Introduction: Osteoporosis is a prevalent condition associated with reduced bone density and increased fracture risk, yet many patients rely on online health information to guide lifestyle management. This study aimed to evaluate the quality and accessibility of consumer health websites providing information on osteoporosis lifestyle modifications.
Methods: A systematic Google search identified the first 150 websites, with 85 websites eligible for inclusion. After review of several national guidelines, we established four lifestyle domains: calcium/vitamin D supplementation, fall prevention, exercise, and smoking cessation. Two independent reviewers assessed each website using the DISCERN instrument, which examines the quality of written consumer health information.
Results: The mean DISCERN score was 50.7±9.71 (out of 80). Of the 85 websites, 7 (8.2%) were rated as excellent, 41 (48.2%) as good, 31 (36.5%) as fair, 5 (5.9%) as poor, and 1 (1.2%) as very poor. Accessibility features were limited, with 7.8% offering translation and 31.8% incorporating multimedia content.
Conclusions: These findings demonstrate considerable variability in quality and highlight gaps in accessibility. Improvements in guideline-based recommendations, transparency, and reliability can support more equitable osteoporosis care.
Osteoporosis is a widespread reduction in bone density and mass, leading to compromised bone strength and increased fracture risk.1 In 2021, the global prevalence reached 18.3%, and in the United States, 21% of older adults had osteoporosis in the hip or spine.2-4 Because osteoporosis remains silent until fractures occur, early diagnosis and lifestyle management are essential to prevent progression.1 Fractures often serve as the sentinel event in diagnosing osteoporosis and create long-term economic, morbidity, and mortality burdens.5 To prevent these complications, clinicians must promote evidence-based lifestyle modifications, such as adequate calcium and vitamin D intake, frequent weight-bearing exercises, fall prevention, smoking cessation, and moderation of alcohol use.6,7
Many patients turn to the Internet for health-related information, yet the quality, accuracy, and accessibility of online resources vary widely.8 Incomplete information and poor reliability may undermine patient engagement or adherence.9 Evidence has shown that populations with lower health literacy rates often face social factors that hinder optimal bone health, such as dietary deficiencies or reduced opportunities for physical activity; therefore, significant disparities persist in osteoporosis screening, diagnosis, and treatment.10 These disparities raise concerns about whether online resources are accessible or effective for higher-risk groups.
