Introduction: Food pantries have been created in health care settings to directly address food insecurity. Little is known about how visitors might use food from a colocated pantry, what items are most useful, how a pantry may improve healthy choices, and the ongoing value of a food pantry in a family medicine office.
Methods: We interviewed 55 patients by phone 1 week after their visit to our clinic-based food pantry using a semistructured interview format. We performed a qualitative analysis of open-ended questions using an editing-organizing approach.
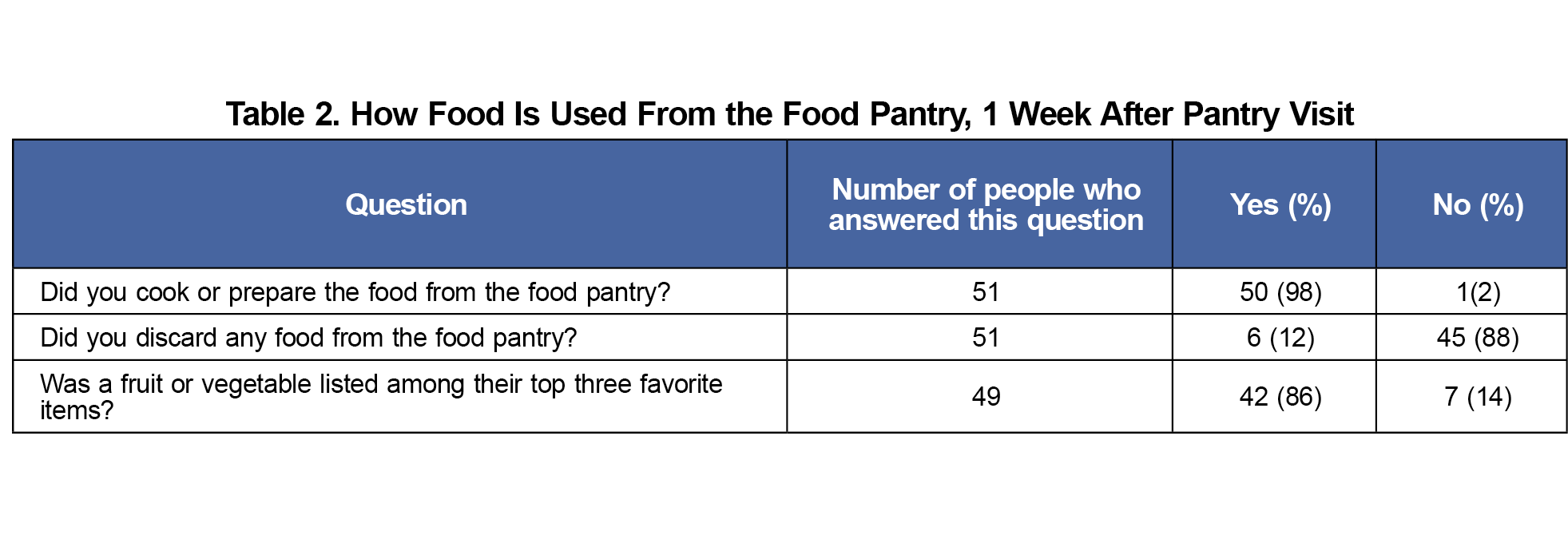
Results: Most participants cooked or prepared food from the pantry. Food was rarely discarded. A total of 35 of 49 (71%) used 75% or more of the food within 1 week. Fruits and vegetables were among the favorite items of most users. Qualitative themes included strong confidence in ability to cook, making health-conscious choices, taboo against food waste, comfort integrating items into their regular food habits, and the food pantry empowering people to make dietary changes.
Conclusions: A food pantry in a residency clinic is feasible, appreciated by visitors, and can help with nutritious food choices for those in need.
