Background and Objectives: Academic promotion is critical in academic medicine. Traditionally, peer-reviewed journal articles have been at the core of advancement deliberations. With the increasing prominence digital content and social media, an increasing number of academics have begun linking their scholarly value with their online activities. It is unclear whether and how US academic medical institutions have updated their promotion criteria to reflect the changing environment and digital practices of faculty members.
Methods: We reviewed publicly available advancement and promotion policies and faculty handbooks of 148 allopathic medical schools in the United States (April 2018 through September 2018), to see if social media was explicitly included in their scholarship criteria.
Results: Of the 148 allopathic institutions only 12 (8.1%) stated that digital and social media products would be factored into the scholarship and/or other domains of the promotion application. There were no associations between acceptability of social media in the tenure process and schools’ characteristics.
Conclusions: Digital media use has the potential to distribute scholarship widely. Including digital scholarship in promotion would help destigmatize the use of digital platforms and promote science dissemination to the public. Medical institutions should embrace new models of digital scholarship and lead the way in defining and ensuring quality.
Academic promotion is critically important to those in academic medicine. The process involves rigorous reviews by committees that generally consider three domains: clinical care, research and education.1-3 Traditionally, scholarly output in the form of peer-reviewed journal articles has been at the core of committee deliberations, looking at publication metrics such as the journal’s prestige (measured by its impact factor), and the number of citations, among others.
Alternative metrics (known as “altmetrics”) seeking to measure the impact of scientific output beyond the academic world,4 are gaining acceptance, as an increasing number of academics contribute to scholarship via digital means: blogs, podcasts, social media, and online publications.5
In 2016, the Mayo Clinic Academic Appointments and Promotions Committee announced that they would be including digital and social media scholarship in academic advancement considerations,6 reflecting a trend of academics who have begun linking their scholarly value with their online activities.7-10
Few studies have evaluated the attitudes of academic leaders about using digital scholarship for promotion, and results have been mixed. A survey of medicine and pediatrics department chairs11 showed that only 23% perceived blogging as an important effort. Other studies showed more positive attitudes towards the use of social media in tenure,4 though concluded (in 2012) that use of social media is “not widely recognized by most research institutions as part of their tenure and promotion review process.”8
Years later, with thousands of physicians engaged in social media, it was still unclear whether academic institutions have updated their promotion criteria to reflect the changing environment and digital practices of faculty members.
We reviewed publicly available promotion policies of 148 allopathic medical schools in the United States between April 2018 and September 2018 to see if digital scholarship or social media were explicitly included in their criteria. Handbooks reviewed were for the 2018-2019 academic period. We reviewed the medical school’s public websites, searched faculty affairs pages for each school’s requirements for promotion and advancement. Search terms included “Web 2.0,” “digital,” “scholarship,” “social media,” “electronic,” “epublication,” “Twitter,” “Facebook,” “(micro)blogs,” and “Podcasts”. Schools with multiple campuses were assessed separately if a unique policy or faculty handbook existed.
Medical schools were grouped into four categories based on explicit inclusion of digital scholarship in advancement policies: explicitly endorsed (group 1); explicitly denied (group 2); ambiguous (group 3); and N/A (group 4). Group 1 schools explicitly stated digital scholarship as factored in advancement considerations; group 2 schools explicitly stated that publications must be peer-reviewed to be considered; group 3 schools stated other non-peer-reviewed electronic media would be considered but did not explicitly state digital scholarship. The N/A category included schools that required a log-in or no policy could be found.
