety practices such as storing a firearm locked and unloaded are widely promoted although not universally applied. Educating patients about firearm safety practices is effective in increasing safe firearms storage behaviors; however, screening for safe firearm storage in practice remains low. The aim of this study was to evaluate whether our clinic population was at risk for firearm-related injuries and whether opportunities existed to study risk-mitigation interventions in future work.
Methods: The study was conducted at a suburban, midwestern academic family medicine clinic. Patients filled out paper surveys about firearm ownership and willingness to discuss firearms safety with clinicians. Health care personnel filled out paper or electronic surveys about their comfort level in discussing firearm safety with patients. Data then were collated and analyzed.
Results: We surveyed 160 patients (60% female, 80% White), and 40.6% of respondents reported living in a home with a firearm. Respondents who stored their firearm unsafely were more willing to discuss firearm safety than to change their storage behavior. Eighteen health care personnel responded to our health care personnel survey. Perceived barriers to asking about firearms included lack of time, knowledge, or educational materials. Having a screening policy was selected as the best opportunity for improvement.
Conclusions: Firearm owners appear willing to discuss firearm safety with their clinician, potentially representing an opportunity to promote risk-reduction through approaches such as motivational interviewing. In a busy outpatient setting, automating the firearm screening process could lessen the burden on clinicians.
In 2020, the United States had 45,222 firearm-related deaths.1 More than half were suicides.1 For ages 1 through 44 years, firearms are among the top five leading causes of death in the United States.1 Although overall suicide rates in the United States are similar to other countries, the use of firearms in suicides is eight times higher in the United States.2 Nationally, household firearm ownership rates vary by geographic region from 10% to 60% with a mean of 40%.3,4 In the Midwest, 50% of US adults have reported living in a household with a firearm.5 Studies have shown that reducing access to lethal means can decrease deaths by suicide, especially among populations at higher risk of suicide, such as children, older White men, and veterans.6–11
Studies also have indicated that firearm safety screening can be an effective way to increase safe storage.12–15 However, in practice, screening rates are low.16,17 Additionally, patients’ attitudes toward firearm screening range widely.16,18
The aim of this study was to evaluate whether our clinic population was at risk for firearm-related injuries due to unsafe firearm storage and whether an opportunity existed to study risk-mitigation interventions in future work. Therefore, we collected data on patient attitudes and practices around firearm ownership, and health care personnel’s attitudes and practices around firearm safety screening and counseling in a primary care setting.
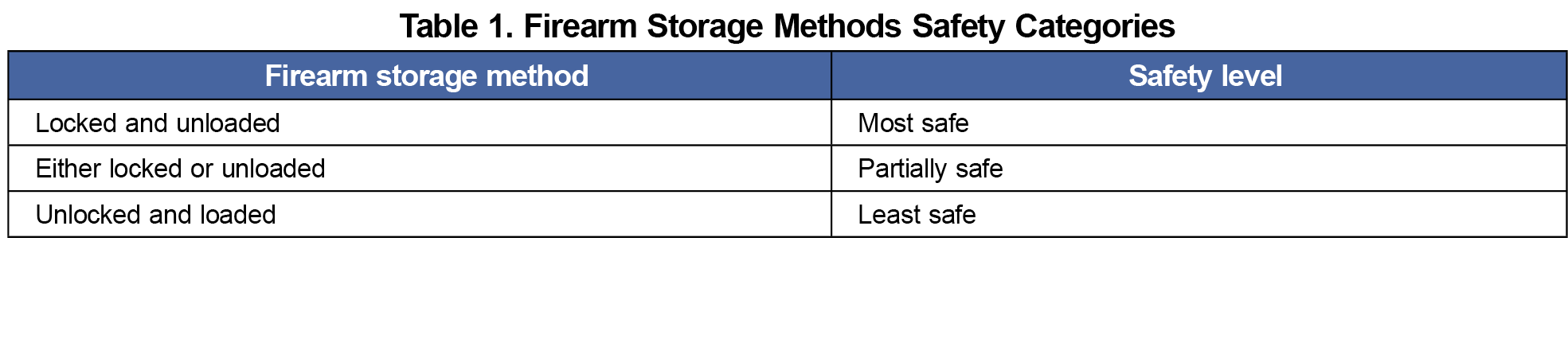
We invited patients at a suburban, midwestern academic family medicine practice to complete an author-developed paper survey on firearm ownership and willingness to discuss firearms safety with health care personnel. Those living in a firearm household were asked how their firearms were stored (Table 1). Health care personnel in the same office were asked to complete a survey, modified from a published nursing survey,19 either on paper or via REDCap (Research Electronic Data Capture) about their attitudes toward and familiarity with firearm safety. Data were collated in REDCap and analyzed in SAS version 9.4 (SAS Institute).
