Background and Objectives: In response to the COVID-19 pandemic, academic family physicians had to change their clinical, teaching, research, and administrative efforts, while simultaneously balancing their home environment demands. It is unclear how the changes in effort affected physicians’ personal well-being, particularly burnout. This study sought to identify changes in faculty’s clinical, teaching, research, and administrative efforts during the COVID-19 pandemic and how effort shifts were associated with burnout. We also examined associations with important demographics and burnout.
Methods: We took data from the 2020 Council of Academic Family Medicine’s Educational Research Alliance survey of family medicine educators and practicing physicians during November 2020 through December 2020. We analyzed self-report measures of demographics, effort (clinical, teaching, research, and administrative) before and during the pandemic, COVID-19 exposure level, and rates of burnout (emotional exhaustion and depersonalization) using logistic regressions.
Results: Most participants reported no change in efforts. If changes were reported, clinical (21.6%) and administrative (24.8%) efforts tended to increase from before to during the pandemic, while teaching tended to decrease (27.7%). Increases in teaching and clinical efforts were associated with higher rates of emotional exhaustion. Higher depersonalization was associated with increased clinical efforts. Being older and working in a rural setting was associated with lower burnout, while being female was associated with higher burnout.
Conclusions: Shifts in effort across academic family physicians’ multiple roles were associated with emotional exhaustion and, to a lesser degree, depersonalization. The high rates of burnout demand additional attention from directors and administrators, especially among female physicians.
The COVID-19 pandemic has deeply affected individuals and communities across the world. As the epidemic continues, rising levels of emotional distress have been reported in the general population, placing individuals at risk for increased anxiety, depression, and other mental illnesses (eg, posttraumatic stress disorder).1,2 In one survey, over 50% of citizens reported anxiety and psychological distress related to the pandemic.3 Members of the medical community are not immune to the risk of increased psychological distress; medical students reported increased emotional detachment and decreased work performance after the start of the pandemic.4 In the face of rising distress levels, physicians have continued to provide essential services and lifesaving care to patients. Many have reorganized their workplace responsibilities to accomplish these job tasks. It remains unknown how shifts in efforts during the COVID-19 pandemic are associated with physicians’ well-being.
The COVID-19 pandemic coincides with a physician burnout epidemic. In 2017, roughly 50% of family physicians reported symptoms of burnout.5 High levels of burnout may arise from high-volume work expectations, system inefficiencies, and lack of resources for high-quality, equitable care experienced by physicians in clinical practice.6 The pandemic further stressed many health care systems, depleting the available resources of providers and staff, and added risk and uncertainty for everyone. Academic family physicians may be particularly vulnerable to pandemic stress, due to rapid changes in work responsibilities (ie, clinical, teaching, research, and administrative roles) and the requirements of social distancing. In response to COVID-19, many academic institutions implemented policies that fundamentally changed how faculty conducted clinical work, engaged with learners, carried out research, and met administrative requirements.7 Rapidly evolving policies coupled with the demand for clinical patient care were likely drivers of additional pandemic stress within academic family medicine.
In addition to shifts in work responsibilities, the COVID-19 pandemic may have a differential impact on physicians’ burnout based on important demographics. Though COVID-19 appears to pose greater health risk to older individuals,8 studies conducted in Spain and Egypt have found older age is associated with lower levels of physician burnout during the pandemic.9,10 Scholars have theorized that older age is associated with more clinical experience, which serves as a protective factor against burnout.10 Women have been disproportionately impacted by the pandemic, particularly by institutional policies and government mandates forcing shifts in childcare, which culturally is attended to primarily by women, and creating additional pressures on females balancing family and career life.11,12 Such pressures have been linked to increased burnout during the COVID-19 pandemic13; however, no studies have contextualized burnout specific to workplace demands. The rurality of a physician’s practice has inconsistently been associated with burnout, with some scholars finding an increased rate of burnout14 and some finding no difference from prepandemic.15
Rapid shifts in routines, expectations, and roles have been linked with increased risk of burnout in health care workers,16 suggesting that the advent of the COVID-19 pandemic may create additional risk as it has touched almost every area of physicians’ professional and personal lives. Thus, the purpose of this study was to describe how family medicine faculty’s clinical, teaching, research, and administrative efforts shifted during the COVID-19 pandemic, and how the shifts correlated with faculty’s experiences of burnout. Additionally, we examined differences in burnout across demographics and within the context of risk associated with exposure to COVID-19.