Social determinants of health (SDoH) have an important impact on health equity.1 The Accreditation Council for Graduate Medical Education requires residents in all specialties to be aware of and address SDoH.2 Some medical schools and residency programs have curricula to address SDoH.3,4 Food insecurity is an important SDoH; and one out of every eight people live in a household with food insecurity in the United States.5
Government programs and food pantries are available in most communities to address food insecurity. However, obtaining these resources has many barriers,6-10 and addressing food waste is an important challenge for food banks.11
Primary care offices may address food insecurity through community partnerships, screening, and referrals.12.13 Physicians and residency programs find connecting patients to resources challenging.14,15 People with food insecurity value emergency food boxes more than any other intervention.16 Some health systems and clinics have made food available directly where patients receive care.17-21
We recently described our experience opening a food pantry within a family medicine residency clinic.22 We established the Banner Family Food Pantry in April 2023 in Phoenix, Arizona. Family medicine residents have protected time and work with faculty, staff, and volunteers in collaboration with a local food bank and a local produce cooperative to maintain the pantry. From April 2023 through February 2026, the pantry provided fresh produce and healthy nonperishable food to 7,935 households and 24,309 individuals.
Our food pantry provides bagged items, preselected based on availability. Each bag contains approximately eight nonperishable items and four fresh fruit and vegetable items. Food bags may include at least one recipe for how to use the food contained in the bag. Our prior publication described barriers to healthy eating, why patients use the food pantry, and their appreciation for this colocated service.22 However, minimal published research exists on how patients use food pantry items, especially when obtained in a primary care office.
This study aimed to understand how patients use food from our pantry, which items are most useful, possible food waste, how the pantry may improve healthy choices, and the ongoing value of a food pantry in a family medicine office.
We gathered names and phone numbers of visitors to the Banner Family Food Pantry from June 3 to June 27, 2024. We contacted these individuals by phone 1 week after their pantry visit. The study was reviewed and approved by the University of Arizona Institutional Review Board (#00004165).
One author (A.H.), a medical student who was unknown to the clients, interviewed pantry visitors using a semistructured format guided by an interview topic guide (Table 1). He called each participant up to three times to reach them by phone and transcribed interview responses into REDCap (REDCap Consortium). Interviews were not recorded. The senior author (S.B.) is a family physician who has practiced for many years at the Family Medicine Center. He did not interact with the food pantry clients at the time of the food pickup or interview. The interviewees likely were aware that the interviewer was an advocate and supporter of our food pantry model.
We used the editing-organizing style for qualitative analysis.23 We each reviewed the transcriptions first in their entirety. Each of us then highlighted meaningful text segments and made comments about these segments either in the margin of a paper transcript (S.B.) or in a separate column in a spreadsheet (A.H.). We then discussed and compared our comments. We discussed our biases during this iterative process, especially because neither of us have experienced food insecurity and both of us are advocates for a food pantry in a primary care clinic. We each identified themes within our transcript comments and reached consensus on which themes were most important to understanding the experience of food pantry users.
A total of 204 individuals visited the food pantry during our cross-sectional study. We collected phone numbers for 95 people based on a convenience sample. Forty pantry users could not be interviewed because we were unable to reach them. After three attempts (33), we had the wrong number (3), poor phone connection (2), the participant was hard of hearing (1), or refused consent (1). Six respondents partially completed the interview, and 49 completed the full interview.
Of the 55 patients interviewed, 12 (22%) reported that they were first-time visitors to the food pantry, 30 (55%) had visited two to five times, and 13 (24%) reported visiting more than five times.
Most patients prepared or cooked the food, and very few people discarded food. Fruits and vegetables were among the favorite items of most food pantry users (Table 2). A total of 35 of 49 (71%) reported using 75% or more of the food. Eight participants gave away at least one item to a neighbor or family member.