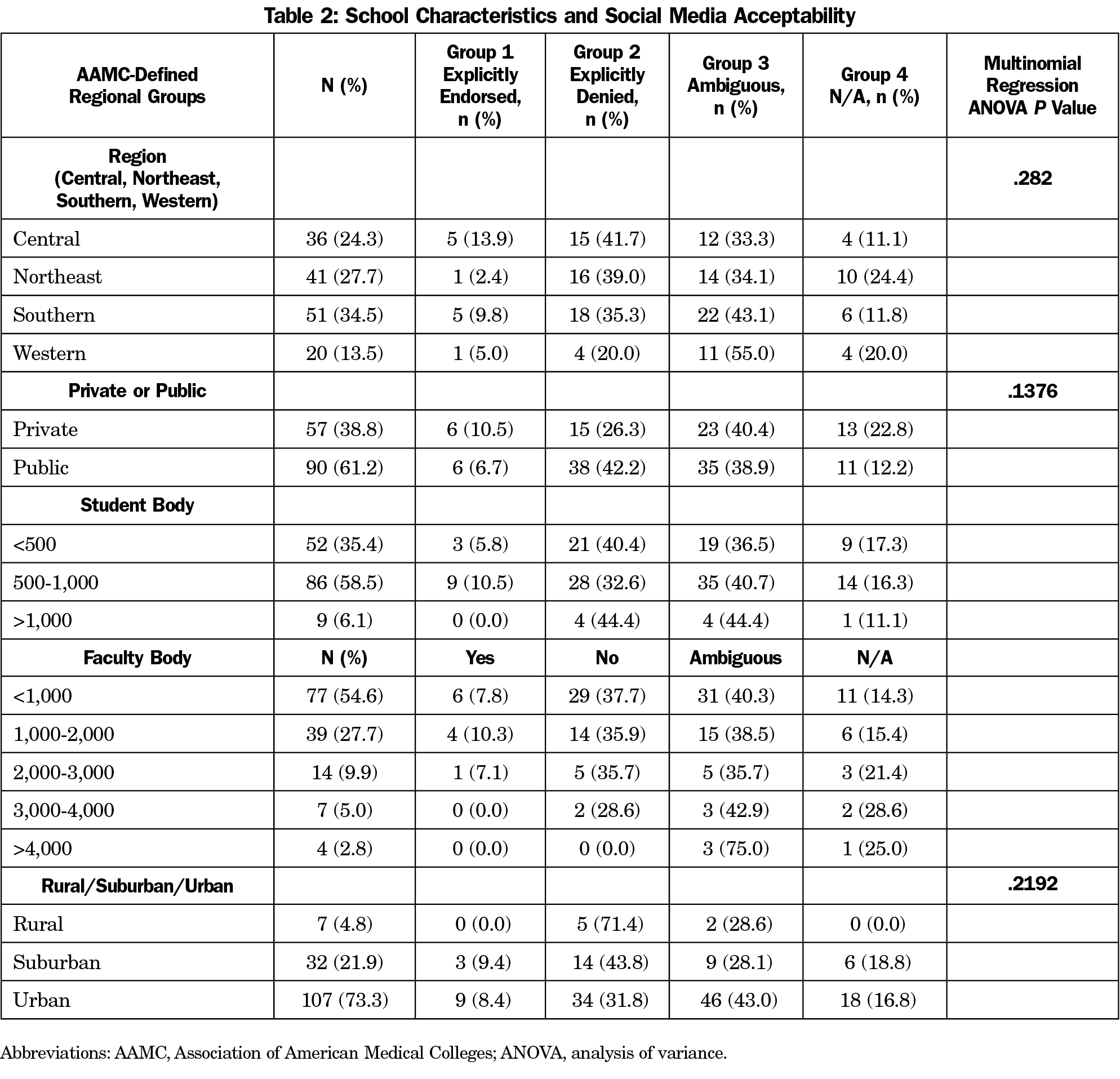
To look for an association between the school’s characteristics (rural/urban, designated region, private/public) and the inclusion of digital scholarship in academic promotion we used multinomial regression with a subsequent analysis of variance (R Core Team; [Software program]; 2020).
Of the 148 allopathic institutions only 12 (8.1%) explicitly endorsed including digital scholarship in advancement. Table 1 Describes the distribution of schools that consider digital scholarship in academic promotion.
Language used to describe digital scholarship in schools that explicitly endorsed it included: “professionally relevant podcasts, blogs, tutorials, or other digital presentations” (Florida International University Herbert Wertheim College of Medicine); “[scholarship includes] popular dissemination of teaching expertise (eg, blogs, webinars, Twitter Chats, etc” (Loyola University Chicago Stritch School of Medicine); “... website/ software development” and “…popular writings/lay press contributes [are not required but will be considered]” (Northwestern University Feinberg School of Medicine); “novel channels for durable dissemination of info (web-based, social media)” (Temple University School of Medicine); “electronic media” (University of Arkansas for Medical Sciences); “contributions to social media with widespread reach” (Washington State University Elson S. Floyd College of Medicine).