We gathered and analyzed data as part of the 2020 Council of Academic Family Medicine’s (CAFM) Educational Research Alliance (CERA) survey of family medicine educators and practicing physicians.17 CAFM is a joint initiative of four major academic family medicine organizations: the Society of Teachers of Family Medicine (STFM), North American Primary Care Research Group (NAPCRG), Association of Departments of Family Medicine (ADFM), and Association of Family Medicine Residency Directors (FMRD). Pretesting, conducted with family medicine educators who were not included in the sampling frame, evaluated questions for flow, timing, and readability, and the final study was approved by the American Academy of Family Physicians (AAFP) Institutional Review Board in November 2020.
Participants were selected based on membership type in one of the CAFM organizations, and program directors, clerkship directors, and department chairs were excluded from the current study as they participated in separate CERA surveys. Qualifying questions were used to ensure that only practicing physicians and educators completed the survey. Invitations to participate in the study included a personalized greeting and a letter signed by the presidents of each of the four sponsoring organizations. A link to the survey via SurveyMonkey was provided to participants. Nonrespondents received four requests to complete the survey, the final request at 2 days before closing the survey.
The survey was distributed to 4,582 candidates. Of the surveys, 177 were returned as undeliverable email addresses and 58 candidates were excluded who had previously opted out of receiving surveys from SurveyMonkey. Additionally, 64 respondents did not meet the qualifying questions and were excluded from further survey questions. The survey was delivered to a final sample of 4,283 family physicians (4,133 US and 215 Canadian) between November 20 and December 15, 2020.
Survey Questions
Demographic questions asked participants to report their self-identified age, gender, racial identity and ethnicity, and community size. Age was captured continuously and was dichotomized into 60 years and older vs less than 60 to assess associations based on an age category associated with increased risk for severe COVID-19 infections. Gender was limited to identification of male or female due to very low cell counts for “other” and “nondisclosed.” We used race to adjust models, but it was not assessed as an independent variable. We based this decision on the poor quality of race variables within the data set. We recoded community size into urban and rural areas based on the US Census Bureau population definitions.18
We created effort change in each role using two items from the demographics section. Participants were asked “In the past year, before the COVID-19 pandemic, from September 2019 to February 2020, what percentage of your time was spent on…” and respondents were prompted to input a percentage of time (0%-100%) spent in undergraduate and graduate teaching, research, clinical, and administrative roles. We totaled undergraduate and graduate teaching efforts to create a respondent’s teaching effort. Participants were instructed to use whole numbers and to make sure that their answers added up to 100. Participants were also asked “Throughout the COVID-19 pandemic, from March 2020 to August 2020, what percentage of your time was spent on…” and were prompted to input a percentage of time for each of the four roles. We constructed new separate variables as the difference in pre-COVID-19 (September 2019-February 2020) and during COVID-19 (March 2020-August 2020) effort variables for reports of clinical, teaching, research, and administrative efforts, with positive scores indicating an increase in effort during COVID-19, negative scores indicating a decrease in effort, and a score of zero indicating no change.
Experience of burnout was assessed using two single-item questions19,20 adapted from the Maslach Burnout Inventory (MBI).21 The first item measured the participants’ emotional exhaustion during the pandemic (“How often do you feel burned out from your work during the COVID-19 pandemic?”). Though this item does not use the phrase “emotional exhaustion,” responses to this question in past research highly correlate to the emotional exhaustion subscale in the full MBI (ρ correlation of .8120), thus the term “emotional exhaustion” will be used herein. The second measured the participants’ depersonalization (“How often do you feel you’ve become more callous toward people during the COVID-19 pandemic?”), measured on a 7-point Likert scale (1=never, 7=every day). Emotional exhaustion and depersonalization were dichotomized to high (scores of ≥4) vs low levels (scores from 1 to 3) of symptom burden, using the cut-off points found in previously published studies.19,20
We assessed COVID-19 exposure risk by asking participants to indicate “What best describes your work-related risk for contracting COVID-19?” Participants indicated one of six levels of risk: “I do no clinical work and can work remotely”; “I do no clinical work but do work some on-site with staff and colleagues”; “I do clinical work and can work remotely”; “I do outpatient clinical work only”; “My work includes inpatient clinical work of patients that generally do not have COVID-19”; or “My work includes inpatient care of COVID-19 patients.” We created categories to indicate lowest (nonclinical or clinical remote work), low (nonclinical work onsite), medium (outpatient and inpatient work with non-COVID-19 patients), and high (ie, COVID inpatient work) risk of COVID-19 exposures.