This study aimed to evaluate the quality and accessibility of online health information on lifestyle changes for osteoporosis and identified areas for improvement to better support patient education, equity, and care for individuals affected by or at risk for the disease.
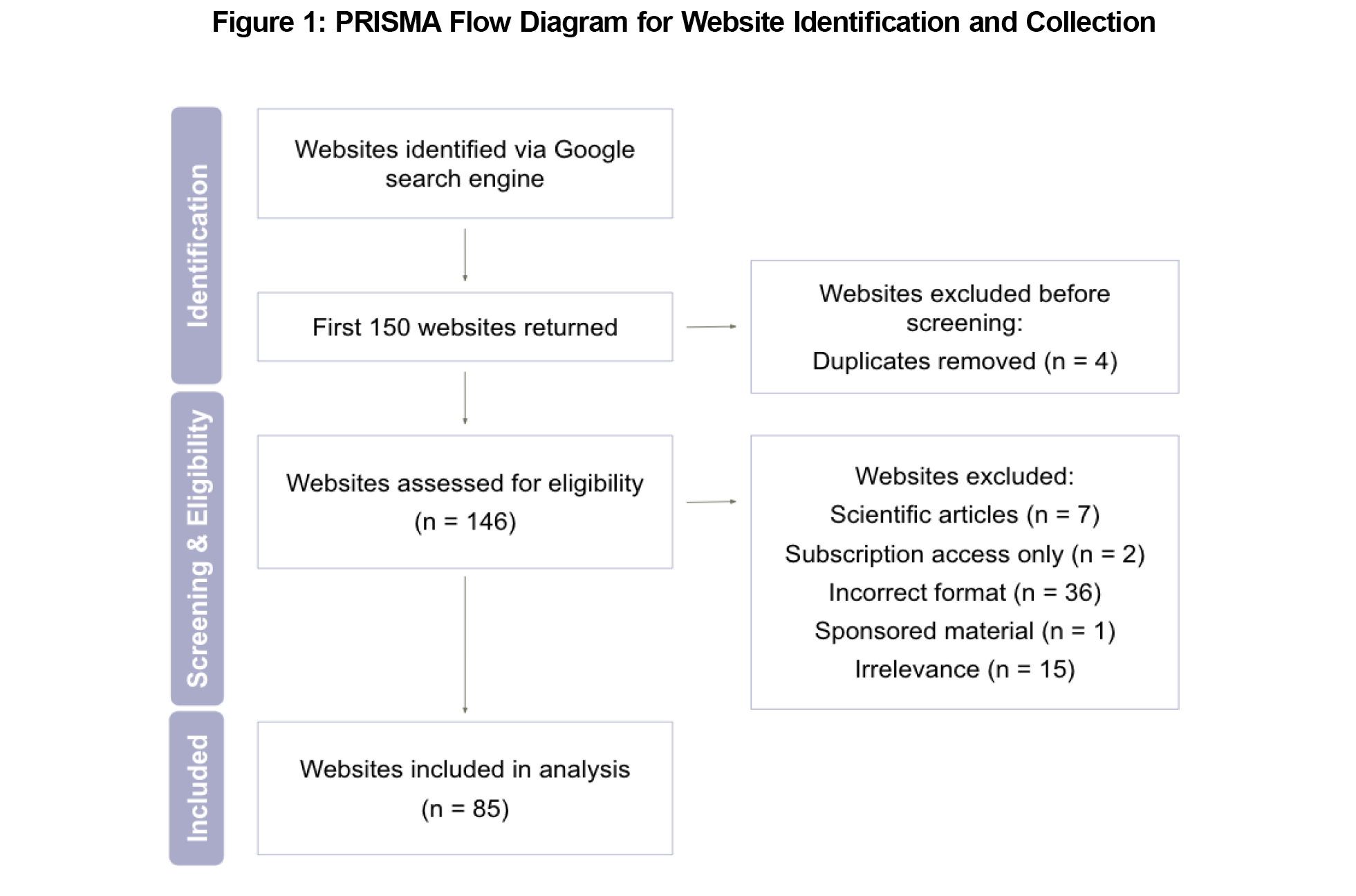
The institutional review board declared our study exempt. The authors first defined essential lifestyle modifications based on current national and international osteoporosis guidelines and selected four domains as the gold standard for scoring: calcium and vitamin D supplementation, fall prevention, exercise recommendations, and smoking cessation. We then conducted a Google Chrome search in incognito mode with default English settings using the term “osteoporosis lifestyle changes” to replicate a typical patient query. We screened the first 150 websites. Websites were excluded if they were scientific journals, required a subscription, were in an incorrect format (eg, videos), consisted of sponsored material, or were not relevant to lifestyle modifications for osteoporosis. A total of 85 websites were eligible for analysis following exclusion (Figure 1).
Two blinded, independent reviewers evaluated each website using DISCERN, a validated 16-item tool that assesses quality of consumer health information.11 Each item is scored from 1 (low quality) to 5 (high quality), then summed (maximum score of 80). Reviewers resolved discrepancies through consensus, then calculated average scores to classify a website’s quality into five tiers: excellent (≥65), good (55–64), fair (45–54), poor (35-44), and very poor (<35). The interrater reliability score was 0.94, indicating excellent agreement. Website accessibility was evaluated for language translations and multimedia components, features that enhance user engagement, and comprehension.12,13 Language translation was defined as the presence of a website-provided option listing the availability of translated content. Multimedia components were recorded as the presence of video, audio, interactive tools, or descriptive images (eg, labeled diagrams or infographics).