Ambiguous schools used the following terms: “creative activities,” “electronic media,” publications would be viewed in the “broadest review,” or items would be reviewed on a “case-by-case basis.” Others did not explicitly state that non-peer-reviewed journals/ digital scholarship/social media would not be included for consideration.
Statistical analyses did not reveal any significant associations between acceptability of digital scholarship and schools’ characteristics. Table 2 describes the school characteristics and digital scholarship acceptability.
Digital scholarship has the potential to disseminate content to peers and colleagues rapidly and efficiently, as well as to members of the public. The importance of such channels of communicating medical and health information has been on display during the COVID-19 pandemic, where scientists from around the world bypassed the long delays of scientific publications and provided critical information through social medial and digital formats. Pre-COVID, such dissemination efforts, however, have rarely been seen as worthy of recognition through academic promotion processes.
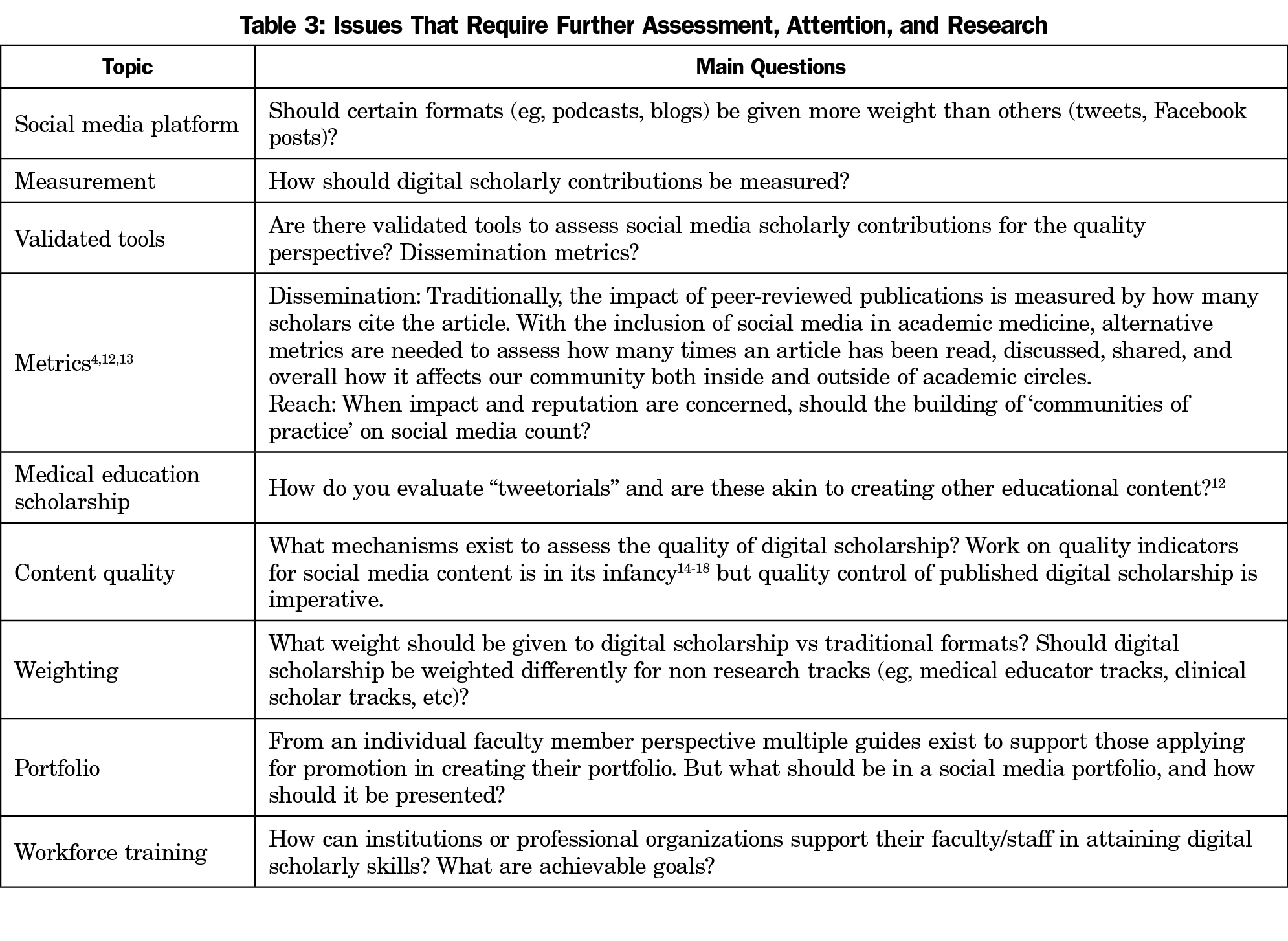
Our descriptive project is the first to show that most medical schools are still using guidelines established nearly 3 decades ago, and only 8% explicitly included digital scholarship as part of promotion considerations. Though the landscape has been changing, it is likely that one of the reasons why so few institutions explicitly endorse digital/social media for promotion is because there is no consensus about what constitutes digital and social media scholarship appropriate for promotion, in terms of which formats merit inclusion, or how to assess quality, though efforts are underway to create benchmarks. Table 3 summarizes open questions medical institutions should consider when developing such promotion criteria.
Including digital scholarship in faculty promotion would reflect growing trends in scholarly dissemination and highlight the importance of public and professional discourse via less traditional and less exclusionary avenues.
Our study has several limitations. First, it was a point-in-time evaluation; it is possible that these policies have changed or are undergoing change since we last reviewed the websites. Schools that explicitly endorsed or were ambiguous to including digital scholarship did not indicate how much weight these publications would hold in promotion decision; 16% of medical schools were categorized as N/A, because we were unable to gain access to their materials, which does not mean that these policies do not exist. Some schools may have internal documents/handbooks that we did not have access to, and therefore it is possible that we mischaracterized the number of institutions that were actually including digital scholarship in their academic promotion criteria.