Analysis
We used descriptive statistics to assess distributions of demographics and reported shifts in efforts (teaching, researching, clinical practice, and administration) during the COVID-19 pandemic. We used logistic regression to compute odds ratios to estimate the associations between dependent (emotional exhaustion and depersonalization) and independent measures (demographics, COVID-19 exposure risk categories, and shifts in effort categories). We used the tab function with χ2 output and expected values to explore associations between effort changes and demographics. We employed a level of statistical significance set at α=0.05 and we used Stata 16 software for the analyses.
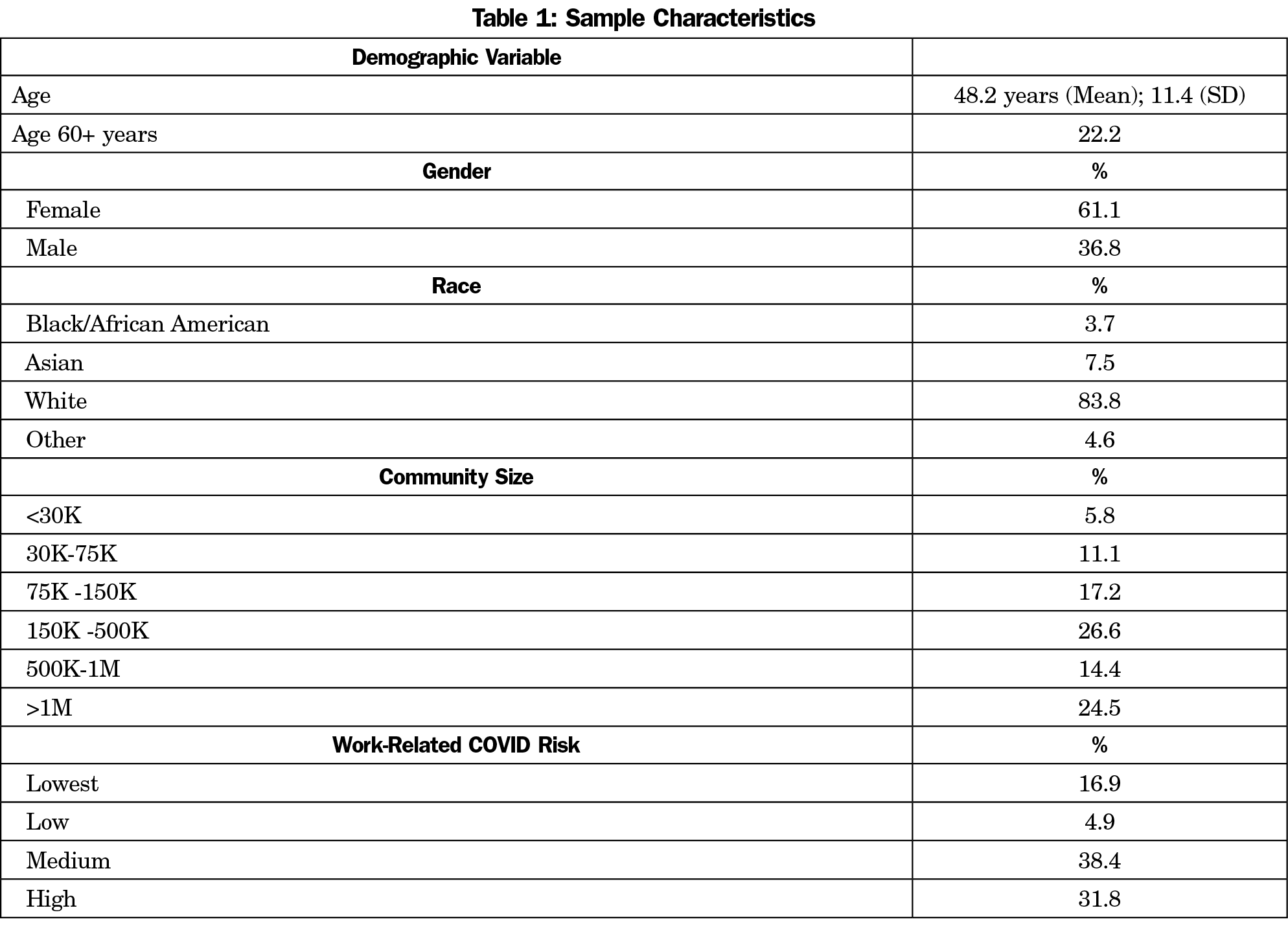
The overall response rate for the survey was 20.13% (862/4283). Within the final sample, response rates for the study questions ranged from 62% (536/862; percent effort in research) to 99% (856/862; gender). Table 1 illustrates the sample characteristics with participants being predominantly White and female. All community sizes were represented, with the largest proportion residing in communities of 150,000-500,000 (26.6%) and the smallest residing in communities of less than 30,000 (5.8%). Work-related COVID-19 exposure categories were relatively evenly distributed, with the low-risk category being the least represented at 4.9%. Rates of both high-level emotional exhaustion and depersonalization were noted in our sample, with 61.1% of respondents reporting high-level emotional exhaustion and 32.8% of respondents reporting high-level depersonalization.