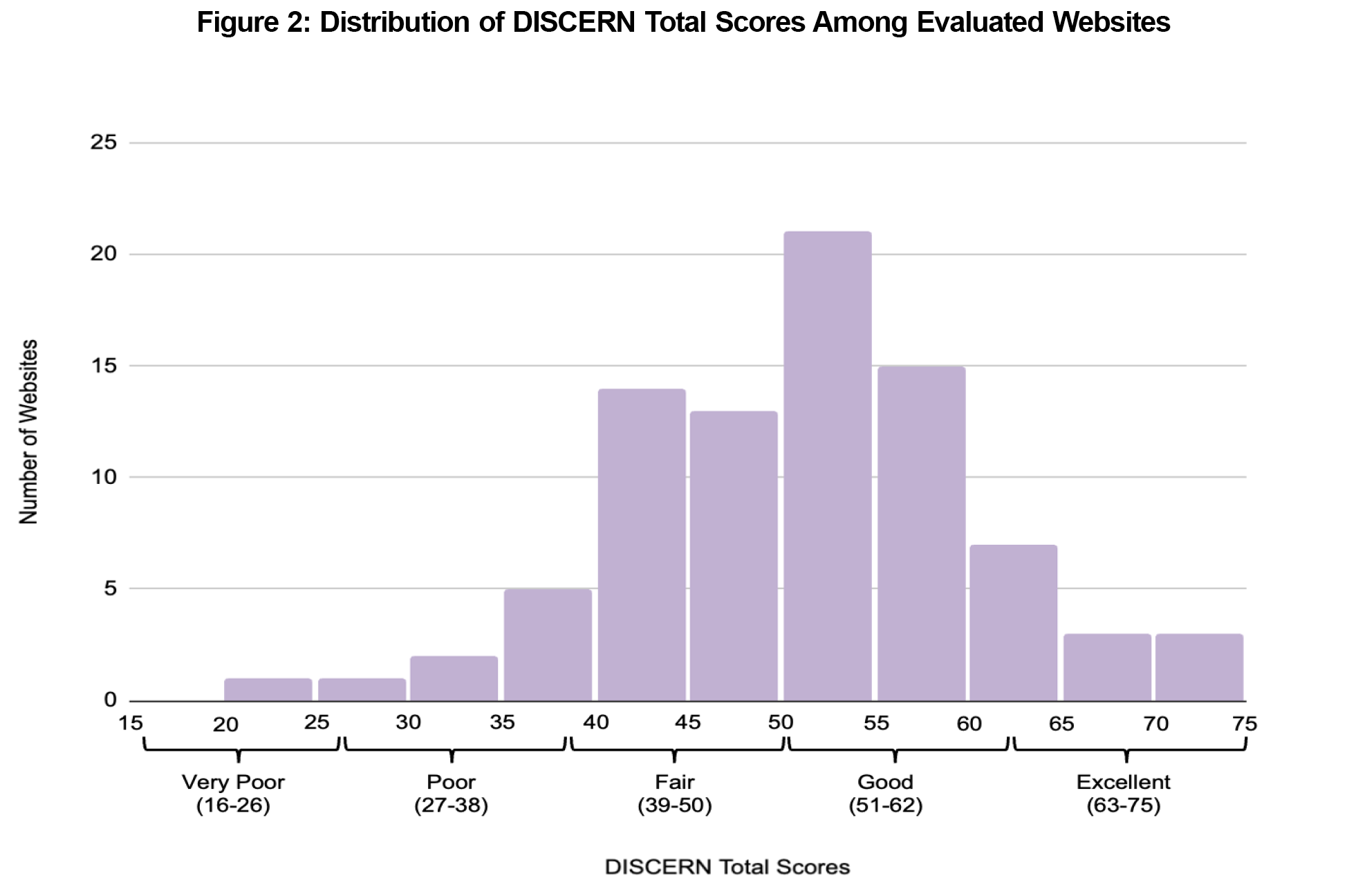
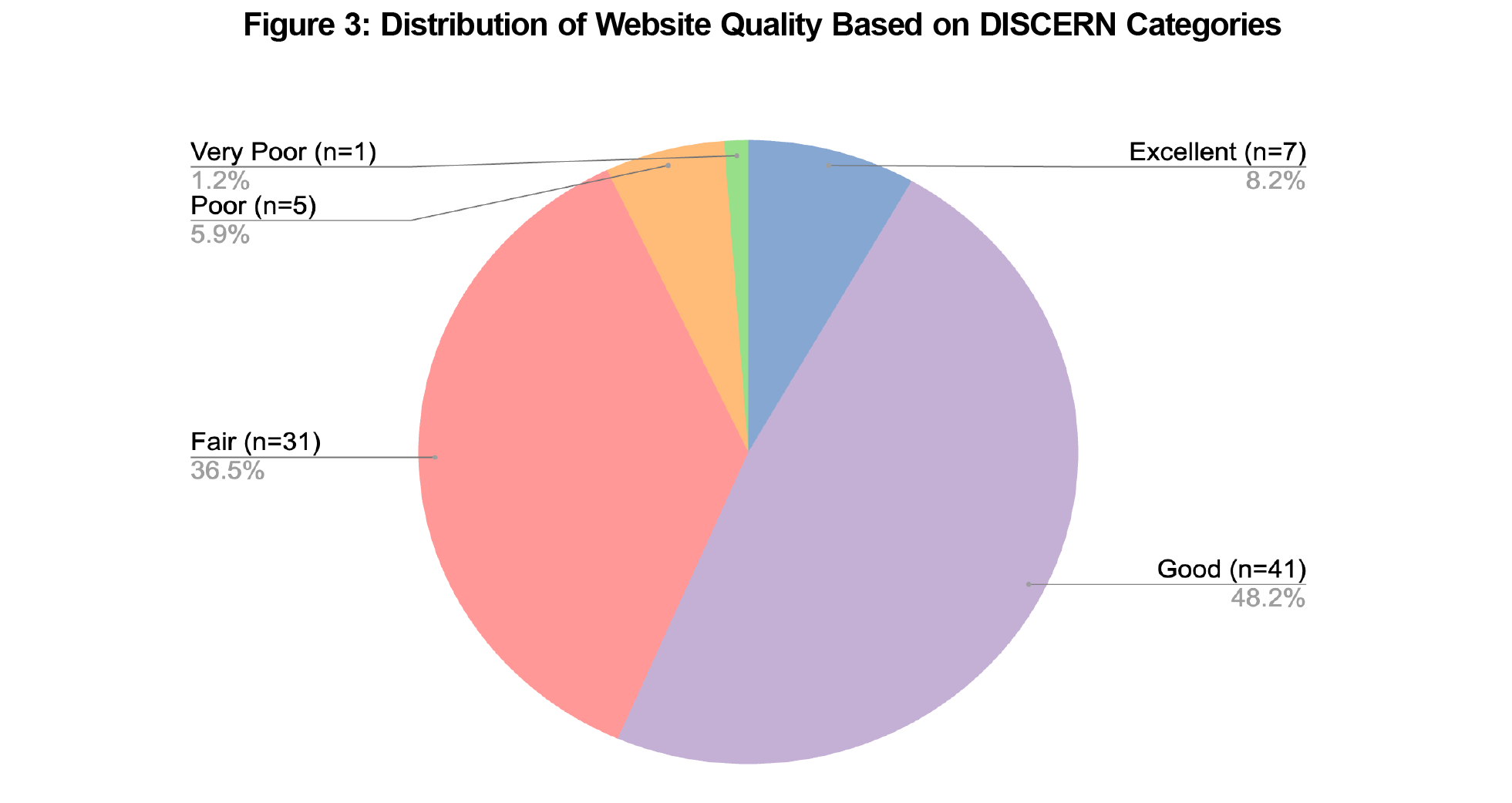
The mean DISCERN score was 50.7±9.71, indicating an overall fair quality of patient information on osteoporosis lifestyle modifications (Figure 2). Out of 85 websites, 7 (8.2%) were graded as excellent, 41 (48.2%) as good, 31 (36.5%) as fair, 5 (5.9%) as poor, and 1 (1.2%) as very poor (Figure 3).
Websites generally offered several prevention strategies, detailed descriptions, and benefits of lifestyle changes. However, citing sources, providing publication dates, and addressing risks or uncertainties of each recommendation were all low-scoring areas.
Only 7.8% of websites provided information in languages other than English. Furthermore, 31.8% of websites included multimedia elements, including videos (n=8), descriptive images (n=20), interactive images (n=2), and audio clips (n=3), with some websites containing multiple types of content.