Survey participation was voluntary and confidential. We administered the surveys from August to December 2021. This study was determined by the Wright State University Institutional Review Board to be exempt from review. We calculated categorical percentages to quantify responses. We also calculated frequencies and percentages for categorical variables and means and standard deviations for continuous variables to describe the participant’s responses. Although the purpose of the study was descriptive in nature, we conducted secondary subgroup analyses using χ2, Fisher’s exact tests, and analysis of variance (ANOVA).
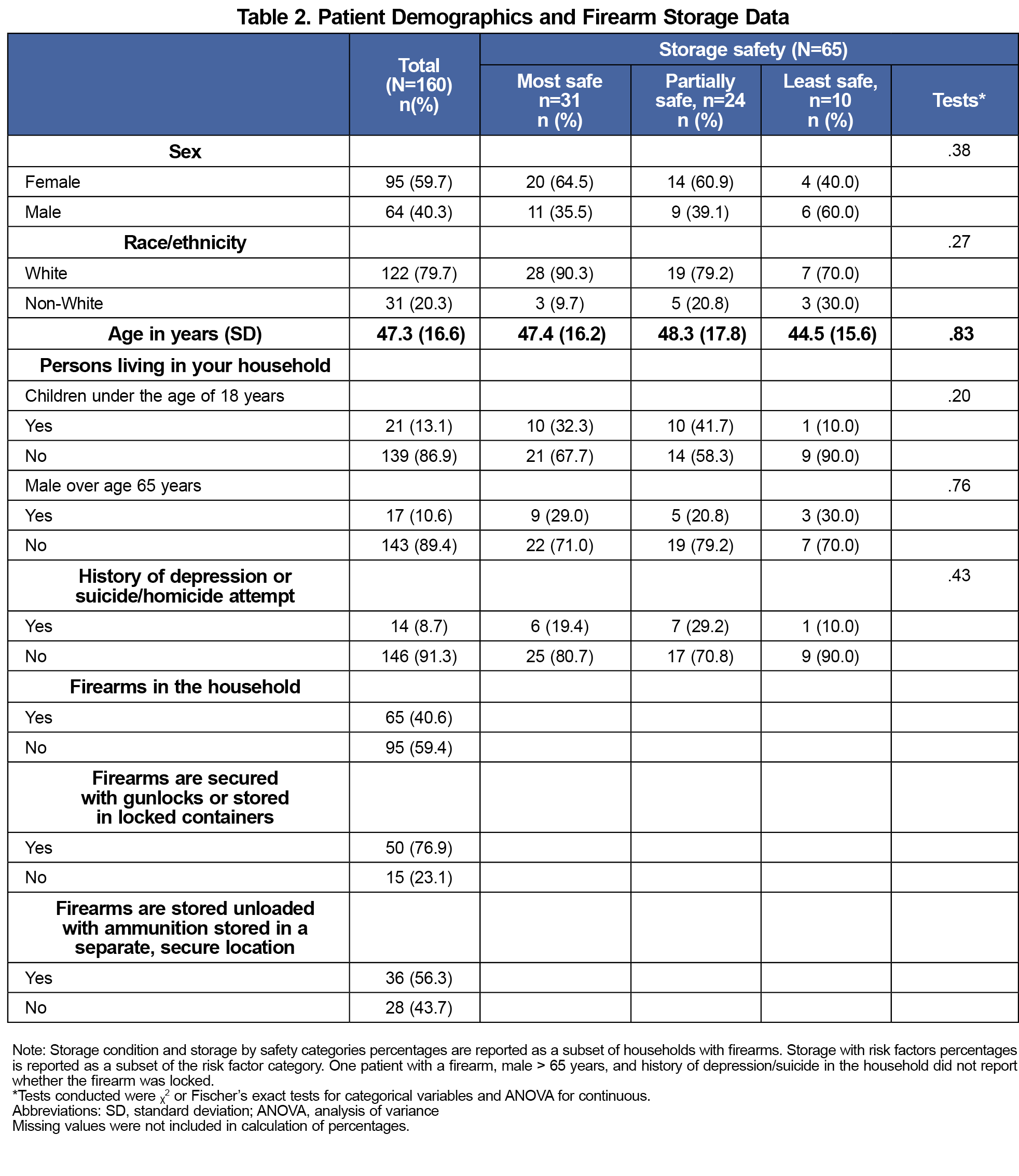
A total of 160 patient surveys were collected. Eighty percent of respondents identified as White and 60% were female. Forty percent (n=65) of respondents lived in a home with firearms. Approximately 48% of respondents with firearms in the household had the safest storage arrangement (locked and unloaded). We found no differences in storage safety by subgroups, nor any significant differences between groups on the traits we measured (Table 2).
More than half (55%) of patients who lived in a home with a firearm reported willingness to discuss firearm safety with their clinician. For patients that did not store their firearm either locked or unloaded, only 35% and 23%, respectively, were willing to change their storage practice. Only 18% of respondents with firearms reported willingness to remove their firearms from their home for safety, and 64% were unwilling to remove their firearms.
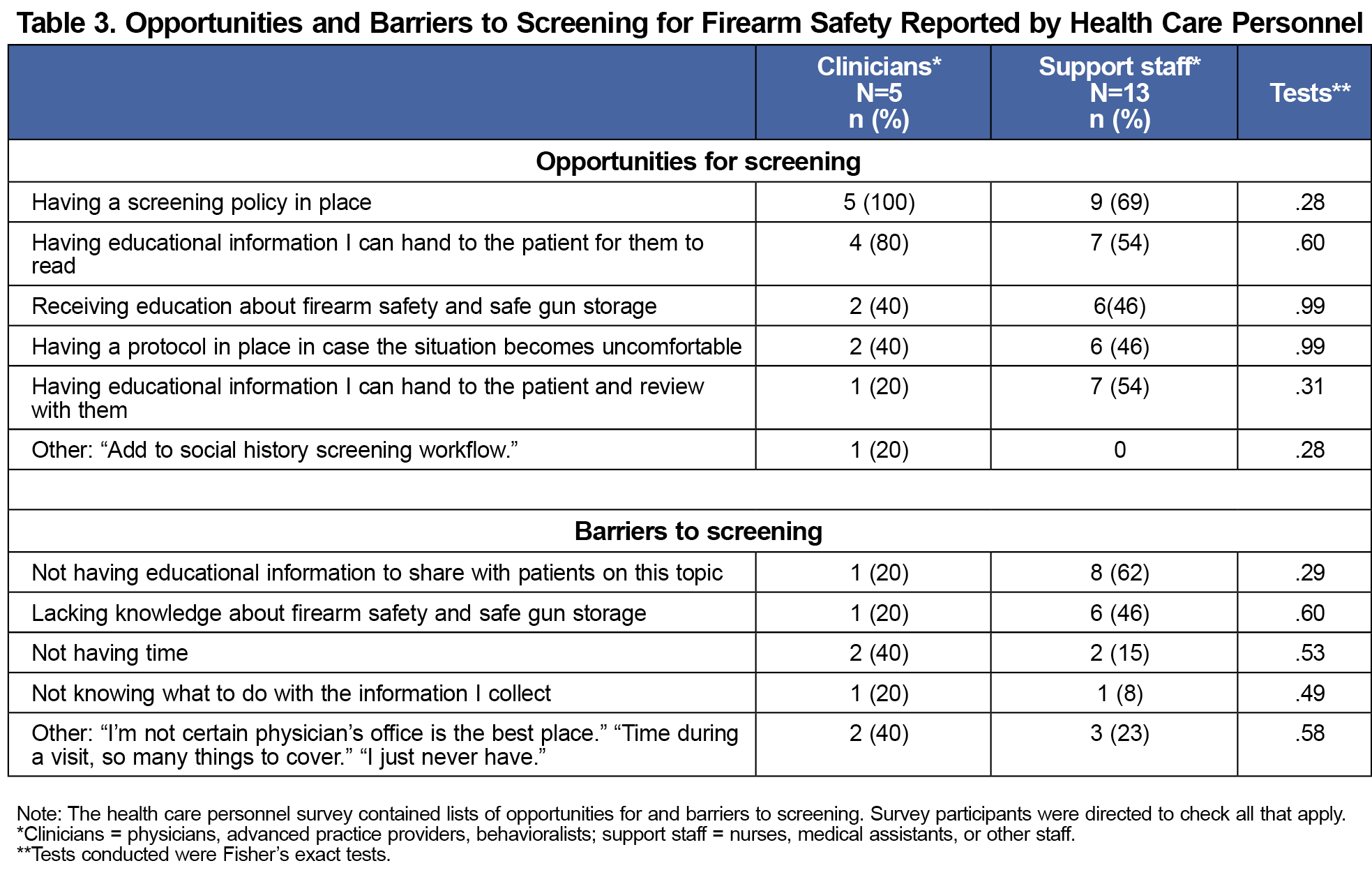