Effort Shifts
“No change” represented the highest proportion of effort adjustment reported during the COVID-19 period compared to the pre-COVID-19 period. More participants reported increases than decreases in clinical and administrative effort categories during the COVID-19 period. Research effort had the lowest proportion of increased effort. Teaching had the largest decrease in effort in the COVID-19 period relative to pre-COVID-19. Table 2 illustrates the proportions of adjustments in effort lines in the COVID-19 period in comparison to the pre-COVID-19 period. During COVID, men were more likely to have no change in research effort (135 vs 120.8 expected), women were more likely to have decreased research effort (111 vs 95.4 expected), and slightly more men had increased research effort (22 vs 20.6 expected) (overall χ2 9.3435; P=.009). No other changes in effort were significantly associated with demographics.
Demographic Associations With Burnout
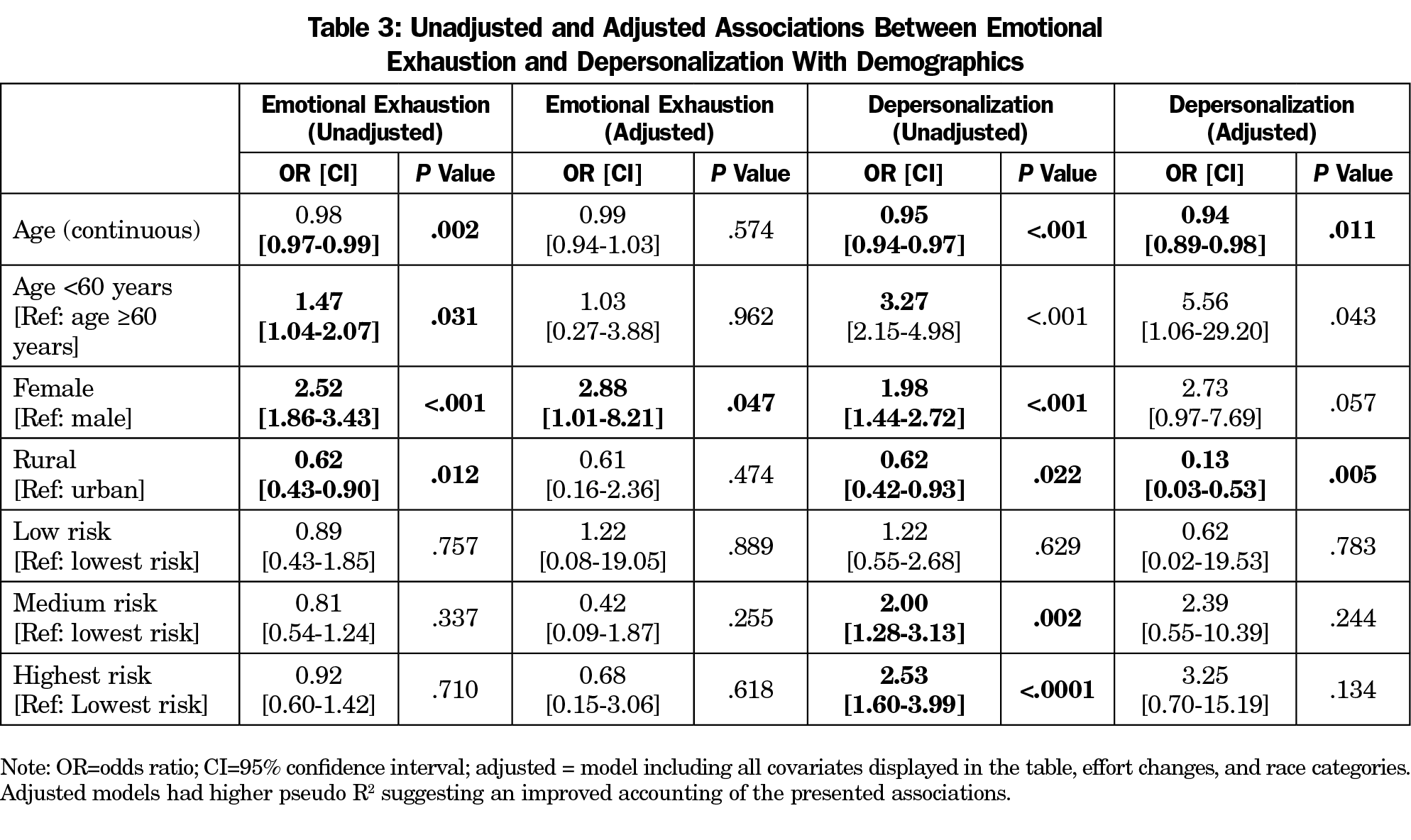
In unadjusted models, increasing age as a continuous variable was associated with significantly fewer reports of high-level emotional exhaustion and depersonalization. Female gender was associated with significantly greater reports of high-level emotional exhaustion and depersonalization. Rural settings were associated with significantly fewer reports of high-level emotional exhaustion and depersonalization. There was a step-wise association with higher levels of COVID-19 risk categories with high levels of depersonalization. When adjusting for all sample characteristics in the model, reports of high levels of emotional exhaustion were only associated with being female, and reports of high levels of depersonalization were only seen with younger age and working in an urban community. Table 3 illustrates unadjusted and adjusted associations between sample characteristics and high-levels of burnout.
Effort Change Associations With Burnout
In unadjusted models, changes in teaching and research efforts (both increases and decreases) and increases in clinical effort were associated with high emotional exhaustion compared to participants with no change in effort. In models adjusted for sample characteristics, decreased clinical and administrative efforts were associated with lower rates of emotional exhaustion compared to participants with no change in effort. Increased clinical and teaching efforts were associated with high emotional exhaustion compared to participants with no change in effort. Only increased clinical effort was associated with high depersonalization. Table 4 illustrates unadjusted and adjusted associations between effort changes and high rates of burnout.