Qualitative Themes
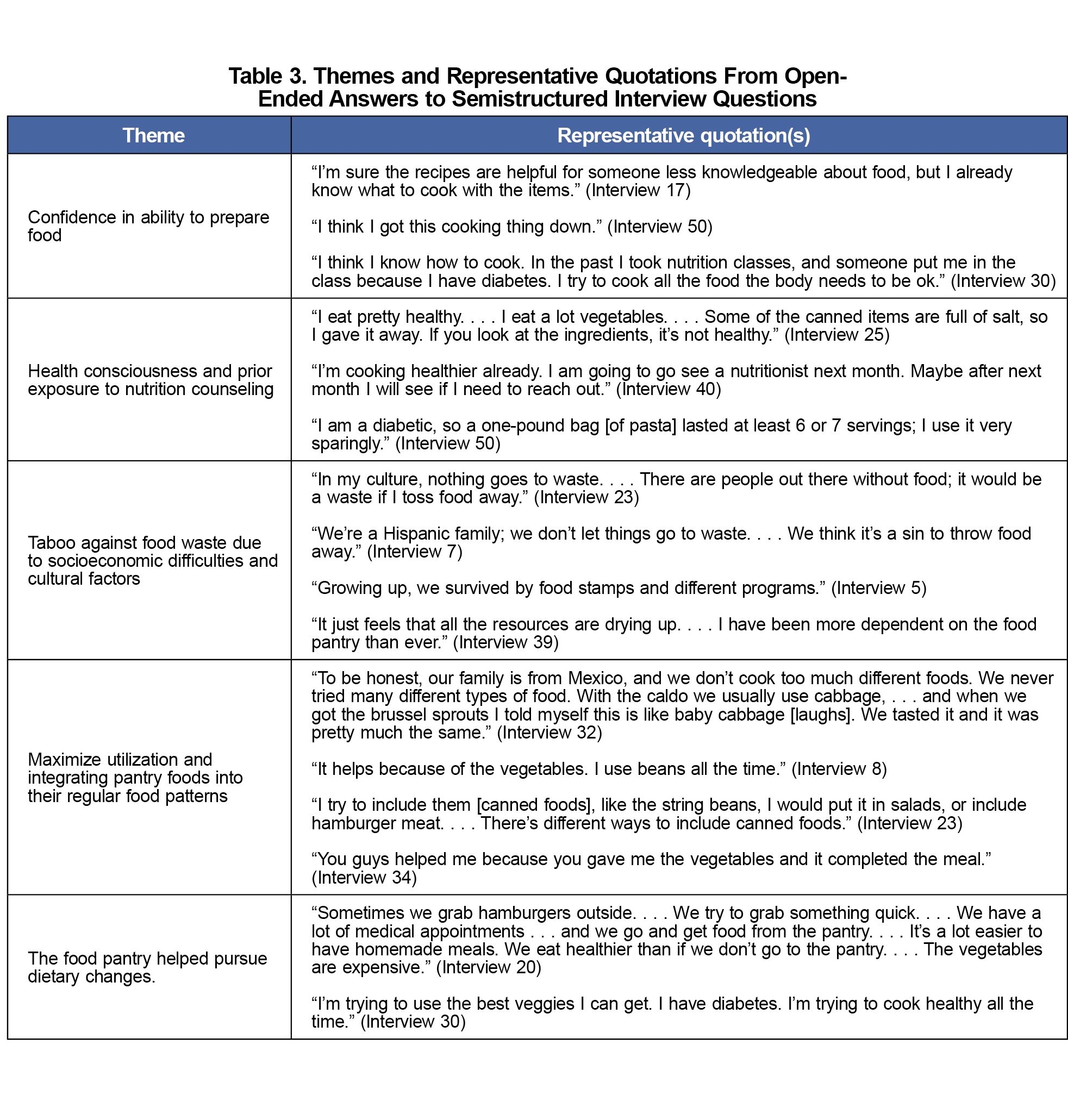
Food pantry users had strong confidence in their own ability to cook or prepare foods, often knowing how to use foods provided and knowing how to integrate foods into their existing diet. They routinely would use the pantry food to supplement meals that were already planned or meals they regularly prepared, including foods that aligned with their cultural preferences.
Visitors to our food pantry rarely wasted food. Many commented that for them to throw away food would be taboo and often cited cultural or economic reasons why throwing away food was not among their values.
Food pantry patrons were aware of healthy food habits and their importance. Some reported that the food pantry would help them make more healthy food choices. See Table 3 for interview themes and representative quotations.