This study systematically evaluated the quality and accessibility of web-based patient education on lifestyle modifications for osteoporosis. Our findings revealed substantial variability across resources, with most achieving moderate quality but only a 12th reaching excellence, indicating a discrepancy between available information and national osteoporosis standards. While many websites convey practical recommendations, they appear to lack transparency or updated evidence, which limits their reliability. This finding raises concerns given the prevalence and preventable nature of osteoporosis.
The inconsistency in website quality parallels previous investigations for other chronic diseases, such as diabetes and cardiovascular disease, where lack of citation transparency and evidence-based recommendations were observed.14,15 Given that many patients rely on the Internet before or in place of consulting a health care professional, improving the quality and credibility of online health information represents an important public health priority.16,17
Accessibility limitations further compound these issues. The minimal incorporation of multilingual support and multimedia content restricts these resources from non-English speakers and individuals with lower health literacy, populations that already face barriers to osteoporosis prevention and treatment.18 This finding underscores a missed opportunity to promote engagement and understanding through proven, multimodal approaches.19 Improving this aspect of osteoporosis education may enhance patient engagement and ultimately reduce the burden of osteoporosis-related fractures.
Several limitations should be acknowledged. Our analysis was restricted to English-language searches using a single search engine, which may not capture all available resources or algorithm differences. Additionally, although DISCERN is a validated instrument, it evaluates content quality rather than usability or design, which are also critical components of effective digital education.20 Moreover, while our study identified four domains as the gold standard, our results did not quantify the extent to which each website addressed these individual criteria, limiting insight into which areas are most underrepresented. Finally, while our study emphasized health literacy, we did not apply formal readability metrics such as Flesch-Kincaid or SMOG. Our primary focus was evidence-based quality as measured by DISCERN; however future research should integrate readability metrics with quality assessment to provide a comprehensive evaluation of web-based education materials.
Our study is among the few that evaluated web-based information on osteoporosis lifestyle modification, rather than pharmacologic management. Prior research assessed the readability of online information focused primarily on osteoporosis and drug treatment.9 In contrast, our analysis specifically centered on lifestyle modification content, a cornerstone of both prevention and long-term management. Rather than emphasizing readability metrics, we used the DISCERN instrument to evaluate content quality and further assessed accessibility features. By using DISCERN and reporting accessibility features, we highlighted actionable areas for improvement. Patient education websites should strive to reflect the national guidelines for lifestyle recommendations, provide clear citations, and thoroughly discuss risks versus benefits. Addressing these gaps is an essential step toward reducing health disparities and improving outcomes in osteoporosis care.
Online patient education regarding lifestyle modifications for osteoporosis are highly variable in quality, with the majority scoring only moderate in quality. Accessibility is also limited, with minimal multilingual support and multimedia elements, which may disproportionately impact populations at higher risk for poor bone health. By identifying gaps in both content and accessibility, we demonstrated the need for websites to adhere to national lifestyle guidelines and employ strategies that improve transparency, comprehensiveness, and usability. Enhancing the quality and accessibility of web-based health information can support patient engagement, promote preventive behaviors, and reduce outcome disparities.
Acknowledgments
Conflicts of Interest: The authors have no conflicts of interest to declare.
Presentations:
This study was presented at the following venues:
- National Student Research Forum, April 5, 2025, Galveston, Texas.
- Texas Academy of Family Physicians Annual Session and Primary Care Summit, November 15, 2025, Addison, Texas.