A total of 20 health care personnel surveys were collected. Five were physicians, advanced practice providers, or behavioralists. Thirteen were nurses, medical assistants, or other staff. We excluded two respondents because they had no direct patient care. Only 33% of health care personnel asked patients about firearms. However, 61% of health care personnel were comfortable with the idea of asking about firearms in the home. Table 3 provides a summary of health care personnel’s perceived barriers to firearms screening as well as their preferences for improving screening rates.
More than 50% of our patient population in firearm households indicated willingness to engage in a conversation about firearm safety with their clinician, a largely positive result that aligns with studies done in pediatric populations16 and with a recent study in the veteran population,18 suggesting that our patient population may be receptive to further safe firearm storage interventions. However, our data also suggested that even though patients reported being willing to have a conversation with a clinician about firearm storage, their preconversation willingness to change their storage method was low. This unwillingness possibly is related to the reasons patients choose to own guns. The primary reasons for firearm ownership are first safety and then recreation, and firearms are viewed as a symbol of freedom and safety.20 This deeply held belief persists despite multiple studies that have shown that living in a household without a gun or where a firearm is safely stored reduces the likelihood of death by firearms.6–9,21
In spite of this low willingness to change, studies that have included counseling, motivational interviewing principles, or support aids such as gun locks or cabinets have shown promising results for behavior change in firearm safety, especially in pediatrics.14 Using motivational interviewing as a tool to support behavioral change has a history of positive outcomes for other high-risk behaviors.22 Future studies could explore motivational interviewing as an intervention to increase firearm safety practices.
Another avenue for improving screening and interventions is focusing on reducing barriers for health care personnel. Educational information, directed toward either the public or health care setting, is continuing to be developed.23 With more information and tools, clinicians may feel more comfortable directing risk identification and intervention around firearm access and lethal means safety.24 As advocacy for this important initiative continues, clinicians may continue to recognize its importance and dedicate time to address this topic during office visits.
A strength of our study was using a previously developed survey tool and assessing the views and opinions of multiple stakeholders, namely patients as well as health care personnel in a diverse range of clinical roles, in a single clinic setting. However, because patients and health care personnel self-selected to participate in the surveys, the results may be skewed. Forty percent of our self-selected patient population reported living in a household with firearms, which reflects the national average for household firearm ownership but is likely lower than the expected mean for a clinic in a suburb of a midwestern city with a high military and veteran population. Because our sample was not random, our results are possibly skewed toward a population of firearm owners more favorable to conversations with clinicians about firearm safety. Additionally, our sample sizes were small, limiting subgroup analyses; current analyses should therefore be interpreted with caution. The patient survey did not differentiate between firearm owners and those living in a household with firearms; these two populations may have different views.