In this study, a significant percentage of family medicine faculty reported high levels of burnout, in terms of both emotional exhaustion (66.5%) and depersonalization (35.7%) during the COVID-19 pandemic, and that burnout was related to shifts in faculty roles. Faculty with moderate to high exposures to COVID-19 reported high depersonalization, but not emotional exhaustion. Women experienced higher rates of burnout and reduced research effort, and older faculty and those in rural settings experienced less burnout.
Most faculty did not report effort shifts across the four roles. For those who did, effort shifts were associated with increased rates of burnout, mostly regarding emotional exhaustion which encompasses the feelings toward oneself and assesses one’s ability to access their personal resiliency.22 Even among faculty reporting no change in effort, high rates of emotional exhaustion (~60% across effort categories) and depersonalization (~30% across effort categories) were noted. Elevated emotional exhaustion has been associated with higher levels of role ambiguity, or confusion in expectations of a role, and role conflict (ie, existing in two or more roles at once) among physicians and nurses at an academic hospital.21 University faculty’s perception of job uncertainties during COVID-19 has been associated with elevated levels of emotional exhaustion.23 We believe that the shifts in teaching, research, and clinical efforts may have left faculty overwhelmed and uncertain about their job expectations, leading to this emotional exhaustion. In light of this, it may be important to increase the level of transparency around the expectations of faculty in each of their roles during times of crisis and/or transitions and how these shifts in expectations will impact tenure and promotion. By doing so, faculty may be better able to understand how these hopefully-short periods of crisis can factor into their long-term career goals and trajectories. Additionally, policies regarding tenure and promotion benchmarks may need to be revisited to address the unique context of COVID-19 and the shifts in efforts expected of academic physicians.