Several of our findings add new information to the literature for clinicians seeking to address food insecurity in a primary care office. Visitors to our in-clinic food pantry are able to use almost all the food provided and prepare most of the items for consumption. Pantry users appreciate fruits and vegetables and are knowledgeable about how to prepare food and how to make healthy choices. Food waste is rare among users of our food pantry. The food pantry is a valued resource for users, recognized both at food pickup22 and after 1 week with the items.
Prior published research has described how people use food from food pantries.24-27 As in our study, pantry patrons appreciate staple items that they already know how to cook, including food that matches existing routines.26 Our respondents reported minimal waste. A client-choice model compared to prepackaged bags may lead to even less waste.27 Our findings confirm prior findings that food pantry clients are seeking healthy food options.24,25
Our study had several limitations. Our convenience sample was nonrandom based on staff availability to gather phone numbers. Food pantry visitors may have answered based on a social desirability bias because they were likely aware that the interviewer was an advocate for our food pantry. Our findings could have been strengthened by collecting demographic data and considering saturation in our analysis. As a single-site study, our findings may not be generalizable to all settings. Further research could apply our approach to other settings and to understanding the benefit of more food choice to align with user preferences.
A food pantry in a residency clinic is feasible, appreciated by users, and can help with nutritious food choices for those in need. Family medicine residencies could use our findings to refine their own design for a food pantry to address food insecurity in their own communities.
Acknowledgments
The authors are grateful to Kreena Patel, MD, MPH, who cofounded the Banner Family Food Pantry in 2023.
Conflict of Interest Statement: The authors have not conflicts of interest to declare.
Presentations:
- Society of Teachers of Family Medicine Annual Spring Conference, May 6, 2025, Salt Lake City, UT
- Arizona Health Equity Conference, October 10, 2024, Phoenix, AZ
- Arizona Academic Family Medicine Innovation Conference, April 4, 2025, Phoenix, AZ
References
- American Academy of Family Physicians. Advancing health equity by addressing social determinants of health in family medicine. AAFP; 2019. Accessed January 30, 2026. https://www.aafp.org/about/policies/all/social-determinants-health-family-medicine-position-paper.html
- Accreditation Council for Graduate Medical Education. ACGME Common Program Requirements (Residency). 2025. Accessed January 30. 2026. https://www.acgme.org/globalassets/pfassets/programrequirements/2025-reformatted-requirements/cprresidency_2025_reformatted.pdf
- Jarris YS, Chang H, Kureshi S, et al. Screening for food insecurity: a curriculum for medical students. PRiMER. 2024;8:9. doi:10.22454/PRiMER.2024.858771
- Cline M, Pagels P, Gimpel N, Day PG. Utilizing home visits to assess social determinants of health during family medicine residency. PRiMER. 2020;4:31. doi:10.22454/PRiMER.2020.448665
- Slupski A. How we measure hunger in America. September 16, 2021. Accessed January 30, 2026. https://www.feedingamerica.org/hunger-blog/how-we-measure-hunger-america
- Sheridan M, Ferrant C. Participation in the women, infants and children (WIC) program: a synthesis of the literature. SciencesPo. 2022. Accessed January 30, 2026. https://sciencespo.hal.science/hal-03521082
- Leung CW, Hoffnagle EE, Lindsay AC, et al. A qualitative study of diverse experts’ views about barriers and strategies to improve the diets and health of Supplemental Nutrition Assistance Program (SNAP) beneficiaries. J Acad Nutr Diet. 2013;113(1):70-76. doi:10.1016/j.jand.2012.09.018