Overall, our study suggests that further research in the primary care setting about screening and interventions for safe firearm storage is warranted. Such research should include the development of appropriate and effective screening and intervention strategies, and how to best incorporate these processes given the barriers that health care personnel face. Many factors have been identified that affect the choices individuals make regarding firearm ownership and how firearms are stored, as well as perceptions of risk.25,26 Therefore, patient-centered approaches (eg, motivational interviewing) that consider individuals’ own reasons for their choices deserve particular attention in future studies.
Acknowledgments
The authors thank the Wright State University (WSU) Department of Family Medicine and the staff of the Wright State Physicians Family Medicine practice for their support of this project. The previous work on this topic completed by Dr Tyler Luonuansuu when he was a WSU Boonshoft School of Medicine medical student is gratefully acknowledged.
Presentations:
Nguyen A, Owens G, Conway K, Hershberger P, Crawford T. Prevalence of firearm ownership in Wright State Physicians patients and attitude toward firearm safety screening. Poster presented at: First Annual Boonshoft School of Medicine Research Symposium; April 6, 2022; Dayton, OH.
Nguyen A, Owens G, Conway K, Hershberger P, Crawford T. Prevalence of firearm ownership in Wright State Physicians patients and attitude toward firearm safety screening. Poster presented at: American Medical Student Association Annual Convention & Exposition; April 9, 2022; Alexandria, VA.
Nguyen, A, Owens, G, Conway, K, Hershberger, P, Crawford, T. Primary care office staff’s attitudes toward firearm safety screening. Poster presented at: 2022 Ohio/Air Force Scientific Meeting; October 21, 2022; Columbus, OH.
References
- Centers for Disease Control and Prevention. Firearm violence prevention. Accessed January 17, 2023. https://www.cdc.gov/violenceprevention/firearms/fastfact.html
- Grinshteyn E, Hemenway D. Violent death rates: The US compared with other high-income OECD countries, 2010. Am J Med. 2016;129(3):266-273. doi:10.1016/j.amjmed.2015.10.025
- Kivisto AJ, Magee LA, Phalen PL, Ray BR. Firearm ownership and domestic versus nondomestic homicide in the U.S. Am J Prev Med. 2019;57(3):311-320. doi:10.1016/j.amepre.2019.04.009
- Kivisto AJ, Kivisto KL, Gurnell E, Phalen P, Ray B. Adolescent suicide, household firearm ownership, and the effects of child access prevention laws. J Am Acad Child Adolesc Psychiatry. 2021;60(9):1,096-1,104. doi:10.1016/j.jaac.2020.08.442
- Saad L. What percentage of Americans own guns? Gallup. November 13, 2020. Accessed January 10, 2022. https://news.gallup.com/poll/264932/percentage-americans-own-guns.aspx
- Kellermann AL, Rivara FP, Somes G, et al. Suicide in the home in relation to gun ownership. N Engl J Med. 1992;327(7):467-472. doi:10.1056/NEJM199208133270705
- Conwell Y, Duberstein PR, Connor K, Eberly S, Cox C, Caine ED. Access to firearms and risk for suicide in middle-aged and older adults. Am J Geriatr Psychiatry. 2002;10(4):407-416. doi:10.1097/00019442-200207000-00007
- Grossman DC, Mueller BA, Riedy C, et al. Gun storage practices and risk of youth suicide and unintentional firearm injuries. JAMA. 2005;293(6):707-714. doi:10.1001/jama.293.6.707
- Miller M, Lippmann SJ, Azrael D, Hemenway D. Household firearm ownership and rates of suicide across the 50 United States. J Trauma. 2007;62(4):1,029-1,034. doi:10.1097/01.ta.0000198214.24056.40