This survey occurred during a time when hospitals required physicians to commit to additional shifts within COVID-19 units as censuses expanded. Faculty who increased their clinical effort or were more exposed to COVID-19 reported more depersonalization. Other studies have found associations between depersonalization and increased hours worked24,25 and work specifically with COVID-19-positive patients.24,26,27 Depersonalization captures the extent to which a participant views patients in a detached or callous way,28 which may serve as a means of insulating physicians from the trauma of caring for COVID-19 patients29 or may be the effect of battling the second pandemic of misinformation and stigma surrounding COVID-19.30 More research is needed to understand whether physicians conceptualize this depersonalization as a sequela of trauma or a protective measure, in relation to clinical work with COVID-19. In the meantime, mental health resources may be able to help address the experience of depersonalization. Universities and hospital systems could partner with local mental health agencies to provide additional support for faculty, either on-site, in the community, or virtually.
Being older or living in a rural area was protective against emotional exhaustion and depersonalization. Increased experience, which may come with older age, increases one’s feelings of competency and self-efficacy and lowers one’s risk of burnout.31 Older physicians in the study may have felt capable of handling changes in clinical efforts or may have had prior experience with high-impact clinical disruptions (eg, SARS, influenza, Ebola, civil unrest, natural disasters), which moderated their feelings of burnout.10 Higher levels of competency may buffer older individuals from burnout in nonclinical roles as well. Further, older physicians, based on their life stage, may not be balancing additional shifts, such as school closures, multiple people living in one home, etc. Another explanation for our findings could be that at the examined stage of the COVID-19 pandemic, rural hospitals may have had fewer patients testing positive,32 and may have sent the most ill patients to larger, more urban health systems, buffering physicians from the intensity of COVID seen in urban settings. Further, the close doctor-patient relationships experienced in many small communities33 can protect against depersonalization. The higher level of emotional exhaustion and depersonalization of women in our study confirms previous findings of increased burnout for female health care workers13 and decreases in research productivity in female faculty during the COVID-19 pandemic.34 Women may be experiencing increased pressure at work as well as at home, as their families may be asking them to coordinate shifts in school and childcare schedules, and manage households where more people are both spending more time and assuming household responsibilities. Despite growth in gender equity, working women take on the brunt of household chores and childcare during the pandemic,35 strengthening the call for policies that support female physicians,36 such as tenure clock extensions, subsidized child- or elder care, or protected time for nonclinical activities.
Limitations and Future Directions
Our data were limited by a response rate of 20%. Although the sample was reasonably mapped to the distribution of geographies and demographics found within American family medicine, it is consistent with other response rates for physician surveys,37,38 and reflects response rates of other 2020 CERA surveys.39-41 The observational nature of this study did not establish causation. The survey asked respondents to reflect globally on effort shifts during the pandemic, but effort adaptations likely varied throughout the pandemic as national policies and this survey only examined one point in time, potentially introducing recall bias. Our data suggest that effort changes during the 2020 period of the pandemic may further exacerbate experiences of burnout. Respondents may have either over- or underinflated responses related to effort change and/or experiences of burnout, introducing social desirability bias. Our study did not examine how the magnitude of change in efforts was associated with the experience of burnout. Future studies are needed to examine whether it is the experience of change or the magnitude of change that creates the greater impact. Our study only inquired about work-related COVID-19 exposure and did not assess for family- or community-related exposure, which also may contribute to feelings of burnout, as well as potential protective factors, such as personal motivations to work in the medical field. Future investigations should examine the larger networks surrounding physicians (eg, community attitudes toward COVID-19, personal motivations, social supports, etc) and how these networks are associated with the experience of burnout.
Academic family physicians have played a pivotal role in health care during the COVID-19 pandemic, yet there appears to be a personal cost for such efforts. Women and faculty who are more immersed in clinical COVID-19 care experience high levels of emotional exhaustion and depersonalization. Academic family medicine leaders should examine work effort policies in this and future pandemics to protect faculty well-being.
References
- Fofana NK, Latif F, Sarfraz S, Bilal, Bashir MF, Komal B. Fear and agony of the pandemic leading to stress and mental illness: an emerging crisis in the novel coronavirus (COVID-19) outbreak. Psychiatry Res. 2020;291:113230. doi:10.1016/j.psychres.2020.113230
- Pfefferbaum B, North CS. Mental health and the Covid-19 pandemic. N Engl J Med. 2020;383(6):510-512. doi:10.1056/NEJMp2008017
- Petzold MB, Bendau A, Plag J, et al. Risk, resilience, psychological distress, and anxiety at the beginning of the COVID-19 pandemic in Germany. Brain Behav. 2020;10(9):e01745. doi:10.1002/brb3.1745
- Meo SA, Abukhalaf AA, Alomar AA, Sattar K, Klonoff DC. COVID-19 pandemic: impact of quarantine on medical students’ mental wellbeing and learning behaviors. Pakistan Journal of Medical Sciences. 2020;36(COVID19-S4):S43.