- Bazerghi C, McKay FH, Dunn M. The role of food banks in addressing food insecurity: a systematic review. J Community Health. 2016;41(4):732-740. doi:10.1007/s10900-015-0147-5
- Ginsburg ZA, Bryan AD, Rubinstein EB, et al. Unreliable and difficult-to-access food for those in need: a qualitative and quantitative study of urban food pantries. J Community Health. 2019;44(1):16-31. doi:10.1007/s10900-018-0549-2
- Fong K, Wright RA, Wimer C. The cost of free assistance: why low-income individuals do not access food pantries. J Sociol Soc Welf. 2016;43(1):71-93. doi:10.15453/0191-5096.3999
- Zou F, Sharma L, Pekgün P, Ahire SL. Reducing food waste in U.S. food banks: the role of distribution strategies. Prod Oper Manag. 2025;34(11):3,667-3,685. doi:10.1177/10591478251345133
- De Marchis EH, Torres JM, Benesch T, et al. Interventions addressing food insecurity in health care settings: a systematic review. Ann Fam Med. 2019;17(5):436-447. doi:10.1370/afm.2412
- Acquah OO, Honsvall Hoefler AM, Zoller I, Manning LP, Pine DJ, Mitchell RF. Improving identification of food-insecure patients in an outpatient clinic setting. PRiMER. 2020;4:3. doi:10.22454/PRiMER.2020.115304
- Wright KM, Ravenna P, Wheat S, Villarreal CM, Clements DS, Cronholm PF. Social determinants of health in family medicine residency: a national survey of program directors. Fam Med. 2024;56(2):102-107. doi:10.22454/FamMed.2023.871989
- Heaberlin S, Skelly K, Rosenbaum M, Bunt S. Food insecurity: physician perspectives, screening and communication. PRiMER. 2024;8:38. doi:10.22454/PRiMER.2024.400838
- Kress C, Durvasula J, Knievel A, et al. Patient perspectives: valuable food insecurity interventions. PRiMER. 2021;5:40. doi:10.22454/PRiMER.2021.233359
- Veldheer S, Scartozzi C, Knehans A, et al. A systematic scoping review of how healthcare organizations are facilitating access to fruits and vegetables in their patient populations. J Nutr. 2020;150(11):2,859-2,873. doi:10.1093/jn/nxaa209
- Boston Medical Center. Preventive food pantry. 2024. Accessed January 31, 2026. https://www.bmc.org/nourishing-our-community/preventive-food-pantry
- Greenthal E, Jia J, Poblacion A, James T. Patient experiences and provider perspectives on a hospital-based food pantry: a mixed methods evaluation study. Public Health Nutr. 2019;22(17):3,261-3,269. doi:10.1017/S1368980019002040
- Hickey E, Phan M, Beck AF, Burkhardt MC, Klein MD. A mixed-methods evaluation of a novel food pantry in a pediatric primary care center. Clin Pediatr (Phila). 2020;59(3):278-284. doi:10.1177/0009922819900960
- Reinoso D, Haut D, Claffey S, et al. Addressing food insecurity: lessons learned from co-locating a food pantry with a federally qualified health center. Int J Integr Care. 2022;22(3):24. doi:10.5334/ijic.6430
- Schutz LN, Brown SR. Perspectives from patients using a food pantry in a family medicine residency clinic: a qualitative study. Fam Med. 2024;56(9):584-587. doi:10.22454/FamMed.2024.613582
- Crabtree BF, Miller WL. Doing Qualitative Research. 3rd ed. SAGE; 2022.
- Cooksey-Stowers K, Martin KS, Schwartz M. Client preferences for nutrition interventions in food pantries. J Hunger Environ Nutr. 2019;14(1–2):18-34. doi:10.1080/19320248.2018.1512929
- An R, Wang J, Liu J, Shen J, Loehmer E, McCaffrey J. A systematic review of food pantry-based interventions in the USA. Public Health Nutr. 2019;22(9):1,704-1,716. doi:10.1017/S1368980019000144
- Jones CL, Coffey MC. Consumer choice as experienced in the user-choice food pantry environment: motivations and situational influences on food selection. Public Health Nutr. 2019;22(13):2,479-2,488. doi:10.1017/S1368980019000909
- Pruden B, Poirier L, Gunen B, et al. Client choice distribution model is associated with less leftover food in urban food pantries. Curr Dev Nutr. 2020;4(suppl 2):266. doi:10.1093/cdn/nzaa043_117




There are no comments for this article.