References
- Sözen T, Özışık L, Başaran NC. An overview and management of osteoporosis. Eur J Rheumatol. 2017;4(1):46-56. doi:10.5152/eurjrheum.2016.048
- Salari N, Ghasemi H, Mohammadi L, et al. The global prevalence of osteoporosis in the world: a comprehensive systematic review and meta-analysis. J Orthop Surg Res. 2021;16(1):609-620. doi:10.1186/s13018-021-02772-0
- Wade SW, Strader C, Fitzpatrick LA, Anthony MS, O’Malley CD. Estimating prevalence of osteoporosis: examples from industrialized countries. Arch Osteoporos. 2014;9(1):182. doi:10.1007/s11657-014-0182-3
- U.S. Department of Health and Human Services. Bone Health and Osteoporosis: A Report of the Surgeon General. Office of the Surgeon General; 2004. https://www.ncbi.nlm.nih.gov/books/NBK45513
- Snodgrass P, Zou A, Gruntmanis U, Gitajn IL. Osteoporosis diagnosis, management, and referral practice after fragility fractures. Curr Osteoporos Rep. 2022;20(3):163-169. doi:10.1007/s11914-022-00730-1
- Anupama DS, Noronha JA, Acharya KKV, Prabhu M, Ravishankar N, Nayak BS. Effect of lifestyle modification intervention programme on bone mineral density among postmenopausal women with osteoporosis. Sultan Qaboos Univ Med J. 2023;23(3):387-393. doi:10.18295/squmj.1.2023.010
- Christianson MS, Shen W. Osteoporosis prevention and management: nonpharmacologic and lifestyle options. Clin Obstet Gynecol. 2013;56(4):703-710. doi:10.1097/GRF.0b013e3182a9d15a
- Swire-Thompson B, Lazer D. Public health and online misinformation: challenges and recommendations. Annu Rev Public Health. 2020;41(1):433-451. doi:10.1146/annurev-publhealth-040119-094127
- Crawford-Manning F, Greenall C, Hawarden A, et al. Evaluation of quality and readability of online patient information on osteoporosis and osteoporosis drug treatment and recommendations for improvement. Osteoporos Int. 2021;32(8):1,567-1,584. doi:10.1007/s00198-020-05800-7
- Wu Q, Dai J. Racial/ethnic differences in bone mineral density for osteoporosis. Curr Osteoporos Rep. 2023;21(6):670-684. doi:10.1007/s11914-023-00838-y
- Charnock D, Shepperd S, Needham G, Gann R. DISCERN: an instrument for judging the quality of written consumer health information on treatment choices. J Epidemiol Community Health. 1999;53(2):105-111. doi:10.1136/jech.53.2.105
- Karliner LS, Kim SE, Meltzer DO, Auerbach AD. Influence of language barriers on outcomes of hospital care for general medicine inpatients. J Hosp Med. 2010;5(5):276-282. doi:10.1002/jhm.658
- D’Souza V, Blouin E, Zeitouni A, Muller K, Allison PJ. Do multimedia based information services increase knowledge and satisfaction in head and neck cancer patients? Oral Oncol. 2013;49(9):943-949. doi:10.1016/j.oraloncology.2013.06.005
- Guan Y, Maloney KA, Roter DL, Pollin TI. Evaluation of the informational content, readability and comprehensibility of online health information on monogenic diabetes. J Genet Couns. 2018;27(3):608-615. doi:10.1007/s10897-017-0155-y
- Tahir M, Usman M, Muhammad F, et al. Evaluation of quality and readability of online health information on high blood pressure using DISCERN and Flesch-Kincaid tools. Appl Sci (Basel). 2020;10(9):3214. doi:10.3390/app10093214
- Jung M. Consumer health informatics: promoting patient self-care management of illnesses and health. Health Care Manag (Frederick). 2016;35(4):312-320. doi:10.1097/HCM.0000000000000130
- Sbaffi L, Rowley J. Trust and credibility in web-based health information: a review and agenda for future research. J Med Internet Res. 2017;19(6):e218. doi:10.2196/jmir.7579
- Ramirez N, Shi K, Yabroff KR, Han X, Fedewa SA, Nogueira LM. Access to care among adults with limited English proficiency. J Gen Intern Med. 2023;38(3):592-599. doi:10.1007/s11606-022-07690-3
- Henni SH, Maurud S, Fuglerud KS, Moen A. The experiences, needs and barriers of people with impairments related to usability and accessibility of digital health solutions, levels of involvement in the design process and strategies for participatory and universal design: a scoping review. BMC Public Health. 2022;22(1):35-18. doi:10.1186/s12889-021-12393-1
- Sisson SD, Hill-Briggs F, Levine D. How to improve medical education website design. BMC Med Educ. 2010;10(1):30. doi:10.1186/1472-6920-10-30



There are no comments for this article.