- Shanafelt TDWC, West CP, Sinsky C, et al. Changes in burnout and satisfaction with work-life integration in physicians and the general US working population between 2011 and 2017. Mayo Clin Proc. 2019;94(9):1681-1694. doi:10.1016/j.mayocp.2018.10.023
- Winner J, Knight C. Beyond burnout: addressing system-induced distress. Fam Pract Manag. 2019;26(5):4-7.
- Ferrel MN, Ryan JJ. The impact of COVID-19 on medical education. Cureus. 2020;12(3):e7492. doi:10.7759/cureus.7492
- Shahid Z, Kalayanamitra R, McClafferty B, et al. COVID‐19 and older adults: what we know. J Am Geriatr Soc. 2020;68(5):926-929. doi:10.1111/jgs.16472
- Ruiz-Fernández MD, Ramos-Pichardo JD, Ibáñez-Masero O, Cabrera-Troya J, Carmona-Rega MI, Ortega-Galán ÁM. Compassion fatigue, burnout, compassion satisfaction and perceived stress in healthcare professionals during the COVID-19 health crisis in Spain. J Clin Nurs. 2020;29(21-22):4321-4330. doi:10.1111/jocn.15469
- Abdelhafiz AS, Ali A, Ziady HH, Maaly AM, Alorabi M, Sultan EA. Prevalence, Associated Factors, and Consequences of Burnout Among Egyptian Physicians During COVID-19 Pandemic. Front Public Health. 2020;8:590190. doi:10.3389/fpubh.2020.590190
- Brubaker L. Women physicians and the COVID-19 pandemic. JAMA. 2020;324(9):835-836. doi:10.1001/jama.2020.14797
- Gabster BP, van Daalen K, Dhatt R, Barry M. Challenges for the female academic during the COVID-19 pandemic. Lancet. 2020;395(10242):1968-1970. doi:10.1016/S0140-6736(20)31412-4
- Sriharan A, Ratnapalan S, Tricco AC, et al. Stress, burnout,, and depression in women in health care during COVID-19 pandemic: rapid scoping review. medRxiv. 2020.
- Rinne ST, Mohr DC, Swamy L, Blok AC, Wong ES, Charns MP. National burnout trends among physicians working in the Department of Veterans Affairs. J Gen Intern Med. 2020;35(5):1382-1388. doi:10.1007/s11606-019-05582-7
- Ward ZD, Morgan ZJ, Peterson LE. Family physician burnout does not differ with rurality. J Rural Health. 2020.
- Peiró JM, González-Romá V, Tordera N, Mañas MA. Does role stress predict burnout over time among health care professionals? Psychol Health. 2001;16(5):511-525. doi:10.1080/08870440108405524
- Seehusen DA, Mainous AG III, Chessman AW. Creating a centralized infrastructure to facilitate medical education research. Ann Fam Med. 2018;16(3):257-260. doi:10.1370/afm.2228
- Ratcliffe M, Burd C, Holder K, Fields A. Defining rural at the US Census Bureau. American community survey and geography brief. 2016;1(8).
- West CP, Dyrbye LN, Sloan JA, Shanafelt TD. Single item measures of emotional exhaustion and depersonalization are useful for assessing burnout in medical professionals. J Gen Intern Med. 2009;24(12):1318-1321. doi:10.1007/s11606-009-1129-z
- Li-Sauerwine S, Rebillot K, Melamed M, Addo N, Lin M. A 2-Question Summative Score Correlates with the Maslach Burnout Inventory. West J Emerg Med. 2020;21(3):610-617. doi:10.5811/westjem.2020.2.45139
- Maslach C, Jackson SE, Leiter MP. The maslach burnout inventory-test manual. Palo Alto. CA: Consulting Psychologists Press; 1996.