In recent years other factors have been recognized as important to academic promotion, such as the creation of educational activities, leadership, innovation, quality improvement projects, implementation, and administrative efforts. We believe that the creation of digital content should be included as well, as it represents and captures many of these domains, from creativity and innovation, to leadership to dissemination statistics. We live in a world where the public, multiple stakeholders, and global decision makers rely on information sent and received through digital channels. Doctors, medical educators, and academics have become major players, content creators and curators of health information, and trend setters in highlighting critical issues in medicine and health through social medial and digital formats.19 Medical organizations and conferences have fully embraced the importance of information dissemination through digital and social media channels.20,21
Rather than ignore this reality, medical institutions should lead the way to finding solutions that both recognize the changing landscape of scholarly work, as well as adhere to quality standards.
References
- Bunton SA, Mallon WT. The continued evolution of faculty appointment and tenure policies at U.S. medical schools. Acad Med. 2007;82(3):281-289. doi:10.1097/ACM.0b013e3180307e87
- Buchanan GR. Academic promotion and tenure: a user’s guide for junior faculty members. Hematology Am Soc Hematol Educ Program; 2009:736-741, doi:10.1182/asheducation-2009.1.736
- McGaghie WC. Scholarship, publication, and career advancement in health professions education: AMEE Guide No. 43. Med Teach. 2009;31(7):574-590. doi:10.1080/01421590903050366
- Amath A, Ambacher K, Leddy JJ, Wood TJ, Ramnanan CJ. Comparing alternative and traditional dissemination metrics in medical education. Med Educ. 2017;51(9):935-941. doi:10.1111/medu.13359
- Gruzd A, Staves K, Wilk A. Tenure and promotion in the age of online social media. Proceedings of the American Society for Information Science and Technology. 2011;48(1):1-9. doi:10.1002/meet.2011.14504801154
- Cabrera D. Using Social Media in Academic Promotion. Mayo Clinic Social Media Network. https://socialmedia.mayoclinic.org/2017/08/16/using-social-media-in-academic-promotion/. Published August 16, 2017. Accessed January 5, 2020
- Stukus DR. How I used Twitter to get promoted in academic medicine. KevinMD.com. https://www.kevinmd.com/blog/2016/10/used-twitter-get-promoted-academic-medicine.html. Published October 9, 2016. Accessed February 8, 2018.