- Azrael D, Miller MJ. Reducing suicide without affecting underlying mental health. In: O’Connor RC, Pirkis J, eds. The International Handbook of Suicide Prevention. 2nd ed. Wiley; 2016:637-662. doi:10.1002/9781118903223.ch36
- Monuteaux MC, Azrael D, Miller M. Association of increased safe household firearm storage with firearm suicide and unintentional death among US youths. JAMA Pediatr. 2019;173(7):657-662. doi:10.1001/jamapediatrics.2019.1078
- Albright TL, Burge SK. Improving firearm storage habits: impact of brief office counseling by family physicians. J Am Board Fam Pract. 2003;16(1):40-46. doi:10.3122/jabfm.16.1.40
- Carbone PS, Clemens CJ, Ball TM. Effectiveness of gun-safety counseling and a gun lock giveaway in a Hispanic community. Arch Pediatr Adolesc Med. 2005;159(11):1,049-1,054. doi:10.1001/archpedi.159.11.1049
- Rowhani-Rahbar A, Simonetti JA, Rivara FP. Effectiveness of interventions to promote safe firearm storage. Epidemiol Rev. 2016;38(1):111-124. doi:10.1093/epirev/mxv006
- Ngo QM, Sigel E, Moon A, et al; FACTS Consortium. State of the science: a scoping review of primary prevention of firearm injuries among children and adolescents. J Behav Med. 2019;42(4):811-829. doi:10.1007/s10865-019-00043-2
- Roszko PJD, Ameli J, Carter PM, Cunningham RM, Ranney ML. Clinician attitudes, screening practices, and interventions to reduce firearm-related injury. Epidemiol Rev. 2016;38(1):87-110. doi:10.1093/epirev/mxv005
- Bond AE, Moceri-Brooks J, Rodriguez TR, Semenza D, Anestis MD. Determining who healthcare providers screen for firearm access in the United States. Prev Med. 2023;169:107476. doi:10.1016/j.ypmed.2023.107476
- Newell S, Kenyon E, Clark KD, et al. Veterans are agreeable to discussions about firearms safety in primary care. J Am Board Fam Med. 2021;34(2):338-345. doi:10.3122/jabfm.2021.02.200261
- Smith Sheppard K, Hall K, Carney J, et al. Nurses’ knowledge and comfort with assessing inpatients’ firearm access and providing education on safe gun storage: findings from a study among hospital staff nurses. AJN Am J Nurs. 2020;120(9):26-35. doi:10.1097/01.NAJ.0000697636.34423.45
- Siegel MB, Boine CC. The meaning of guns to gun owners in the U.S.: The 2019 national lawful use of guns survey. Am J Prev Med. 2020;59(5):678-685. doi:10.1016/j.amepre.2020.05.010
- Kellermann AL, Rivara FP, Rushforth NB, et al. Gun ownership as a risk factor for homicide in the home. N Engl J Med. 1993;329(15):1,084-1,091. doi:10.1056/NEJM199310073291506
- Frost H, Campbell P, Maxwell M, et al. Effectiveness of motivational interviewing on adult behaviour change in health and social care settings: A systematic review of reviews. PLoS One. 2018;13(10):e0204890. doi:10.1371/journal.pone.0204890
- Betz ME, Thomas AC, Simonetti JA. Firearms, suicide, and approaches for prevention. JAMA. 2022;328(12):1,179-1,180. doi:10.1001/jama.2022.16663
- Pallin R, Barnhorst A. Clinical strategies for reducing firearm suicide. Inj Epidemiol. 2021;8(1):57. doi:10.1186/s40621-021-00352-8
- Simonetti JA, Brenner LA. Promoting firearm safety as a suicide prevention strategy within health care systems: challenges and recommendations. Psychiatr Serv. 2020;71(3):298-300. doi:10.1176/appi.ps.201900286
- Butterworth SE, Daruwala SE, Anestis MD. The role of reason for firearm ownership in beliefs about firearms and suicide, openness to means safety, and current firearm storage. Suicide Life Threat Behav. 2020;50(3):617-630. doi:10.1111/sltb.12619