- Seidler A, Thinschmidt M, Deckert S, et al. The role of psychosocial working conditions on burnout and its core component emotional exhaustion–a systematic review. J Occup Med Toxicol. 2014;9(1):1-13. doi:10.1186/1745-6673-9-10
- Charoensukmongkol P, Phungsoonthorn T. The effectiveness of supervisor support in lessening perceived uncertainties and emotional exhaustion of university employees during the COVID-19 crisis: the constraining role of organizational intransigence. J Gen Psychol. 2020;•••:1-20. doi:10.1080/00221309.2020.1800582
- Giusti EM, Pedroli E, D’Aniello GE, et al. The psychological impact of the COVID-19 outbreak on health professionals: a cross-sectional study. Front Psychol. 2020;11:1684. doi:10.3389/fpsyg.2020.01684
- Shanafelt TD, West CP, Sinsky C, et al. Changes in burnout and satisfaction with work-life integration in physicians and the general US working population between 2011 and 2017. Paper presented at: Mayo Clinic Proceedings; 2019. doi:10.1016/j.mayocp.2018.10.023
- Kannampallil TG, Goss CW, Evanoff BA, Strickland JR, McAlister RP, Duncan J. Exposure to COVID-19 patients increases physician trainee stress and burnout. PLoS One. 2020;15(8):e0237301. doi:10.1371/journal.pone.0237301
- Morgantini LA, Naha U, Wang H, et al. Factors contributing to healthcare professional burnout during the COVID-19 pandemic: A rapid turnaround global survey. PLoS One. 2020;15(9):e0238217. doi:10.1371/journal.pone.0238217
- Maslach C. Burnout: The cost of caring. Ishk; 2003.
- Raudenská J, Steinerová V, Javůrková A, et al. Occupational burnout syndrome and post-traumatic stress among healthcare professionals during the novel coronavirus disease 2019 (COVID-19) pandemic. Best Pract Res Clin Anaesthesiol. 2020;34(3):553-560. doi:10.1016/j.bpa.2020.07.008
- Bagcchi S. Stigma during the COVID-19 pandemic. Lancet Infect Dis. 2020;20(7):782. doi:10.1016/S1473-3099(20)30498-9
- Shoji K, Cieslak R, Smoktunowicz E, Rogala A, Benight CC, Luszczynska A. Associations between job burnout and self-efficacy: a meta-analysis. Anxiety Stress Coping. 2016;29(4):367-386. doi:10.1080/10615806.2015.1058369
- Wang Y, Liu Y, Struthers J, Lian M. Spatiotemporal characteristics of the COVID-19 epidemic in the United States. Clin Infect Dis. 2021;72(4):643-651. doi:10.1093/cid/ciaa934
- Cameron PJ, Este DC, Worthington CA. Professional, personal and community: 3 domains of physician retention in rural communities. Can J Rural Med. 2012;17(2):47-55.
- Krukowski RA, Jagsi R, Cardel MI. Academic productivity differences by gender and child age in science, technology, engineering, mathematics, and medicine faculty during the COVID-19 pandemic. J Womens Health (Larchmt). 2020.
- Del Boca D, Oggero N, Profeta P, Rossi M. Women’s and men’s work, housework and childcare, before and during COVID-19. Rev Econ Househ. 2020;18(4):1-17. doi:10.1007/s11150-020-09502-1
- Sriharan A, Ratnapalan S, Tricco AC, Lupea D. Women in Health Care Experiencing Occupational Stress and Burnout during COVID-19: A Review. medRxiv. 2021. doi:10.1101/2021.01.08.21249468
- Naylor KB, Tootoo J, Yakusheva O, Shipman SA, Bynum JPW, Davis MA. Geographic variation in spatial accessibility of U.S. healthcare providers. PLoS One. 2019;14(4):e0215016. doi:10.1371/journal.pone.0215016
- Kottke TE, Solberg LI, Conn S, et al. A comparison of two methods to recruit physicians to deliver smoking cessation interventions. Arch Intern Med. 1990;150(7):1477-1481. doi:10.1001/archinte.1990.00390190121019
- Nilsen K, Walling A, Dooley P, Krohn K, Kellerman R, Antoun J. To post or not to post: does applicants’ social media affect family medicine resident recruitment? Fam Med. 2021;53(9):766-772. doi:10.22454/FamMed.2021.292421
- Everard KM, Schiel KZ. Changes in family medicine clerkship teaching due to the COVID-19 pandemic. Fam Med. 2021;53(4):282-284. doi:10.22454/FamMed.2021.583240
- Seehusen DA, Kost A, Barr WB, Theobald M, Harper DM, Eden AR. Family medicine residents’ experience during early phases of the COVID-19 pandemic. PRiMER. 2021;5:18. doi: 10.22454/PRiMER.2021.909862





There are no comments for this article.