- Gruzd A, Staves K, Wilk A. Connected scholars: examining the role of social media in research practices of faculty using the UTAUT model. Comput Human Behav. 2012;28(6):2340-2350. doi:10.1016/j.chb.2012.07.004
- Cabrera D, Roy D, Chisolm MS. Social media scholarship and alternative metrics for academic promotion and tenure. J Am Coll Radiol. 2018;15(1)(1 Pt B):135-141. doi:10.1016/j.jacr.2017.09.012
- Cabrera D, Vartabedian BS, Spinner RJ, Jordan BL, Aase LA, Timimi FK. More than likes and tweets: creating social media portfolios for academic promotion and tenure. J Grad Med Educ. 2017;9(4):421-425. doi:10.4300/JGME-D-17-00171.1
- Cameron CB, Nair V, Varma M, Adams M, Jhaveri KD, Sparks MA. Does Academic Blogging Enhance Promotion and Tenure? A Survey of US and Canadian Medicine and Pediatric Department Chairs. JMIR Med Educ. 2016;2(1):e10. doi:10.2196/mededu.4867
- Ramnanan CJ, Ambacher K, Amath A, O’Brien C, Wood TJ, Leddy JJ. How do alternative and traditional dissemination metrics compare in medical education scholarship? FASEB J. 2016;30(1 Supplement):568.1-568.1.
- Priem J, Hemminger BH. Scientometrics 2.0: new metrics of scholarly impact on the social Web. First Monday. 2010;15(7). http://pear.accc.uic.edu/ojs/index.php/fm/article/view/2874 doi:10.5210/fm.v15i7.2874
- Lin M, Thoma B, Trueger NS, Ankel F, Sherbino J, Chan T. Quality indicators for blogs and podcasts used in medical education: modified Delphi consensus recommendations by an international cohort of health professions educators. Postgrad Med J. 2015;91(1080):546-550. doi:10.1136/postgradmedj-2014-133230
- Thoma B, Chan TM, Kapur P, et al; METRIQ Study Collaborators. The social media index as an indicator of quality for emergency medicine blogs: a METRIQ study. Ann Emerg Med. 2018;72(6):696-702. doi:10.1016/j.annemergmed.2018.05.003
- Thoma B, Sebok-Syer SS, Krishnan K, et al; METRIQ Study Collaborators. Individual gestalt is unreliable for the evaluation of quality in medical education blogs: A METRIQ Study. Ann Emerg Med. 2017;70(3):394-401. doi:10.1016/j.annemergmed.2016.12.025
- Thoma B, Chan TM, Paterson QS, Milne WK, Sanders JL, Lin M. Emergency medicine and critical care blogs and podcasts: establishing an international consensus on quality. Ann Emerg Med. 2015;66(4):396-402.e4. doi:10.1016/j.annemergmed.2015.03.002
- Paterson QS, Thoma B, Milne WK, Lin M, Chan TM. A systematic review and qualitative analysis to determine quality indicators for health professions education blogs and podcasts. J Grad Med Educ. 2015;7(4):549-554. doi:10.4300/JGME-D-14-00728.1
- Mishori R, Singh L, Lin KW, Wei Y. #Diversity: conversations on Twitter about women and black men in medicine. J Am Board Fam Med. 2019;32(1):28-36. doi:10.3122/jabfm.2019.01.180175
- Mishori R, Levy B, Donvan B. Twitter use at a family medicine conference: analyzing #STFM13. Fam Med. 2014;46(8):608-614.
- Mishori R, Singh LO, Levy B, Newport C. Mapping physician Twitter networks: describing how they work as a first step in understanding connectivity, information flow, and message diffusion. J Med Internet Res. 2014;16(4):e107. doi:10.2196/jmir.3006




There are no comments for this article.